Business Wire03.14.17
Masimo has announced the availability of the RD SedLine EEG sensor, for use with Masimo SedLine Brain Function Monitoring and compatible with simultaneous use of Masimo O3 Regional Oximetry. SedLine and O3 provide simultaneous monitoring on the Masimo Root monitoring platform, helping to give clinicians more information about the brain.
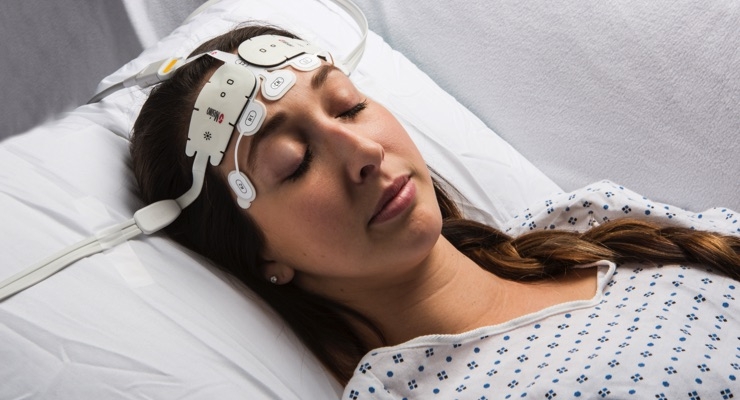
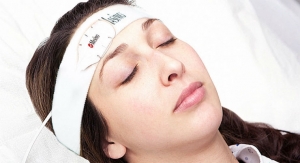
The RD SedLine EEG sensor features a repositioned, color-coded sensor-cable connection that lies comfortably on the patient’s head and soft foam pads to reduce discomfort upon application to the patient. The sensor’s streamlined shape and built-in fitting guide allow simultaneous application of SedLine and O3 sensors. The sensor’s performance and specifications remain the same and work with existing SedLine modules, via an updated patient cable.
SedLine brain function monitoring features four simultaneous EEG leads to enable continuous assessment of both sides of the brain, four EEG waveforms, a Density Spectral Array (DSA; an easy-to-interpret, high-resolution display of bi-hemispheric activity and EEG power), and the Patient State Index (PSI; a processed EEG parameter related to the effect of anesthetic agents). Next Generation SedLine, available outside the U.S., enhances the PSI to make it less susceptible to electromyographic (EMG) interference and to improve performance in low-power EEG cases.
Dr. David Drover, professor of anesthesiology in the Department of Anesthesiology, Perioperative and Pain Medicine at Stanford Hospital (California), stated, “The RD SedLine sensor allows simultaneous application with O3 Regional Oximetry to deliver more information about my patient’s brain in a single specialty monitor.”
O3 regional oximetry uses near-infrared spectroscopy (NIRS) to continuously monitor absolute and trended regional tissue oxygen saturation (rSO2) in the cerebral region. Regional oximetry may help clinicians monitor cerebral oxygenation in situations in which pulse oximetry alone may not be fully indicative of the oxygen in the brain due to various factors, such as the type of clinical procedure being performed.
“Root with SedLine and O3 presents a powerful brain monitoring solution,” said Joe Kiani, founder and CEO of Masimo. “With the addition of the RD SedLine EEG sensor, the EEG and optical sensors fit together like puzzle pieces, making it easier for clinicians to simultaneously monitor patients with both technologies, while providing a comfortable experience for the patient.”
The RD SedLine EEG sensor is available in the United States. Next-generation SedLine does not have 510(k) clearance and is not available in the United States.
Masimo develops noninvasive monitoring technologies. In 1995, the company debuted Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, which has been shown in multiple studies to significantly reduce false alarms and accurately monitor for true alarms. Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,1 improve CCHD screening in newborns,2 and, when used for continuous monitoring in post-surgical wards, reduce rapid response activations and costs.3,4,5 Masimo SET is estimated to be used on more than 100 million patients in leading hospitals and other healthcare settings around the world. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), and more recently, Pleth Variability Index (PVi) and Oxygen Reserve Index (ORi), in addition to SpO2, pulse rate, and perfusion index. Studies with SpHb have shown reductions in unnecessary blood transfusion,*6,7 and when used with PVi, reductions in length of hospital stay8 and 30- and 90-day mortality.9 In 2014, Masimo introduced Root, an intuitive patient monitoring and connectivity platform with the Masimo Open Connect (MOC-9) interface, enabling other companies to augment Root with new features and measurement capabilities. Masimo is also taking an active leadership role in mHealth with products such as the Radius-7 wearable patient monitor, iSpO2 pulse oximeter for smartphones, and the MightySat fingertip pulse oximeter.
*Clinical decisions regarding red blood cell transfusions should be based on the clinician’s judgment considering, among other factors: patient condition, continuous SpHb monitoring, and laboratory diagnostic tests using blood samples.
References
Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;338.
Taenzer AH et al. Impact of Pulse Oximetry Surveillance on Rescue Events and Intensive Care Unit Transfers: A Before-And-After Concurrence Study. Anesthesiology. 2010; 112(2):282-287.
Taenzer AH et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
Ehrenfeld JM et al. Continuous Non-invasive Hemoglobin Monitoring during Orthopedia Surgery: A Randomized Trial. J Blood Disorders Transf. 2014. 5:9. 2.
Awada WN et al. Continuous and noninvasive hemoglobin monitoring reduces red blood cell transfusion during neurosurgery: a prospective cohort study. J Clin Monit Comput. 2015 Feb 4.
Thiele RH et al. Standardization of Care: Impact of an Enhanced Recovery Protocol on Length of Stay, Complications, and Direct Costs after Colorectal Surgery. JACS (2015). doi: 10.1016/j.jamcollsurg.2014.12.042.
Nathan N et al. Impact of Continuous Perioperative SpHb Monitoring. Proceedings from the 2016 ASA Annual Meeting, Chicago. Abstract #A1103.
The RD SedLine EEG sensor features a repositioned, color-coded sensor-cable connection that lies comfortably on the patient’s head and soft foam pads to reduce discomfort upon application to the patient. The sensor’s streamlined shape and built-in fitting guide allow simultaneous application of SedLine and O3 sensors. The sensor’s performance and specifications remain the same and work with existing SedLine modules, via an updated patient cable.
SedLine brain function monitoring features four simultaneous EEG leads to enable continuous assessment of both sides of the brain, four EEG waveforms, a Density Spectral Array (DSA; an easy-to-interpret, high-resolution display of bi-hemispheric activity and EEG power), and the Patient State Index (PSI; a processed EEG parameter related to the effect of anesthetic agents). Next Generation SedLine, available outside the U.S., enhances the PSI to make it less susceptible to electromyographic (EMG) interference and to improve performance in low-power EEG cases.
Dr. David Drover, professor of anesthesiology in the Department of Anesthesiology, Perioperative and Pain Medicine at Stanford Hospital (California), stated, “The RD SedLine sensor allows simultaneous application with O3 Regional Oximetry to deliver more information about my patient’s brain in a single specialty monitor.”
O3 regional oximetry uses near-infrared spectroscopy (NIRS) to continuously monitor absolute and trended regional tissue oxygen saturation (rSO2) in the cerebral region. Regional oximetry may help clinicians monitor cerebral oxygenation in situations in which pulse oximetry alone may not be fully indicative of the oxygen in the brain due to various factors, such as the type of clinical procedure being performed.
“Root with SedLine and O3 presents a powerful brain monitoring solution,” said Joe Kiani, founder and CEO of Masimo. “With the addition of the RD SedLine EEG sensor, the EEG and optical sensors fit together like puzzle pieces, making it easier for clinicians to simultaneously monitor patients with both technologies, while providing a comfortable experience for the patient.”
The RD SedLine EEG sensor is available in the United States. Next-generation SedLine does not have 510(k) clearance and is not available in the United States.
Masimo develops noninvasive monitoring technologies. In 1995, the company debuted Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, which has been shown in multiple studies to significantly reduce false alarms and accurately monitor for true alarms. Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,1 improve CCHD screening in newborns,2 and, when used for continuous monitoring in post-surgical wards, reduce rapid response activations and costs.3,4,5 Masimo SET is estimated to be used on more than 100 million patients in leading hospitals and other healthcare settings around the world. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), and more recently, Pleth Variability Index (PVi) and Oxygen Reserve Index (ORi), in addition to SpO2, pulse rate, and perfusion index. Studies with SpHb have shown reductions in unnecessary blood transfusion,*6,7 and when used with PVi, reductions in length of hospital stay8 and 30- and 90-day mortality.9 In 2014, Masimo introduced Root, an intuitive patient monitoring and connectivity platform with the Masimo Open Connect (MOC-9) interface, enabling other companies to augment Root with new features and measurement capabilities. Masimo is also taking an active leadership role in mHealth with products such as the Radius-7 wearable patient monitor, iSpO2 pulse oximeter for smartphones, and the MightySat fingertip pulse oximeter.
*Clinical decisions regarding red blood cell transfusions should be based on the clinician’s judgment considering, among other factors: patient condition, continuous SpHb monitoring, and laboratory diagnostic tests using blood samples.
References
Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;338.
Taenzer AH et al. Impact of Pulse Oximetry Surveillance on Rescue Events and Intensive Care Unit Transfers: A Before-And-After Concurrence Study. Anesthesiology. 2010; 112(2):282-287.
Taenzer AH et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
Ehrenfeld JM et al. Continuous Non-invasive Hemoglobin Monitoring during Orthopedia Surgery: A Randomized Trial. J Blood Disorders Transf. 2014. 5:9. 2.
Awada WN et al. Continuous and noninvasive hemoglobin monitoring reduces red blood cell transfusion during neurosurgery: a prospective cohort study. J Clin Monit Comput. 2015 Feb 4.
Thiele RH et al. Standardization of Care: Impact of an Enhanced Recovery Protocol on Length of Stay, Complications, and Direct Costs after Colorectal Surgery. JACS (2015). doi: 10.1016/j.jamcollsurg.2014.12.042.
Nathan N et al. Impact of Continuous Perioperative SpHb Monitoring. Proceedings from the 2016 ASA Annual Meeting, Chicago. Abstract #A1103.