Marc Helberg, Managing Vice President, Pariveda Solutions05.17.19
During the 35-day partial government shutdown—the longest in United States history—we heard a lot about people ransacking national parks, the hundreds of thousands of struggling government workers, and bitter arguments around border wall funding. But one source of contention we didn’t hear as much about was pending U.S. Food and Drug Administration reviews.
At the beginning of 2019, 52 healthcare-focused organizations penned an open letter stating the government shutdown placed medical innovation in peril. Several important new generic drugs, for instance, would take longer to reach market as a direct result of the shutdown.
Their concern was fair, as the government’s drawn-out stall hampered important progress regarding research and review of medical products. Prior to the shutdown, the FDA had discussed incorporating big data and real-world evidence (RWE) into its review process.
Modernizing Medical Device Oversight With RWE
The FDA has good reason to incorporate RWE into these processes as well, as it would serve to improve trial efficiency and cost effectiveness. RWE is a data collection method where valid data is obtained outside the context of randomized controlled trials. It helps organizations make judgements that previously could only be made after extensive clinical trials, which are often expensive and challenging to administer.
Rather than wait for trials to conclude and collect data only on participants, RWE encompasses real-life data from a broader spectrum of sources, including health insurance claims, electronic health records, registries, and personal medical devices. This provides a more comprehensive data set around patients, conditions, and innovative therapies.
Tapping into big data and RWE can help the FDA more accurately gauge the impact new treatments and innovative medical devices could have. That’s because RWE provides data on a broader selection of the patient population and includes longer-term information on the effects of certain types of treatments—both of which should guide the development and review of all future healthcare solutions.
How the FDA Will Move Forward
Both manufacturers and the public are putting pressure on the FDA for fast, safe reviews. Late last year, the International Consortium of Investigative Journalists completed a yearlong investigation that pointed toward medical implants as a potential factor in 80,000 deaths since 2008. This called into question not just the safety of medical devices currently on the market, but also the robustness of FDA reviews.
The FDA has since launched its Medical Device Safety Action Plan, which will ultimately seek to overhaul the process of reviewing medical devices before they hit the market. This also included the launch of the National Evaluation System for Health Technology (NEST). According to the FDA, NEST aims to “generate evidence across the total product lifecycle of medical devices by strategically and systematically leveraging real-world evidence and applying advanced analytics to data tailored to the unique data needs and innovation cycles of medical devices.”
Until recently, manufacturers often sought quick clearance for their devices by claiming they were equivalent to ones previously cleared. The pathway for expedited clearance, known as a 510(k) clearance process, began in 1976. In some cases, new products and devices were cleared based on comparisons to old technology.
Unsurprisingly, this led to claims that cleared devices weren’t vetted thoroughly enough, and manufacturers bore the brunt of that. Lawsuits against companies and products—such as those filed against pelvic mesh manufacturers—scare patients away, making it harder for them to receive effective treatment for their conditions.
Achieving Faster, Safer Clearance
This combination of shaky comparisons and limited clinical knowledge have created a system that’s no longer relevant in today’s healthcare market. A better one would include predicates based on current technology, greater levels of clinical trial activity, and plenty of RWE to verify product safety and effectiveness. As the FDA’s clearance system moves toward the future, medical device manufacturers should follow in kind.
Following are three important factors for manufacturers to consider when working with new review systems.
1. Continue pushing comparisons to newer technology
Updating predicates is one of the most important goals of the FDA’s overhaul. According to Modern Healthcare, nearly 80 percent of devices on the market go through the 510(k) process, and almost 20 percent of those are cleared based on technology that’s at least a decade old. To quell this problem and increase trust, medical manufacturers should base their applications on up-to-date predicates.
Overhauling the process will reduce the risks of new, fast-tracked products failing in the field and can lessen manufacturer vulnerability if a product does fail.
2. Implement technology processes during research and development to fast-track new products
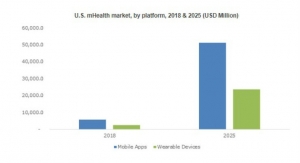
As part of the push for newer predicates, the FDA recently created a specific fast-track for clearing technologies created by Apple, Samsung Electronics, Fitbit, and several other notable companies that manufacture wearables. The goal of the “Pre-Cert for Software Pilot,” as it’s called, is to help promote faster review of health-related technology products that meet a higher, more modern standard.
These tech-first principles could be carried over to the medical device manufacturing side.
3. Leverage artificial intelligence during diagnostics and R&D
Using RWE in the R&D process is another significant step in overhauling the review process, especially when extensive clinical data isn’t available.
More physicians, patients, and regulators accept RWE as a valid basis for decision-making, and using the right AI-based software during the R&D process can help manufacturers ensure their products align with the most relevant RWE data.
Conclusion
The FDA—along with its NEST and RWE initiatives—is meant to protect patient safety. Part of this involves streamlining evaluations for new medical devices. For the initiative to work and for manufacturers and patients to thrive under it, though, companies and regulatory agencies should work in tandem to modernize the review process.
Marc Helberg is the managing vice president at the Philadelphia office of Pariveda Solutions, a consulting firm driven to create innovative, growth-oriented, and people-first solutions. (Click here to read more about the work Pariveda Solutions does.) He has extensive expertise delivering strategic initiatives and brings more than 25 years of consulting and industry experience to helping Fortune 100 companies transform their operating models and achieve their business goals. Outside of the office, he enjoys scuba diving, photography, cooking, and playing music.
At the beginning of 2019, 52 healthcare-focused organizations penned an open letter stating the government shutdown placed medical innovation in peril. Several important new generic drugs, for instance, would take longer to reach market as a direct result of the shutdown.
Their concern was fair, as the government’s drawn-out stall hampered important progress regarding research and review of medical products. Prior to the shutdown, the FDA had discussed incorporating big data and real-world evidence (RWE) into its review process.
Modernizing Medical Device Oversight With RWE
The FDA has good reason to incorporate RWE into these processes as well, as it would serve to improve trial efficiency and cost effectiveness. RWE is a data collection method where valid data is obtained outside the context of randomized controlled trials. It helps organizations make judgements that previously could only be made after extensive clinical trials, which are often expensive and challenging to administer.
Rather than wait for trials to conclude and collect data only on participants, RWE encompasses real-life data from a broader spectrum of sources, including health insurance claims, electronic health records, registries, and personal medical devices. This provides a more comprehensive data set around patients, conditions, and innovative therapies.
Tapping into big data and RWE can help the FDA more accurately gauge the impact new treatments and innovative medical devices could have. That’s because RWE provides data on a broader selection of the patient population and includes longer-term information on the effects of certain types of treatments—both of which should guide the development and review of all future healthcare solutions.
How the FDA Will Move Forward
Both manufacturers and the public are putting pressure on the FDA for fast, safe reviews. Late last year, the International Consortium of Investigative Journalists completed a yearlong investigation that pointed toward medical implants as a potential factor in 80,000 deaths since 2008. This called into question not just the safety of medical devices currently on the market, but also the robustness of FDA reviews.
The FDA has since launched its Medical Device Safety Action Plan, which will ultimately seek to overhaul the process of reviewing medical devices before they hit the market. This also included the launch of the National Evaluation System for Health Technology (NEST). According to the FDA, NEST aims to “generate evidence across the total product lifecycle of medical devices by strategically and systematically leveraging real-world evidence and applying advanced analytics to data tailored to the unique data needs and innovation cycles of medical devices.”
Until recently, manufacturers often sought quick clearance for their devices by claiming they were equivalent to ones previously cleared. The pathway for expedited clearance, known as a 510(k) clearance process, began in 1976. In some cases, new products and devices were cleared based on comparisons to old technology.
Unsurprisingly, this led to claims that cleared devices weren’t vetted thoroughly enough, and manufacturers bore the brunt of that. Lawsuits against companies and products—such as those filed against pelvic mesh manufacturers—scare patients away, making it harder for them to receive effective treatment for their conditions.
Achieving Faster, Safer Clearance
This combination of shaky comparisons and limited clinical knowledge have created a system that’s no longer relevant in today’s healthcare market. A better one would include predicates based on current technology, greater levels of clinical trial activity, and plenty of RWE to verify product safety and effectiveness. As the FDA’s clearance system moves toward the future, medical device manufacturers should follow in kind.
Following are three important factors for manufacturers to consider when working with new review systems.
1. Continue pushing comparisons to newer technology
Updating predicates is one of the most important goals of the FDA’s overhaul. According to Modern Healthcare, nearly 80 percent of devices on the market go through the 510(k) process, and almost 20 percent of those are cleared based on technology that’s at least a decade old. To quell this problem and increase trust, medical manufacturers should base their applications on up-to-date predicates.
Overhauling the process will reduce the risks of new, fast-tracked products failing in the field and can lessen manufacturer vulnerability if a product does fail.
2. Implement technology processes during research and development to fast-track new products
As part of the push for newer predicates, the FDA recently created a specific fast-track for clearing technologies created by Apple, Samsung Electronics, Fitbit, and several other notable companies that manufacture wearables. The goal of the “Pre-Cert for Software Pilot,” as it’s called, is to help promote faster review of health-related technology products that meet a higher, more modern standard.
These tech-first principles could be carried over to the medical device manufacturing side.
3. Leverage artificial intelligence during diagnostics and R&D
Using RWE in the R&D process is another significant step in overhauling the review process, especially when extensive clinical data isn’t available.
More physicians, patients, and regulators accept RWE as a valid basis for decision-making, and using the right AI-based software during the R&D process can help manufacturers ensure their products align with the most relevant RWE data.
Conclusion
The FDA—along with its NEST and RWE initiatives—is meant to protect patient safety. Part of this involves streamlining evaluations for new medical devices. For the initiative to work and for manufacturers and patients to thrive under it, though, companies and regulatory agencies should work in tandem to modernize the review process.
Marc Helberg is the managing vice president at the Philadelphia office of Pariveda Solutions, a consulting firm driven to create innovative, growth-oriented, and people-first solutions. (Click here to read more about the work Pariveda Solutions does.) He has extensive expertise delivering strategic initiatives and brings more than 25 years of consulting and industry experience to helping Fortune 100 companies transform their operating models and achieve their business goals. Outside of the office, he enjoys scuba diving, photography, cooking, and playing music.