04.29.15
The Journal of the American College of Cardiology: Cardiovascular Interventions has published data from the first clinical experience of Wayne, Pa.-based Intact Vascular Inc.’s Tack Endovascular System. The article, title “Early Experimental and Clinical Experience with a Focal Implant for Lower Extremity Post-Angioplasty Dissection,” reportedly reveals the potential that the Tack Endovascular System offers for the repair of arterial dissections following percutaneous transluminal angioplasty (PTA).
The first-in-human safety and feasibility study with one-year follow up was performed at 2 sites in Asunción, Paraguay (Santa Clara Hospital and The Italian Hospital). Eleven patients with fifteen treated ischemic limbs were enrolled. The 25 treated lesions covered the thigh to the ankle: eight in the superficial femoral artery, seven in the popliteal artery, and ten in the tibial artery. Six of the lesions were occlusions and 19 were stenoses. The number of Tacks implanted per patient averaged 3.4.
Successful dissection repair was achieved at all the lesion sites with the placement of the Tack implant, as determined by angiography. The key endpoints at 12 month follow up included 100 percent repair of dissection flaps. The 12 month patency rates revealed 87.5 percent openness for superficial the femoral artery (SFA) and popliteal vessels, 83.3 percent for SFA, popliteal and tibial vessels, and 80.0 percent for only tibial vessels. There was no limb loss and no implant migration. One target lesion revascularization and death occurred, but according to the company, these were not related to the device or procedure.
“This early clinical experience highlights the potential for a new paradigm in treating peripheral arterial disease that minimizes the metal we leave behind, helps heal the trauma associated with angioplasty, and preserves future treatment options for patients,” said Peter A. Schneider, M.D., vascular surgeon at Kaiser Hospital in Honolulu, Hawaii and chief medical officer of Intact Vascular.
Balloon angioplasty is the most commonly performed peripheral intervention used to improve blood flow in leg arteries. However, suboptimal results frequently occur due to tissue dissection resulting from dilating the artery to restore blood flow. If left untreated, acute or late complications can occur, resulting in re-intervention, tissue loss, or amputation. Stents are currently used to treat dissections; however, stents were not designed to address dissections. Stents involve the implantation of significant amounts of metal, and induce chronic injury and inflammation as a result of applying too much chronic outward force to the vessel wall. Stents permanently alter the structural quality of the artery and limit future treatment options.
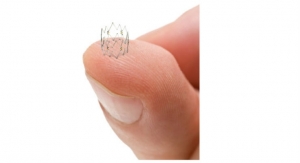
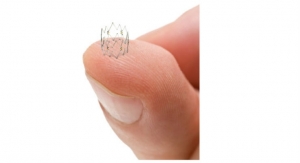
The Tack Endovascular System has been designed to leave minimal foreign material in the artery, apply a low outward force on the arterial wall, and allow “spot” treatment only where needed. To minimize exchanges and increase procedural efficiency, the Tack endovascular delivery catheter contains multiple self-expanding nitinol Tacks. The system is designed to optimize angioplasty by repairing vessel wall dissections, while allowing the artery to maintain its natural configuration.
Schneider added, “The medical community has been looking for treatment options that reduce vessel inflammation and, ultimately, re-occlusion. The recent introduction of drug coated balloons advances the basic angioplasty procedure toward that goal, and the Tack Endovascular System will work to solve the problem of repairing arterial dissections with minimal inflammation. These innovations, taken together, represent the next generation of treatment options for our patients.”
“This early pioneering work, coupled with the recently presented 12 month European TOBA clinical study data, make for a strong foundation as we move forward with the development of this important new approach to treating peripheral arterial disease,” said Bruce Shook, president and CEO of Intact Vascular.
Intact Vascular develops minimally invasive peripheral vascular products.
The first-in-human safety and feasibility study with one-year follow up was performed at 2 sites in Asunción, Paraguay (Santa Clara Hospital and The Italian Hospital). Eleven patients with fifteen treated ischemic limbs were enrolled. The 25 treated lesions covered the thigh to the ankle: eight in the superficial femoral artery, seven in the popliteal artery, and ten in the tibial artery. Six of the lesions were occlusions and 19 were stenoses. The number of Tacks implanted per patient averaged 3.4.
Successful dissection repair was achieved at all the lesion sites with the placement of the Tack implant, as determined by angiography. The key endpoints at 12 month follow up included 100 percent repair of dissection flaps. The 12 month patency rates revealed 87.5 percent openness for superficial the femoral artery (SFA) and popliteal vessels, 83.3 percent for SFA, popliteal and tibial vessels, and 80.0 percent for only tibial vessels. There was no limb loss and no implant migration. One target lesion revascularization and death occurred, but according to the company, these were not related to the device or procedure.
“This early clinical experience highlights the potential for a new paradigm in treating peripheral arterial disease that minimizes the metal we leave behind, helps heal the trauma associated with angioplasty, and preserves future treatment options for patients,” said Peter A. Schneider, M.D., vascular surgeon at Kaiser Hospital in Honolulu, Hawaii and chief medical officer of Intact Vascular.
Balloon angioplasty is the most commonly performed peripheral intervention used to improve blood flow in leg arteries. However, suboptimal results frequently occur due to tissue dissection resulting from dilating the artery to restore blood flow. If left untreated, acute or late complications can occur, resulting in re-intervention, tissue loss, or amputation. Stents are currently used to treat dissections; however, stents were not designed to address dissections. Stents involve the implantation of significant amounts of metal, and induce chronic injury and inflammation as a result of applying too much chronic outward force to the vessel wall. Stents permanently alter the structural quality of the artery and limit future treatment options.
The Tack Endovascular System has been designed to leave minimal foreign material in the artery, apply a low outward force on the arterial wall, and allow “spot” treatment only where needed. To minimize exchanges and increase procedural efficiency, the Tack endovascular delivery catheter contains multiple self-expanding nitinol Tacks. The system is designed to optimize angioplasty by repairing vessel wall dissections, while allowing the artery to maintain its natural configuration.
Schneider added, “The medical community has been looking for treatment options that reduce vessel inflammation and, ultimately, re-occlusion. The recent introduction of drug coated balloons advances the basic angioplasty procedure toward that goal, and the Tack Endovascular System will work to solve the problem of repairing arterial dissections with minimal inflammation. These innovations, taken together, represent the next generation of treatment options for our patients.”
“This early pioneering work, coupled with the recently presented 12 month European TOBA clinical study data, make for a strong foundation as we move forward with the development of this important new approach to treating peripheral arterial disease,” said Bruce Shook, president and CEO of Intact Vascular.
Intact Vascular develops minimally invasive peripheral vascular products.