Business Wire10.17.17
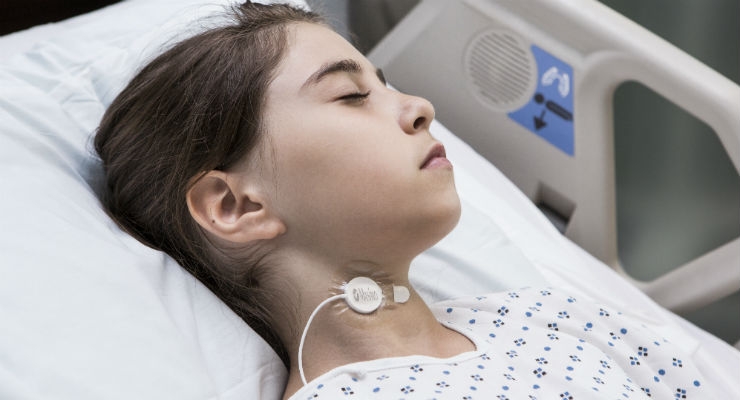
Masimo has announced the full market release of RAS-45, an adhesive adult and pediatric acoustic respiration sensor for rainbow Acoustic Monitoring (RAM). RAS-45 offers the same performance as the currently available RAS-125c sensor but in a smaller size, with more flexible adhesive.
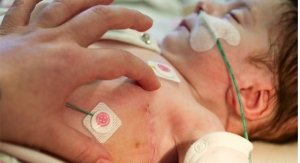
RAM noninvasively and continuously measures respiration rate using an innovative adhesive sensor with an integrated acoustic transducer, such as Masimo’s RAS-125c and now RAS-45, that is applied to the patient’s neck area. Using acoustic signal processing that leverages Masimo Signal Extraction Technology (SET), the respiratory signal is separated and processed to display continuous respiration rate (RRa) and respiratory waveform, with the option to listen to the sound of breathing from the acoustic sensor.
RRa has been shown to be accurate,1,2 easy-to-use,1 easy-to-tolerate,1,3 and reliable,1 and has also been shown to enhance patient compliance with respiration monitoring. In a study comparing pediatric patient tolerance of sidestream capnography with a nasal cannula to respiration rate monitoring with an RAS-125c acoustic sensor, 15 out of 40 patients removed the cannula, while only one removed the acoustic sensor.3 In a study of 98 patients consciously sedated during upper gastrointestinal endoscopy, researchers found that RRa monitoring with the RAS-125c sensor more accurately assessed respiration rate than capnography using end-tidal carbon dioxide (EtCO2) measurement or impedance pneumography.2 RAS-45 maintains the same performance parameters, range, and accuracy specification as RAS-125c.
With its smaller size, RAS-45 is well-suited for monitoring pediatric patients and patients with shorter necks. The RAS-45 adhesive is transparent, lighter, and more flexible than the RAS-125c adhesive. Like RAS-125c, RAS-45 operates with Masimo MX technology boards to measure RRa, display the acoustic respiration wave form, and optionally allow clinicians to listen to the sound of breathing. Both sensors are for adult and pediatric patients who weigh more than 10 kg.
“RAM harnesses the power of our breakthrough signal processing technology and applies it to a respiratory measurement derived from the sound of breathing," said Joe Kiani, dounder and CEO of Masimo. "With the addition of the RAS-45 sensor, RRa is now a more convenient and comfortable measurement for clinicians and patients—especially children.”
Continuous monitoring of respiration rate can be helpful in cases such as sedation-based procedures and post-surgical patients receiving patient-controlled analgesia for pain management. The Anesthesia Patient Safety Foundation and The Joint Commission recommend continuous oxygenation and ventilation (respiration) monitoring for all patients receiving opioid-based pain medications.4,5
References
1. Macknet MR et al. Accuracy and Tolerance of a Novel Bioacoustic Respiratory Sensor in Pediatric Patients Anesthesiology. 2007;107:A84 (abstract).
2. Goudra BG et al. Comparison of Acoustic Respiration Rate, Impedance Pneumography and Capnometry Monitors for Respiration Rate Accuracy and Apnea Detection during GI Endoscopy Anesthesia. Open J Anesthesiol. 2013;3:74-79.
3. Patino M et al. Accuracy of Acoustic Respiration Rate Monitoring in Pediatric Patients. Paediatr Anaesth. 2013 Sep 3.
4. Stoelting, RK et al. APSF newsletter. 2011. www.apsf.org.
5. The Joint Commission Sentinel Event Alert. Issue 49, August 8, 2012. www.jointcomission.org.
Masimo develops noninvasive monitoring technologies. In 1995, the company debuted Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, which has been shown in multiple studies to significantly reduce false alarms and accurately monitor for true alarms. Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,1 improve CCHD screening in newborns,2 and, when used for continuous monitoring with Masimo Patient SafetyNet™* in post-surgical wards, reduce rapid response activations and costs.3,4,5 Masimo SET is estimated to be used on more than 100 million patients in hospitals and other healthcare settings around the world,6 and is the primary pulse oximetry at 16 of the top 20 hospitals listed in the 2017-18 U.S. News and World Report "Best Hospitals Honor Roll."7 In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), and more recently, Oxygen Reserve Index (ORi), in addition to SpO2, pulse rate, and perfusion index (Pi). In 2014, Masimo introduced Root, an intuitive patient monitoring and connectivity platform with the Masimo Open Connect (MOC-9) interface, enabling other companies to augment Root with new features and measurement capabilities. Masimo is also taking an active leadership role in mHealth with products such as the Radius-7 wearable patient monitor, iSpO2 pulse oximeter for smartphones, and the MightySat fingertip pulse oximeter.
ORi has not received U.S. Food and Drug Administration 510(k) clearance and is not available for sale in the United States.
*The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
References
1. Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
2. de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;338.
3. Taenzer AH et al. Impact of Pulse Oximetry Surveillance on Rescue Events and Intensive Care Unit Transfers: A Before-And-After Concurrence Study. Anesthesiology. 2010; 112(2):282-287.
4. Taenzer AH et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
5. McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
6. Estimate: Masimo data on file.
7. http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.
RAM noninvasively and continuously measures respiration rate using an innovative adhesive sensor with an integrated acoustic transducer, such as Masimo’s RAS-125c and now RAS-45, that is applied to the patient’s neck area. Using acoustic signal processing that leverages Masimo Signal Extraction Technology (SET), the respiratory signal is separated and processed to display continuous respiration rate (RRa) and respiratory waveform, with the option to listen to the sound of breathing from the acoustic sensor.
RRa has been shown to be accurate,1,2 easy-to-use,1 easy-to-tolerate,1,3 and reliable,1 and has also been shown to enhance patient compliance with respiration monitoring. In a study comparing pediatric patient tolerance of sidestream capnography with a nasal cannula to respiration rate monitoring with an RAS-125c acoustic sensor, 15 out of 40 patients removed the cannula, while only one removed the acoustic sensor.3 In a study of 98 patients consciously sedated during upper gastrointestinal endoscopy, researchers found that RRa monitoring with the RAS-125c sensor more accurately assessed respiration rate than capnography using end-tidal carbon dioxide (EtCO2) measurement or impedance pneumography.2 RAS-45 maintains the same performance parameters, range, and accuracy specification as RAS-125c.
With its smaller size, RAS-45 is well-suited for monitoring pediatric patients and patients with shorter necks. The RAS-45 adhesive is transparent, lighter, and more flexible than the RAS-125c adhesive. Like RAS-125c, RAS-45 operates with Masimo MX technology boards to measure RRa, display the acoustic respiration wave form, and optionally allow clinicians to listen to the sound of breathing. Both sensors are for adult and pediatric patients who weigh more than 10 kg.
“RAM harnesses the power of our breakthrough signal processing technology and applies it to a respiratory measurement derived from the sound of breathing," said Joe Kiani, dounder and CEO of Masimo. "With the addition of the RAS-45 sensor, RRa is now a more convenient and comfortable measurement for clinicians and patients—especially children.”
Continuous monitoring of respiration rate can be helpful in cases such as sedation-based procedures and post-surgical patients receiving patient-controlled analgesia for pain management. The Anesthesia Patient Safety Foundation and The Joint Commission recommend continuous oxygenation and ventilation (respiration) monitoring for all patients receiving opioid-based pain medications.4,5
References
1. Macknet MR et al. Accuracy and Tolerance of a Novel Bioacoustic Respiratory Sensor in Pediatric Patients Anesthesiology. 2007;107:A84 (abstract).
2. Goudra BG et al. Comparison of Acoustic Respiration Rate, Impedance Pneumography and Capnometry Monitors for Respiration Rate Accuracy and Apnea Detection during GI Endoscopy Anesthesia. Open J Anesthesiol. 2013;3:74-79.
3. Patino M et al. Accuracy of Acoustic Respiration Rate Monitoring in Pediatric Patients. Paediatr Anaesth. 2013 Sep 3.
4. Stoelting, RK et al. APSF newsletter. 2011. www.apsf.org.
5. The Joint Commission Sentinel Event Alert. Issue 49, August 8, 2012. www.jointcomission.org.
Masimo develops noninvasive monitoring technologies. In 1995, the company debuted Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, which has been shown in multiple studies to significantly reduce false alarms and accurately monitor for true alarms. Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,1 improve CCHD screening in newborns,2 and, when used for continuous monitoring with Masimo Patient SafetyNet™* in post-surgical wards, reduce rapid response activations and costs.3,4,5 Masimo SET is estimated to be used on more than 100 million patients in hospitals and other healthcare settings around the world,6 and is the primary pulse oximetry at 16 of the top 20 hospitals listed in the 2017-18 U.S. News and World Report "Best Hospitals Honor Roll."7 In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), and more recently, Oxygen Reserve Index (ORi), in addition to SpO2, pulse rate, and perfusion index (Pi). In 2014, Masimo introduced Root, an intuitive patient monitoring and connectivity platform with the Masimo Open Connect (MOC-9) interface, enabling other companies to augment Root with new features and measurement capabilities. Masimo is also taking an active leadership role in mHealth with products such as the Radius-7 wearable patient monitor, iSpO2 pulse oximeter for smartphones, and the MightySat fingertip pulse oximeter.
ORi has not received U.S. Food and Drug Administration 510(k) clearance and is not available for sale in the United States.
*The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
References
1. Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
2. de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;338.
3. Taenzer AH et al. Impact of Pulse Oximetry Surveillance on Rescue Events and Intensive Care Unit Transfers: A Before-And-After Concurrence Study. Anesthesiology. 2010; 112(2):282-287.
4. Taenzer AH et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
5. McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
6. Estimate: Masimo data on file.
7. http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.