U.S. Food and Drug Administration06.22.18
The U.S. Food and Drug Administration today approved the Eversense Continuous Glucose Monitoring (CGM) system for use in people 18 years of age and older with diabetes. This is the first FDA-approved CGM system to include a fully implantable sensor to detect glucose, which can be worn for up to 90 days.
“The FDA is committed to advancing novel products that leverage digital technology to improve patient care,” said FDA Commissioner Scott Gottlieb, M.D. “These technologies allow patients to gain better control over their health. This approval of a more seamless digital system that gives patients the ability to effectively manage a chronic disease like diabetes is a vivid illustration of the potential for these mobile platforms. The FDA is creating a new and more carefully tailored regulatory approach for software products, including mobile medical apps, that will enable efficient oversight of these digital technologies and maintain FDA’s gold standard for product review. We’re advancing a more modern approach for these products that’s carefully adapted to the unique characteristics of these opportunities.”
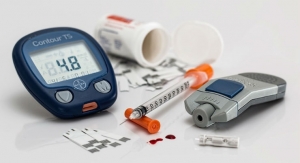
People with diabetes either do not make enough insulin (type 1 diabetes) or cannot use insulin properly (type 2 diabetes). When the body does not have enough insulin, or cannot use it effectively, sugar builds up in the blood. High blood sugar levels can lead to heart disease, stroke, blindness, kidney failure and amputation of toes, feet or legs. Individuals living with diabetes must regularly monitor their glucose levels as part of the management of the disease. This includes making sure that diabetes management accessories, like most current glucose sensors, are replaced on a regular basis (generally, every seven days) to ensure that an overall CGM system is properly functioning.
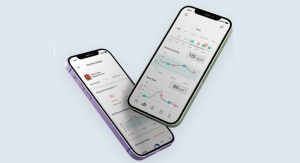
The Eversense CGM system uses a small sensor that is implanted just under the skin by a qualified health care provider during an outpatient procedure. After it is implanted, the sensor regularly measures glucose levels in adults with diabetes for up to 90 days. The implanted sensor works with a novel light-based technology to measure glucose levels and send information to a mobile app to alert users if glucose levels are too high (hyperglycemia) or too low (hypoglycemia). The sensor is coated with a fluorescent chemical which, when exposed to blood sugar, produces a small amount of light that is measured by the sensor. Every five minutes, measurements are sent to a compatible mobile device (e.g., smart phone or tablet) that is running a device-specific mobile app.
The FDA evaluated clinical study data from 125 individuals aged 18 and older with diabetes and reviewed the device’s effectiveness by comparing readings obtained by the Eversense CGM system to those obtained by a laboratory-based glucose analyzer. The safety of the Eversense CGM system’s 90-day implantable sensor, and the procedure used to implant it, was also evaluated during the clinical studies. During these studies, the proportion of individuals experiencing a serious adverse event with the implanted sensor was less than 1 percent. The safety of this novel system will also be evaluated in a post-approval study. The FDA held an Advisory Committee meeting to provide an independent assessment of the safety and effectiveness of the Eversense CGM system. In an 8 to 0 vote, the committee recommended that the benefits of the Eversense CGM system outweigh the risks for patients with diabetes.
Potential adverse effects related to insertion, removal and wear of the sensor include allergic reaction to adhesives, bleeding, bruising, infection, pain or discomfort, scarring or skin discoloration, sensor fracture during removal, skin inflammation, thinning, discoloration or redness. Other risks associated with use of the CGM system may include hypoglycemia or hyperglycemia in cases where information provided by the device is inaccurate or where alerts are missed.
The FDA granted approval of the Eversense Continuous Glucose Monitoring System to Senseonics Inc.
“The FDA is committed to advancing novel products that leverage digital technology to improve patient care,” said FDA Commissioner Scott Gottlieb, M.D. “These technologies allow patients to gain better control over their health. This approval of a more seamless digital system that gives patients the ability to effectively manage a chronic disease like diabetes is a vivid illustration of the potential for these mobile platforms. The FDA is creating a new and more carefully tailored regulatory approach for software products, including mobile medical apps, that will enable efficient oversight of these digital technologies and maintain FDA’s gold standard for product review. We’re advancing a more modern approach for these products that’s carefully adapted to the unique characteristics of these opportunities.”
People with diabetes either do not make enough insulin (type 1 diabetes) or cannot use insulin properly (type 2 diabetes). When the body does not have enough insulin, or cannot use it effectively, sugar builds up in the blood. High blood sugar levels can lead to heart disease, stroke, blindness, kidney failure and amputation of toes, feet or legs. Individuals living with diabetes must regularly monitor their glucose levels as part of the management of the disease. This includes making sure that diabetes management accessories, like most current glucose sensors, are replaced on a regular basis (generally, every seven days) to ensure that an overall CGM system is properly functioning.
The Eversense CGM system uses a small sensor that is implanted just under the skin by a qualified health care provider during an outpatient procedure. After it is implanted, the sensor regularly measures glucose levels in adults with diabetes for up to 90 days. The implanted sensor works with a novel light-based technology to measure glucose levels and send information to a mobile app to alert users if glucose levels are too high (hyperglycemia) or too low (hypoglycemia). The sensor is coated with a fluorescent chemical which, when exposed to blood sugar, produces a small amount of light that is measured by the sensor. Every five minutes, measurements are sent to a compatible mobile device (e.g., smart phone or tablet) that is running a device-specific mobile app.
The FDA evaluated clinical study data from 125 individuals aged 18 and older with diabetes and reviewed the device’s effectiveness by comparing readings obtained by the Eversense CGM system to those obtained by a laboratory-based glucose analyzer. The safety of the Eversense CGM system’s 90-day implantable sensor, and the procedure used to implant it, was also evaluated during the clinical studies. During these studies, the proportion of individuals experiencing a serious adverse event with the implanted sensor was less than 1 percent. The safety of this novel system will also be evaluated in a post-approval study. The FDA held an Advisory Committee meeting to provide an independent assessment of the safety and effectiveness of the Eversense CGM system. In an 8 to 0 vote, the committee recommended that the benefits of the Eversense CGM system outweigh the risks for patients with diabetes.
Potential adverse effects related to insertion, removal and wear of the sensor include allergic reaction to adhesives, bleeding, bruising, infection, pain or discomfort, scarring or skin discoloration, sensor fracture during removal, skin inflammation, thinning, discoloration or redness. Other risks associated with use of the CGM system may include hypoglycemia or hyperglycemia in cases where information provided by the device is inaccurate or where alerts are missed.
The FDA granted approval of the Eversense Continuous Glucose Monitoring System to Senseonics Inc.