Business Wire07.02.19
Masimo has announced the results of a study in which clinicians at Peking Union Medical College in Beijing evaluated the ability of noninvasive and continuous hemoglobin monitoring with Masimo SpHb to help clincians estimate when to conduct invasive hemoglobin measurement to detect possible anemia in patients undergoing spine or cytoreductive surgery.1
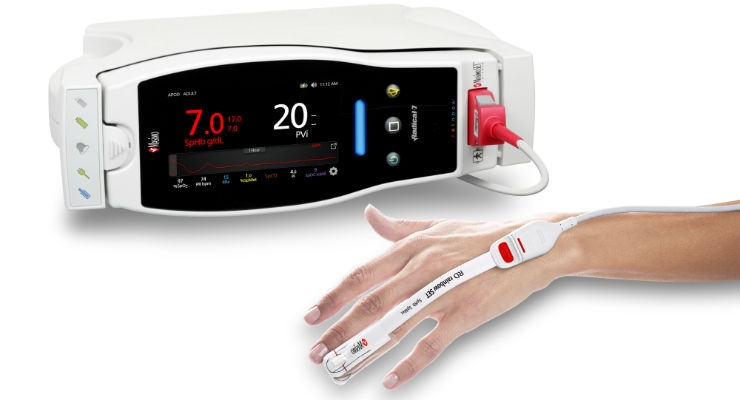
Noting that because of the “invasive, time-consuming and intermittent” nature of invasive blood sampling, clincians often forgo these “objective indications” when making transfusion decisions during surgery, Dr. Tang and colleagues sought to determine whether noninvasive, continuous hemoglobin monitoring could aid clinicians in estimating when it might be appropriate to perform an invasive measurement. They enrolled 69 adult patients scheduled for spine surgery or cytoreductive surgery for whom estimated blood loss was more than 15 percent of total blood volume. The patients were randomly divided into an SpHb group (32 patients) and a standard care group (37 patients). In the SpHb group, diagnostic blood samples were drawn when a patient’s SpHb, measured using a Masimo Radical-7 Pulse CO-Oximeter®, decreased by 1 g/dL. In the standard care group, they were drawn at the clinicians’ discretion.
Blood gas analysis was performed using a Radiometer ABL800. The researchers determined the positive predictive value (PPV) of SpHb for the SpHb group and clinician perception in the standard care group in detecting a decrease in lab hemoglobin of more than 1 g/dL or lab hemoglobin of less than 10 g/dL.
The researchers found that the incidence of unnecessary hemoglobin measurement was lower in the SpHb group than the standard care group. For a decrease of greater than 1 g/dL in lab hemoglobin, SpHb had a PPV of 93.3 percent, compared to 54.5 percent for clinical perception (p = 0.002). For hemoglobin lower than 10 g/dL, SpHb had a PPV of 86.7 percent, compared to 50 percent for clinical perception (p = 0.015). In the SpHb group, lab hemoglobin was never less than 7 g/dL. In addition, using Bland-Altman analysis, the researchers calculated that, compared to lab hemoglobin, SpHb had bias and precision of -0.29 +/- 1.03 g/dL, with limits of agreement of -2.30 and 1.72 g/dL. No difference was observed in transfusion units or postoperative hemoglobin concentrations between the two groups.
The researchers concluded, “The SpHb trend tracked changes in hemoglobin satisfactorily during surgery and more accurately estimated the appropriate timing for invasive hemoglobin measurements than the clinicians.” They also noted that “This study was the first diagnostic randomized controlled trial to explore the triage role of Pulse CO-Oximetry in the intraoperative detection of anemia. We found that the trend in SpHb could detect a decrease in Hb in dynamic situations and indicate the appropriate timing for further Hb measurements.”
Masimo is a global medical technology company that develops and produces monitoring technologies, including measurements, sensors, patient monitors, and automation and connectivity solutions. Its mission is to improve patient outcomes and reduce the cost of care. Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, introduced in 1995, has been shown in over 100 independent and objective studies to outperform other pulse oximetry technologies.2 Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,3 improve CCHD screening in newborns,4 and, when used for continuous monitoring with Masimo Patient SafetyNet in post-surgical wards, reduce rapid response team activations, ICU transfers, and costs.5-7 Masimo SET is estimated to be used on more than 100 million patients in hospitals and other healthcare settings around the world,8 and is the primary pulse oximetry at nine of the top 10 hospitals listed in the 2018-19 U.S. News and World Report Best Hospitals Honor Roll.9 Masimo continues to refine SET and in 2018, announced that SpO2 accuracy on RD SET sensors during conditions of motion has been significantly improved, providing clinicians with even greater confidence that the SpO2 values they rely on accurately reflect a patient’s physiological status. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), RPVi (rainbow PVi), and Oxygen Reserve Index (ORi). In 2013, Masimo introduced the Root Patient Monitoring and Connectivity Platform, built from the ground up to be as flexible and expandable as possible to facilitate the addition of other Masimo and third-party monitoring technologies; key Masimo additions include Next Generation SedLine Brain Function Monitoring, O3 Regional Oximetry, and ISA Capnography with NomoLine sampling lines. Masimo’s family of continuous and spot-check monitoring Pulse CO-Oximeters includes devices designed for use in a variety of clinical and non-clinical scenarios, including tetherless, wearable technology, such as Radius-7, portable devices like Rad-67, fingertip pulse oximeters like MightySat Rx, and devices available for use both in the hospital and at home, such as Rad-97. Masimo hospital automation and connectivity solutions are centered around the Iris platform, and include Iris Gateway, Patient SafetyNet, Replica, Halo ION, UniView, and Doctella.
ORi and RPVi have not received U.S. Food and Drug Administration 510(k) clearance and are not available for sale in the United States. The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
References
1 Tang Bo, Yu X, Xu L, Zhu A, Zhang Y, and Huang Y. Continuous noninvasive hemoglobin monitoring estimates timing for detecting anemia better than clinicians: a randomized controlled trial. BMC Anesthesiology. 17 May 2019. https://doi.org/10.1186/s12871-019-0755-1
2 Published clinical studies on pulse oximetry and the benefits of Masimo SET® can be found on our website at http://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
3 Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
4 de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
5 Taenzer AH et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
6 Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
7 McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
8 Estimate: Masimo data on file.
9 http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.
Noting that because of the “invasive, time-consuming and intermittent” nature of invasive blood sampling, clincians often forgo these “objective indications” when making transfusion decisions during surgery, Dr. Tang and colleagues sought to determine whether noninvasive, continuous hemoglobin monitoring could aid clinicians in estimating when it might be appropriate to perform an invasive measurement. They enrolled 69 adult patients scheduled for spine surgery or cytoreductive surgery for whom estimated blood loss was more than 15 percent of total blood volume. The patients were randomly divided into an SpHb group (32 patients) and a standard care group (37 patients). In the SpHb group, diagnostic blood samples were drawn when a patient’s SpHb, measured using a Masimo Radical-7 Pulse CO-Oximeter®, decreased by 1 g/dL. In the standard care group, they were drawn at the clinicians’ discretion.
Blood gas analysis was performed using a Radiometer ABL800. The researchers determined the positive predictive value (PPV) of SpHb for the SpHb group and clinician perception in the standard care group in detecting a decrease in lab hemoglobin of more than 1 g/dL or lab hemoglobin of less than 10 g/dL.
The researchers found that the incidence of unnecessary hemoglobin measurement was lower in the SpHb group than the standard care group. For a decrease of greater than 1 g/dL in lab hemoglobin, SpHb had a PPV of 93.3 percent, compared to 54.5 percent for clinical perception (p = 0.002). For hemoglobin lower than 10 g/dL, SpHb had a PPV of 86.7 percent, compared to 50 percent for clinical perception (p = 0.015). In the SpHb group, lab hemoglobin was never less than 7 g/dL. In addition, using Bland-Altman analysis, the researchers calculated that, compared to lab hemoglobin, SpHb had bias and precision of -0.29 +/- 1.03 g/dL, with limits of agreement of -2.30 and 1.72 g/dL. No difference was observed in transfusion units or postoperative hemoglobin concentrations between the two groups.
The researchers concluded, “The SpHb trend tracked changes in hemoglobin satisfactorily during surgery and more accurately estimated the appropriate timing for invasive hemoglobin measurements than the clinicians.” They also noted that “This study was the first diagnostic randomized controlled trial to explore the triage role of Pulse CO-Oximetry in the intraoperative detection of anemia. We found that the trend in SpHb could detect a decrease in Hb in dynamic situations and indicate the appropriate timing for further Hb measurements.”
Masimo is a global medical technology company that develops and produces monitoring technologies, including measurements, sensors, patient monitors, and automation and connectivity solutions. Its mission is to improve patient outcomes and reduce the cost of care. Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, introduced in 1995, has been shown in over 100 independent and objective studies to outperform other pulse oximetry technologies.2 Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,3 improve CCHD screening in newborns,4 and, when used for continuous monitoring with Masimo Patient SafetyNet in post-surgical wards, reduce rapid response team activations, ICU transfers, and costs.5-7 Masimo SET is estimated to be used on more than 100 million patients in hospitals and other healthcare settings around the world,8 and is the primary pulse oximetry at nine of the top 10 hospitals listed in the 2018-19 U.S. News and World Report Best Hospitals Honor Roll.9 Masimo continues to refine SET and in 2018, announced that SpO2 accuracy on RD SET sensors during conditions of motion has been significantly improved, providing clinicians with even greater confidence that the SpO2 values they rely on accurately reflect a patient’s physiological status. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), RPVi (rainbow PVi), and Oxygen Reserve Index (ORi). In 2013, Masimo introduced the Root Patient Monitoring and Connectivity Platform, built from the ground up to be as flexible and expandable as possible to facilitate the addition of other Masimo and third-party monitoring technologies; key Masimo additions include Next Generation SedLine Brain Function Monitoring, O3 Regional Oximetry, and ISA Capnography with NomoLine sampling lines. Masimo’s family of continuous and spot-check monitoring Pulse CO-Oximeters includes devices designed for use in a variety of clinical and non-clinical scenarios, including tetherless, wearable technology, such as Radius-7, portable devices like Rad-67, fingertip pulse oximeters like MightySat Rx, and devices available for use both in the hospital and at home, such as Rad-97. Masimo hospital automation and connectivity solutions are centered around the Iris platform, and include Iris Gateway, Patient SafetyNet, Replica, Halo ION, UniView, and Doctella.
ORi and RPVi have not received U.S. Food and Drug Administration 510(k) clearance and are not available for sale in the United States. The use of the trademark Patient SafetyNet is under license from University HealthSystem Consortium.
References
1 Tang Bo, Yu X, Xu L, Zhu A, Zhang Y, and Huang Y. Continuous noninvasive hemoglobin monitoring estimates timing for detecting anemia better than clinicians: a randomized controlled trial. BMC Anesthesiology. 17 May 2019. https://doi.org/10.1186/s12871-019-0755-1
2 Published clinical studies on pulse oximetry and the benefits of Masimo SET® can be found on our website at http://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
3 Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
4 de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
5 Taenzer AH et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
6 Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
7 McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
8 Estimate: Masimo data on file.
9 http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.