GlobeNewswire04.11.18
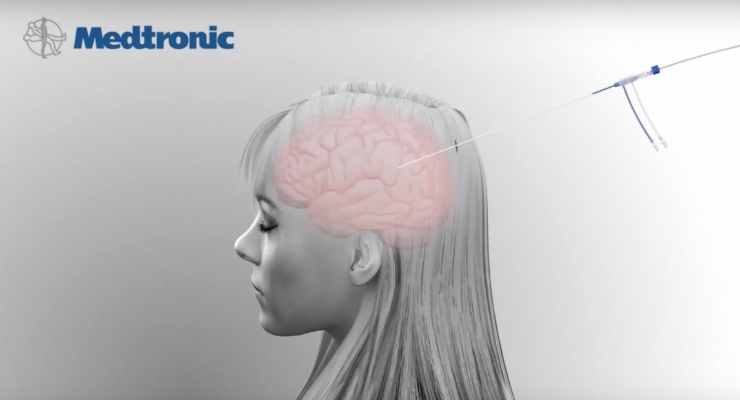
Medtronic plc announced the CE mark and European launch of the Visualase MRI-Guided Laser Ablation System. The Visualase system provides advanced MRI-guided laser ablation technology and can be used in neurosurgery procedures.
With the Visualase system, laser energy is delivered to the target area using an applicator. As light is delivered through the applicator, temperatures in the target area begin to rise, destroying the unwanted soft tissue1. Because Visualase procedures are guided by MRI images, the procedure can provide precise and controlled ablation. Due to the minimally invasive nature of the procedure, patients typically go home the next day.1-10
"The Visualase system will give neurosurgeons an additional minimally invasive option to precisely target and treat small areas of tissue," said Professor Jürgen Voges, M.D., from Magdeburg, Germany. "We are looking forward to offering this procedure to our patients."
The Visualase MRI-Guided Laser Ablation System received Food and Drug Administration (FDA) clearance in the United States in July 2007 to necrotize or coagulate soft tissue. Medtronic is currently involved in a pivotal SLATE (Stereotactic Laser Ablation for Temporal Lobe Epilepsy) study in the United States to support an expanded FDA indication for the treatment of epilepsy in patients with drug-resistant mesial temporal lobe epilepsy (MTLE), the most common form of partial or localization related epilepsy.
"After supporting the FDA clearance with our completion of the first in-human study of the Visualase system in 2006 in Paris, I am excited the technology has arrived in Europe," said Professor Alexandre C. Carpentier, neurosurgeon from Pitie Salpetriere university hospital, Greater Paris University Hospitals - AP-HP of Paris, France.
"The introduction of Visualase to European physicians ensures that more patients will have access to this beneficial technology," said Brett Wall, senior vice president and president of Medtronic's Brain Therapies division, which is part of the Restorative Therapies Group. "This latest milestone is a testament to our commitment to expanding therapeutic options for physicians and their patients."
References
1 Carpentier, A., et. al. Real-time magnetic resonance-guided laser thermal therapy for focal metastatic brain tumors. Neurosurgery July 2008; 63:521-529.
2 Carpentier, A., et. al. MR-guided laser-induced thermal therapy (LITT) for recurrent glioblastomas. Lasers in Surgery and Medicine 2012; 44:361-368.
3 Curry, D., et. al. MR-guided stereotactic laser ablation of epileptogenic foci in children. Epilepsy & Behavior 2012; 24:408-414.
4 Esquanazi, Y., et. al. Stereotactic laser ablation of epileptogenic periventricular nodular heterotopia. Epilepsy Research 2014; 108:547-554.
5 Fabiano, A. and Alberico, R. Laser-interstitial thermal therapy for refractory edema from post-radiosurgery metastasis. World Neurosurgery 2014; 1.E1-1.E4; www.worldneurosurgery.org.
6 Gonzalez-Martinez, J., et. al. Robot-assisted stereotactic laser ablation in medically intractable epilepsy: operative technique. Neurosurgery Publish Ahead of Print 2014; DOI: 10.1227/NEU.0000000000000286.
7 Jethwa, P., et. al. Treatment of a supratentorial primitive neuroectodermal tumor using magnetic resonance-guided laser-induced thermal therapy. J Neurosurg Pediatrics 2011; 8:468-475.
8 Rao, M., et. al. Magnetic resonance-guided laser ablation improves local control for post-radiosurgery recurrence and/or radiation necrosis. Neurosurgery Publish Ahead of Print 2014; DOI: 10.1227/NEU.0000000000000332.
9 Torres-Reveron, J., et. al. Stereotactic laser induced thermotherapy (LITT): a novel treatment for brain lesions regrowing after radiosurgery. J Neuroncol 2013; 113:495-503.
10 Wilfong, A. and Curry, D. Hypothalamic hamartomas: Optimal approach to clinical evaluation and diagnosis. Epilepsia 2013; 54(Suppl. 9): 109-114.
With the Visualase system, laser energy is delivered to the target area using an applicator. As light is delivered through the applicator, temperatures in the target area begin to rise, destroying the unwanted soft tissue1. Because Visualase procedures are guided by MRI images, the procedure can provide precise and controlled ablation. Due to the minimally invasive nature of the procedure, patients typically go home the next day.1-10
"The Visualase system will give neurosurgeons an additional minimally invasive option to precisely target and treat small areas of tissue," said Professor Jürgen Voges, M.D., from Magdeburg, Germany. "We are looking forward to offering this procedure to our patients."
The Visualase MRI-Guided Laser Ablation System received Food and Drug Administration (FDA) clearance in the United States in July 2007 to necrotize or coagulate soft tissue. Medtronic is currently involved in a pivotal SLATE (Stereotactic Laser Ablation for Temporal Lobe Epilepsy) study in the United States to support an expanded FDA indication for the treatment of epilepsy in patients with drug-resistant mesial temporal lobe epilepsy (MTLE), the most common form of partial or localization related epilepsy.
"After supporting the FDA clearance with our completion of the first in-human study of the Visualase system in 2006 in Paris, I am excited the technology has arrived in Europe," said Professor Alexandre C. Carpentier, neurosurgeon from Pitie Salpetriere university hospital, Greater Paris University Hospitals - AP-HP of Paris, France.
"The introduction of Visualase to European physicians ensures that more patients will have access to this beneficial technology," said Brett Wall, senior vice president and president of Medtronic's Brain Therapies division, which is part of the Restorative Therapies Group. "This latest milestone is a testament to our commitment to expanding therapeutic options for physicians and their patients."
References
1 Carpentier, A., et. al. Real-time magnetic resonance-guided laser thermal therapy for focal metastatic brain tumors. Neurosurgery July 2008; 63:521-529.
2 Carpentier, A., et. al. MR-guided laser-induced thermal therapy (LITT) for recurrent glioblastomas. Lasers in Surgery and Medicine 2012; 44:361-368.
3 Curry, D., et. al. MR-guided stereotactic laser ablation of epileptogenic foci in children. Epilepsy & Behavior 2012; 24:408-414.
4 Esquanazi, Y., et. al. Stereotactic laser ablation of epileptogenic periventricular nodular heterotopia. Epilepsy Research 2014; 108:547-554.
5 Fabiano, A. and Alberico, R. Laser-interstitial thermal therapy for refractory edema from post-radiosurgery metastasis. World Neurosurgery 2014; 1.E1-1.E4; www.worldneurosurgery.org.
6 Gonzalez-Martinez, J., et. al. Robot-assisted stereotactic laser ablation in medically intractable epilepsy: operative technique. Neurosurgery Publish Ahead of Print 2014; DOI: 10.1227/NEU.0000000000000286.
7 Jethwa, P., et. al. Treatment of a supratentorial primitive neuroectodermal tumor using magnetic resonance-guided laser-induced thermal therapy. J Neurosurg Pediatrics 2011; 8:468-475.
8 Rao, M., et. al. Magnetic resonance-guided laser ablation improves local control for post-radiosurgery recurrence and/or radiation necrosis. Neurosurgery Publish Ahead of Print 2014; DOI: 10.1227/NEU.0000000000000332.
9 Torres-Reveron, J., et. al. Stereotactic laser induced thermotherapy (LITT): a novel treatment for brain lesions regrowing after radiosurgery. J Neuroncol 2013; 113:495-503.
10 Wilfong, A. and Curry, D. Hypothalamic hamartomas: Optimal approach to clinical evaluation and diagnosis. Epilepsia 2013; 54(Suppl. 9): 109-114.