Michael Barbella, Managing Editor06.04.18
The world is full of Neil Harbissons. So claims billionaire futurist Elon Musk, dreamer extraordinaire and outspoken doomsayer of artificial intelligence who is helming an effort to colonize Mars. Musk contends the Earth’s dominant species has become part cyborg through “machine extensions” of itself (specifically, mobile phones and computers) that are turning human beings into powerful data processing units. “By far you have more power, more capability, than the President of the United States had 30 years ago,” the Tesla and SpaceX CEO told a Future of Life Institute conference audience last year.” If you have an internet link you have an article of wisdom, you can communicate to millions of people, you can communicate to the rest of Earth instantly. I mean, these are magical powers that didn’t exist, not that long ago. So everyone is already superhuman, and a cyborg.”
Indeed we are: The Cyborg Age is well underway, though neither the Web nor social media are entirely responsible for its birth. Increasing numbers of Homo sapiens have become droids, of sorts, in the transcendent quest for eternal youth, beauty, strength, and well-being. As a result, healthcare has become progressively more wired, sensor-filled, and digitally connected: artificial retinas restore sight, cochlear implants augment hearing, deep-brain stimulators (i.e., “brain pacemakers”) treat Parkinson’s disease, and bionic limbs restore movement (and in some cases, feeling) to amputees.
The man-machine merger will likely accelerate over the next decade and a half as technological advances help humankind morph into a cybernetic organism (a living thing both natural and artificial). By 2033, such extraordinary concepts like neuron-strengthening brain chips, implantable wireless video cameras, and cricket ball-sized artificial kidneys could be commonplace.
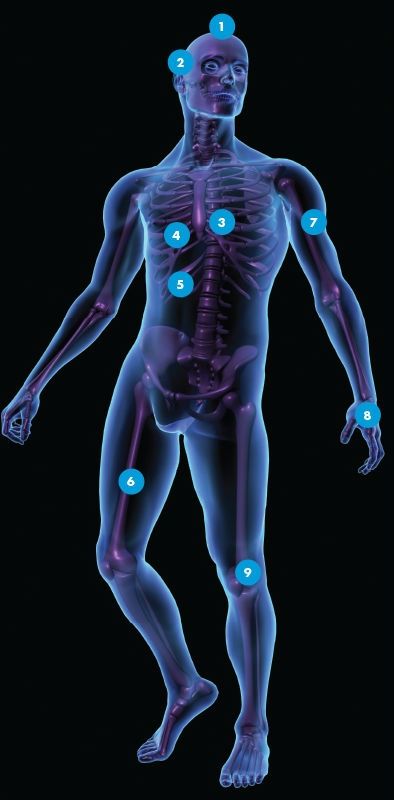
1. BRAIN
 Engineer and distinguished futurist Dr. Ian Pearson expects the human race to soon gain telepathic powers through a global “server” of sorts that interfaces with the brain. Verbal communication be damned (farewell Google and Siri), finding answers to life’s most pressing questions will be just a thought away, as the answer is made available over a network. The best part about this Danny Torrance-like ability? No need for invasive surgery or significant changes to the brain. “It definitely will not be opening up your head sticking a chip in it,” Pearson told Maxim in 2016. “With just an injection...tiny little nanotechnology-based particles will float through your bloodstream across the blood-brain barrier and connect to the neurons themselves. They will be able to pick up electrical signals directly from those neurons and feed them outside into the IT, and your brain basically becomes part of the IT system.” Naysayers take note: Pearson has an 85 percent proven accuracy when looking 10-15 years ahead, and he predicted the rise of text messaging in 1991—long before anyone had ever heard of email.
Engineer and distinguished futurist Dr. Ian Pearson expects the human race to soon gain telepathic powers through a global “server” of sorts that interfaces with the brain. Verbal communication be damned (farewell Google and Siri), finding answers to life’s most pressing questions will be just a thought away, as the answer is made available over a network. The best part about this Danny Torrance-like ability? No need for invasive surgery or significant changes to the brain. “It definitely will not be opening up your head sticking a chip in it,” Pearson told Maxim in 2016. “With just an injection...tiny little nanotechnology-based particles will float through your bloodstream across the blood-brain barrier and connect to the neurons themselves. They will be able to pick up electrical signals directly from those neurons and feed them outside into the IT, and your brain basically becomes part of the IT system.” Naysayers take note: Pearson has an 85 percent proven accuracy when looking 10-15 years ahead, and he predicted the rise of text messaging in 1991—long before anyone had ever heard of email.
2. EYE
Remember the Six Million Dollar Man’s bionic eye? (Didn’t think so, millennials: It was equipped with a telescopic zoom lens). That dream technology is at long last a reality: The U.S. Defense Advanced Research Projects Agency (DARPA) has funded development of a telescopic contact lens that allows users to zoom in and out in literally a wink. The 1.55 mm -thick lens has a larger diameter and more oxygen permeability than typical soft contacts. Developed in tandem with the lens are “smart” eyeglasses that respond to winks (not blinks), thus enabling the user to readily switch between magnified and regular vision (think Clapper for super vision). The lens gives new hope to the 285 million people worldwide suffering from age-related macular degeneration. Diabetics, meanwhile, stand to benefit from a blood glucose-measuring “smart” contact lens designed by Novartis and Google X.
3. HEART
The Temporary Total Artificial Heart (TAH) from Tucson, Ariz.-based SynCardia Systems LLC works just like its biological counterpart—it is pulsatile and consists of two ventricles and four valves that pump blood throughout the body. The battery powered, self-contained TAH is made of special biocompatible plastic, which offers a high degree of fatigue resistance and strength for long-term durability. The company’s 70cc total artificial heart has been implanted in more than 1,700 patients worldwide (one used the system for nearly four years). Still, the TAH is only approved as a temporary solution for those awaiting a transplant.
4. LUNGS
There currently are five bionic lung prototypes in development that can assume the body’s gas exchange duties. One model created at the University of Michigan is roughly the size and shape of a can and has two tubes that attach to the pulmonary artery and patient’s left atrium, respectively. The device has no moving parts, as it relies on the heart to pump blood into a chamber, where oxygen and carbon dioxide are exchanged through a plastic membrane. The oxygen-rich blood is then returned to the body.
5. PANCREAS
Medtronic plc debuted its much-anticipated “artificial pancreas” in the U.S. market last June. The hybrid closed-loop system is the only FDA-approved insulin pump that automatically delivers basal insulin to control blood sugar in patients with Type 1 diabetes. Featuring a glucose sensor to measure blood sugar levels in the fluid directly under the skin, the MiniMed 670G insulin pump and infusion patch delivers insulin through a catheter. An algorithm adjusts the background insulin level every five minutes based on real-time data gathered from the sensor. Although the system is designed to make life easier for diabetics who must constantly manage their blood sugar levels, the MiniMed 670G nevertheless requires patients to track their carbohydrates and manually request bolus insulin at mealtimes. Patients also must calibrate the sensor.
6. BONES
Washington State University researchers have created artificial bone scaffolds through the magic of 3D printing (and a ceramic powder). Using the same printers responsible for producing metal parts found in electric motors, the WSU team covers the ceramic powder with an inkjet layer of plastic binder. The structure is then backed at 2,282 degrees Fahrenheit for 120 minutes and placed into a culture with human bone cells. The scaffold takes to the bone cells within 24 hours.
7. ARMS
“Star Wars” fans will be tickled to learn that Mobius Bionics named its DEKA Arm System after the film’s main protagonist. Approved in 2014, the LUKE Arm provides amputees with a number of new capabilities, including a powered shoulder joint that can reach overhead or behind the back; an elbow strong enough to lift a bag of groceries from floor to tabletop; a wrist with enough range of motion and fine dexterity to hold a glass of water overhead or at waist level without spilling; and a complex hand with four motors that can hold heavy items and delicate ones like an egg without dropping or breaking either. The system has a sensor that also returns “grip-force” information back to the patient, giving feedback about the firmness of his/her grasp. Another new innovation is the use of foot-mounted inertial measurement sensors connected wirelessly to the arm that offer an alternative means of control. The arm decodes signals from the remains of upper limb amputations and translates them into complex motor tasks. The prosthetic is sized and shaped like a human arm and can replace either a complete limb or only the hand and lower arm.
8. HANDS
The i-limb from Manchester, N.H.-based Touch Bionic Inc. is designed to look and move like a natural hand. The prosthetic allows users to program up to 24 grip- and movement-control commands into their smartphones. The robotic appendage functions via myoelectric technology, using small sensors to detect minute muscle movements related to the programmed tasks. A small computer in the i-limb translates those barely-noticeable muscle movements into dozens of precise actions. European researchers, coincidentally, are working on a hand that can actually feel objects. A neural interface provides sensory data from the artificial hand to the brain. The interface links the patient’s nervous system to enhanced sensors embedded in the prosthesis, enabling patients to control complex movements.
9. LEG
The Center for Bionic Medicine at Northwestern University’s Feinberg School of Medicine in Chicago, Ill., has developed the world’s first thought-controlled bionic leg that requires neither nerve redirection surgery nor implanted sensors. An advanced computer program analyzes electromyographic signals (generated by muscle contraction) from sensors on the prosthetic leg. The program decodes the type of attempted movement and then sends those commands simultaneously to the robotic leg’s motorized knee and ankle to produce coordinated movements. Previously, sensors automatically adjusted the angle of the foot during different points in the walker’s stride.
[Author's note: In the June 2018 issue of MPO, this appeared as a sidebar within the 15th Anniversary article, which can be read by clicking here.]
Indeed we are: The Cyborg Age is well underway, though neither the Web nor social media are entirely responsible for its birth. Increasing numbers of Homo sapiens have become droids, of sorts, in the transcendent quest for eternal youth, beauty, strength, and well-being. As a result, healthcare has become progressively more wired, sensor-filled, and digitally connected: artificial retinas restore sight, cochlear implants augment hearing, deep-brain stimulators (i.e., “brain pacemakers”) treat Parkinson’s disease, and bionic limbs restore movement (and in some cases, feeling) to amputees.
The man-machine merger will likely accelerate over the next decade and a half as technological advances help humankind morph into a cybernetic organism (a living thing both natural and artificial). By 2033, such extraordinary concepts like neuron-strengthening brain chips, implantable wireless video cameras, and cricket ball-sized artificial kidneys could be commonplace.
1. BRAIN

2. EYE
Remember the Six Million Dollar Man’s bionic eye? (Didn’t think so, millennials: It was equipped with a telescopic zoom lens). That dream technology is at long last a reality: The U.S. Defense Advanced Research Projects Agency (DARPA) has funded development of a telescopic contact lens that allows users to zoom in and out in literally a wink. The 1.55 mm -thick lens has a larger diameter and more oxygen permeability than typical soft contacts. Developed in tandem with the lens are “smart” eyeglasses that respond to winks (not blinks), thus enabling the user to readily switch between magnified and regular vision (think Clapper for super vision). The lens gives new hope to the 285 million people worldwide suffering from age-related macular degeneration. Diabetics, meanwhile, stand to benefit from a blood glucose-measuring “smart” contact lens designed by Novartis and Google X.
3. HEART
The Temporary Total Artificial Heart (TAH) from Tucson, Ariz.-based SynCardia Systems LLC works just like its biological counterpart—it is pulsatile and consists of two ventricles and four valves that pump blood throughout the body. The battery powered, self-contained TAH is made of special biocompatible plastic, which offers a high degree of fatigue resistance and strength for long-term durability. The company’s 70cc total artificial heart has been implanted in more than 1,700 patients worldwide (one used the system for nearly four years). Still, the TAH is only approved as a temporary solution for those awaiting a transplant.
4. LUNGS
There currently are five bionic lung prototypes in development that can assume the body’s gas exchange duties. One model created at the University of Michigan is roughly the size and shape of a can and has two tubes that attach to the pulmonary artery and patient’s left atrium, respectively. The device has no moving parts, as it relies on the heart to pump blood into a chamber, where oxygen and carbon dioxide are exchanged through a plastic membrane. The oxygen-rich blood is then returned to the body.
5. PANCREAS
Medtronic plc debuted its much-anticipated “artificial pancreas” in the U.S. market last June. The hybrid closed-loop system is the only FDA-approved insulin pump that automatically delivers basal insulin to control blood sugar in patients with Type 1 diabetes. Featuring a glucose sensor to measure blood sugar levels in the fluid directly under the skin, the MiniMed 670G insulin pump and infusion patch delivers insulin through a catheter. An algorithm adjusts the background insulin level every five minutes based on real-time data gathered from the sensor. Although the system is designed to make life easier for diabetics who must constantly manage their blood sugar levels, the MiniMed 670G nevertheless requires patients to track their carbohydrates and manually request bolus insulin at mealtimes. Patients also must calibrate the sensor.
6. BONES
Washington State University researchers have created artificial bone scaffolds through the magic of 3D printing (and a ceramic powder). Using the same printers responsible for producing metal parts found in electric motors, the WSU team covers the ceramic powder with an inkjet layer of plastic binder. The structure is then backed at 2,282 degrees Fahrenheit for 120 minutes and placed into a culture with human bone cells. The scaffold takes to the bone cells within 24 hours.
7. ARMS
“Star Wars” fans will be tickled to learn that Mobius Bionics named its DEKA Arm System after the film’s main protagonist. Approved in 2014, the LUKE Arm provides amputees with a number of new capabilities, including a powered shoulder joint that can reach overhead or behind the back; an elbow strong enough to lift a bag of groceries from floor to tabletop; a wrist with enough range of motion and fine dexterity to hold a glass of water overhead or at waist level without spilling; and a complex hand with four motors that can hold heavy items and delicate ones like an egg without dropping or breaking either. The system has a sensor that also returns “grip-force” information back to the patient, giving feedback about the firmness of his/her grasp. Another new innovation is the use of foot-mounted inertial measurement sensors connected wirelessly to the arm that offer an alternative means of control. The arm decodes signals from the remains of upper limb amputations and translates them into complex motor tasks. The prosthetic is sized and shaped like a human arm and can replace either a complete limb or only the hand and lower arm.
8. HANDS
The i-limb from Manchester, N.H.-based Touch Bionic Inc. is designed to look and move like a natural hand. The prosthetic allows users to program up to 24 grip- and movement-control commands into their smartphones. The robotic appendage functions via myoelectric technology, using small sensors to detect minute muscle movements related to the programmed tasks. A small computer in the i-limb translates those barely-noticeable muscle movements into dozens of precise actions. European researchers, coincidentally, are working on a hand that can actually feel objects. A neural interface provides sensory data from the artificial hand to the brain. The interface links the patient’s nervous system to enhanced sensors embedded in the prosthesis, enabling patients to control complex movements.
9. LEG
The Center for Bionic Medicine at Northwestern University’s Feinberg School of Medicine in Chicago, Ill., has developed the world’s first thought-controlled bionic leg that requires neither nerve redirection surgery nor implanted sensors. An advanced computer program analyzes electromyographic signals (generated by muscle contraction) from sensors on the prosthetic leg. The program decodes the type of attempted movement and then sends those commands simultaneously to the robotic leg’s motorized knee and ankle to produce coordinated movements. Previously, sensors automatically adjusted the angle of the foot during different points in the walker’s stride.
[Author's note: In the June 2018 issue of MPO, this appeared as a sidebar within the 15th Anniversary article, which can be read by clicking here.]