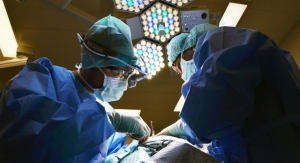
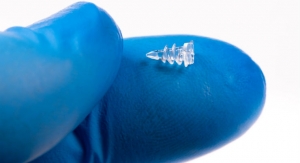
Women who have vaginal surgery to fix a common gynecologic problem, called pelvic organ prolapse (POP), could experience serious problems if mesh is used to repair it, according to a safety communication released by the U.S. Food and Drug Administration (FDA).
The letter urges patients and surgeons to consider other options. The agency will hold an advisory committee meeting in the fall to determine whether to ban the mesh. More than 100,000 women a year with pelvic organ prolapse are treated with plastic mesh, but in most cases, the agency said, the condition “can be treated successfully without mesh.”
"There are clear risks associated with the transvaginal placement of mesh to treat POP," said William Maisel, MD, MPH, deputy director and chief scientist of the FDA's Center for Devices and Radiological Health, in a news release. "The FDA is asking surgeons to carefully consider all other treatment options and to make sure that their patients are fully informed of potential complications from surgical mesh. Mesh is a permanent implant — complete removal may not be possible and may not result in complete resolution of complications."
In 2008, the FDA announced that “rare” problems could be associated with transvaginal placement of the mesh, which is used along with surgical stitches to support sagging pelvic organs such the bladder, uterus, and bowel after they’ve been lifted back out of the vagina where they descended. Mesh-related problems include painful sexual intercourse, infections, urinary problems, overall discomfort, and bleeding usually from the mesh eroding through the stitched tissue or from skin contracting tightly around it.
From 2008 to 2010, the FDA received 1,503 adverse event reports associated with mesh used for POP repair, five times as many as the agency received from 2005 to 2007. It also received three reports of deaths that were related to the mesh placement procedure. Recent studies indicate that about 10 percent of women who have the mesh placed transvaginally experience mesh erosion within 12 months of surgery and that more than half of them require additional surgeries to remove the mesh. Less commonly, the mesh becomes so intertwined with scar tissue that it can’t be removed surgically.
The FDA cited studies showing that abdominal mesh repair for POP led to vaginal erosion in 4 percent of women within 23 months of surgeryEven with today’s FDA announcement, surgeons can still opt to use the mesh for vaginal POP repair, but many may opt not to use it after today’s announcement. The FDA urged patients with the condition to ask their surgeon about all treatment options, including those without mesh, before having the operation.
The FDA cleared the first surgical mesh product specifically for use in stress urinary incontinence in 1996 and for POP in 2002.