Sam Brusco, Associate Editor03.03.22
In-vitro diagnostic (IVD) testing is an extremely diverse market because it spans testing for a variety of diseases and conditions. The introduction of the SARS-CoV-2 virus and resulting COVID-19 disease has made reactionary diagnostic testing for this market the most lucrative sector of the IVD market due to necessity. Diagnostic companies have been reporting massive gains in the COVID-19 testing market as they scramble to ship out the much-needed tests.
But COVID-19 hasn’t just increased the scale and demand for disease testing for pretty much everyone; it’s also spurred adopting more advanced versions of the tests. Hospital systems have begun to purchase PCR (polymerase chain reaction) machines small enough to install in a clinic so samples don’t have to be shipped to a big, centralized lab. This meant patients could get a diagnosis on the spot and isolate immediately afterward. Companies and university researchers working on PCR technologies have reported there’s growing demand for their innovations, like handheld versions that would make testing pretty much anywhere more feasible.
The benefits of this research may extend beyond individual patients. The quick-spreading Omicron variant that emerged in late 2021 showed that testing at the population level was integral to track how COVID-19 might transform and push healthcare systems to a breaking point. The proliferation of PCR testing for COVID-19 could stimulate stronger public health surveillance that can identify future pandemics by testing for dozens of pathogens at one time.
At the time of writing, the U.S. Food and Drug Administration (FDA) has authorized under its emergency use authorization (EUA) over 400 COVID-19 tests and collection kits, comprised of 235 molecular (PCR) tests, 88 antibody tests, and 34 antigen (rapid) tests. Sixty-three of the tests are authorized for home collection, 32 for sample pooling, 55 at the point of care, 19 multi-analyte tests, (COVID-19 and other viruses like the flu), and 13 at-home tests.
PCR testing is considered the gold standard for SARS-CoV-2 detection. The tests detects RNA (or genetic material) specific to the virus via a nasal swab sample and can spot it within days of infection. Turnaround time is generally two to three days but results can arrive in as little as 24 hours. The PCR test is considered the most accurate and reliable test for COVID-19.
Further, once scientists identify new COVID variants they can use PCR testing to track those variants’ spread. Antigen-based methods can’t do this. The Omicron variant’s emergence showed how crucial it was to track variants—data streaming in from PCR tests indicated Omicron was spreading much more quickly compared to its Delta variant predecessor. Because of this data, some governments updated pandemic guidelines and encouraged more booster shots. Some people took the data as a cue to reconsider social interactions and ugrpade their masks’ efficacy as well.
Antigen testing detects protein fragments (antigens) specific to the SARS-CoV-2 virus. It can be done in a clinic, doctor’s office, hospital, or even at home. The turnaround time for antigen test results is usually very quick—because results can be reported in as little as 15 minutes, these tests are also referred to as rapid tests.
In order to boost access to testing, on Jan. 14 the U.S. government purchased 1 billion at-home, rapid COVID-19 tests to give to Americans for free. The tests became available on Jan. 19 and could be mailed directly to U.S. households, with a maximum of four tests per household. The Administration also announced beginning Jan. 15 that private health insurance companies were mandated to cover at-home COVID-19 tests for free and made an additional 10 million tests available to schools nationwide each month.
Medical device and diagnostics firm Abbott Laboratories was and continues to be a significant provider of SARS-CoV-2 diagnostic tests. The firm’s RealTime SARS-CoV-2 molecular test earned FDA emergency use authorization on March 18, 2020. Ten days later the company gained EUA for the ID NOW COVID-19 test, which generates a diagnosis in 13 minutes. In June, EUA was granted for Abbott’s Alinity m molecular lab instrument to test for COVID-19.
An IgG serology test was launched in April 2020, gained EUA a month later, then acquired a CE mark in December 2020. The AdviseDx SARS-CoV-2 IgM antibody test joined the list in October 2020.
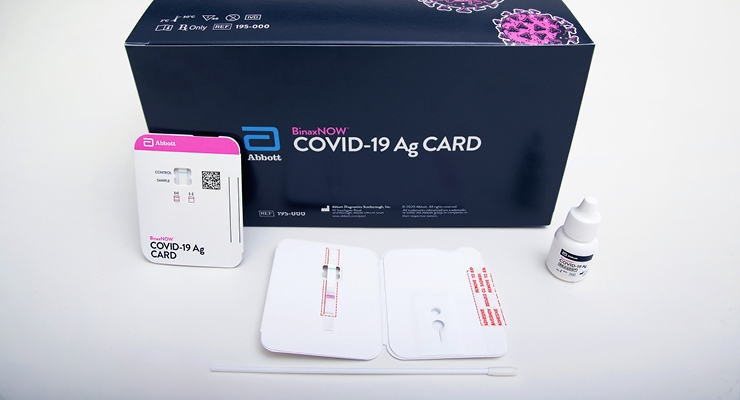
The momentous EUA for the BinaxNow COVID-19 Ag Card—a credit card-sized, five-dollar, 15-minute COVID-19 lateral flow antigen test—came in August 2020. In December 2020, EUA for the test was expanded to virtually-guided home use. Abbott fulfilled the federal government’s order of 150 million tests in January 2021. The test was further expanded to over-the-counter, non-prescription, asymptomatic use in March 2021.
Everyone aged 15 and older are authorized to self-collect samples. Adults can collect samples for children as young as 2. The BinaxNow COVID-19 Ag self-test began shipment to retailers on April 19, 2021.
January 2021 saw a CE mark for the Panbio COVID-19 Ag Rapid test for asymptomatic testing and self-swabbing, supporting mass testing in congregate, asymptomatic populations. A self-test for sale directly to consumers secured CE marking last June.
Abbott CEO Robert Ford joined the White House task force in April 2020 to guide the safe reopening of the U.S. economy. And in March 2021, the company formed the Abbott Pandemic Defense coalition, a global scientific and public health partnership to detect and respond to future pandemic threats. The program aims to connect lab experts, genetic sequencing experts, and public health research experts to identify new pathogens, analyze potential risks, rapidly develop and deploy new diagnostic tests, and assess the impact on public health. That same month the company nabbed EUA for the Alinity m Resp-4-Plex molecular assay, which identifies SARS-CoV-2, influenza A, influenza B, and respiratory syncytial virus in one test.
“We’ve been working 24/7 to scale our operations, producing 70 million tests in January and further scaling toward 100 million a month in March,” an Abbott spokesperson told MPO. “We self-invested to build two new U.S. manufacturing facilities in Maine and Illinois that today employ more than 5,000 people.”
To respond to the variant of concern Omicron, Abbott conducted lab analyses and tests from a live virus, including from the first U.S. Omicron case. BinaxNOW spotted the virus in all tests performed, according to the company, at equal sensitivity as other variants. Data from Abbott customer use did not show a change in test performance, the company reported.
Diagnostics and imaging firm Hologic was also among the first to develop and distribute molecular assays for COVID-19. The company’s Panther Fusion system, which can process up to 1,000 tests in 24 hours, gained FDA emergency use authorization for the Panther Fusion SARS-CoV-2 assay on March 16, 2020. The Biomedical Advanced Research and Development Authority (BARDA) contributed financing to accelerate development of the assay. On May 15, 2020, the firm’s Aptima SARS-CoV-2 assay gained an EUA for the Panther system. In July 2021, the assay secured CE mark was achieved for use of saliva samples.
In September 2020, the Panther Fusion SARS-CoV-2 assay’s EUA was expanded to asymptomatic COVID-19 testing, as well as testing of pooled samples. A month later, the Aptima SARS-CoV-2 assay followed suit. The company was also awarded a $119 million U.S. government contract in October 2020 to support provision of 13 million COVID-19 tests per month in the U.S. market by January 2022.
“In the beginning of the pandemic, Hologic was able to quickly shift production capacity from other diagnostic tests as we worked to develop, then scale up manufacturing to meet the unprecedented demand for COVID-19 tests,” Kevin Thornal, Hologic’s division president of Diagnostic Solutions, told MPO. “Before the pandemic, we were producing approximately 20 million tests per quarter; that number more than doubled by the end of 2021 due to investments in new construction and expansion of production lines. This increase in capacity represents what would normally have taken place over a time period of 10 years. Both the production expansion and test development were supported in part by grants from the Department of Defense, in coordination with the Department of Health and Human Services (HHS) and the Biomedical Advanced Research and Development Authority within HHS.”
In October 2021, Hologic released the Aptima SARS-CoV-2/Flu assay in North America and Europe due to FDA EUA, a CE mark, and Health Canada Interim Order. It can simultaneously spot SARS-CoV-2, influenza A, and influenza B, which all present with similar symptoms.
The World Health Organization designated the latest significant COVID-19 variant of concern—B.1.1.529, also known as Omicron—on Nov. 26, 2021. Because it had about 30 genetic mutations, there was concern of the effect on diagnostic tests’ accuracy. Thankfully, widely used PCR tests continued to spot the infection.
“Due to the natural biology of viruses, which continually mutate and generate new variants, Hologic designed its assays with potential emergent variants in mind,” said Thornal. “To date, Hologic’s Aptima SARS-CoV-2 Assay, Aptima SARS-CoV-2/Flu Assay, and Panther Fusion SARS-CoV-2 Assay can identify all strains of COVID-19. When Omicron first emerged, to ensure accuracy, we tested more than 175 omicron-infected samples, obtained through GISAID (Global Initiative On Sharing All Influenza Data). We found none of the new mutations occur within regions of the genome targeted by our assays. We will continue to test the efficacy of our tests against any new emerging variants.”
This past January, Hologic added the Aptima SARS-CoV-2 assay to its Global Access Inititative, a program aiming to expand access to diagnostic testing in countries with limited resources. The assay is also provided by the WHO Diagnostics Consortium for countries with limited market access. The firm also partners with UNICEF, the Global Fund to Fight AIDS, Tuberculosis, and Malaria, and the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) to help countries in need obtain COVID-19 tests.
Teammates in Testing
An IVD device and component manufacturing partnership can be a valid strategic choice because of the significant capital needed for in-house manufacturing. In addition to equipment costs, there’s the need to build a quality management system aligned with regulatory requirements, personnel hiring, and acquiring the appropriate certifications. Many companies choose outsourcing to redeploy capital toward growing their business and developing new products. It’s important that an IVD manufacturing partner be able to master supply chain management, assay scale-up to manufacture, and regulatory compliance.
According to a February Research and Market report, the global IVD contract manufacturing services market is expected to grow 7.7 percent per year from 2021-2028 to reach $20.6 billion by 2028. The driver for this need is primarily due to the rising prevalence of infectious diseases like COVID-19, the shift from centralized laboratories to point-of-care testing, regulatory complexities, and cost-effective IVD test manufacturing.
This market includes not just complete IVD devices but their various components—sample collection, fluid management, diagnostic cartridges, convenience kits, and many others. It also covers ancillary services for IVD device and component design and manufacturing. To look more closely into this market, MPO spoke to several IVD manufacturing partners over the last few weeks:
Krista Ewing, Ph.D., diagnostics product manager at Porex Filtration Group, a Fairburn, Ga.-based developer of custom-engineered porous polymer solutions.
Ravi Narayanan, global product manager at Nordson Medical, a Minneapolis, Minn.-based manufacturer of medical balloons, medical tubing, catheters and cannulae, fluid management components, and nitinol components.
Bill Ruth, director of global sales, Diagnostics, at Roechling Medical, a Rochester, N.Y.-based supplier of high-quality plastic components, primary packaging, and system solutions for pharma, diagnostics, surgery, and medical technology.
Eileen Williams, senior vice president of Silgan Unicep, a Stamford, Conn.-based supplier of sustainable rigid packaging as well as precision dosing dispensing packaging solutions.
John Woodhouse, director of sales and marketing at Medbio, a Grand Rapids, Mich.-based full-service medical contract manufacturer.
Sam Brusco: Which in-vitro diagnostic (IVD) devices, components, or services does your company offer, and what purpose do they serve in IVD devices?
Krista Ewing, Ph.D.: Porex offers a variety of sample collection components focused mainly on absorption, wicking, and filtration of various of sample types including saliva, nasal, blood, and stool. In terms of absorption and wicking, one of our main product functions is as a sample pad, such as a urine wick on a pregnancy test, along with our other conjugate and waste pad components for lateral flow assays. When it comes to filtration, these offerings can be a pre-filter upstream of the IVD test, like our SQeasy product where the sample is filtered by squeezing the sample through a filter (similar to a dropper bottle) or the filter can be a custom component built into the sample intake of a cartridge-based IVD device. In addition to sample collection, many IVD devices require venting to prevent biological samples from exiting the device, where we offer porous PTFE membranes that work very well in many types of IVD devices, including microfluidic cartridges.
Ravi Narayanan: Nordson Medical manufactures hundreds of fluid management components used in IVD devices. These components could be Luers for fluid connections, tube-to-tube fittings used in flow control, manifolds for branching fluids in multiple directions, and/or quick connects to facilitate faster connections and disconnections. Having served IVD customers for over 50 years, we enjoy the breadth and depth in our portfolio offering components in various plastic materials, helping IVD applications adopt caustic reagents and solutions.
Bill Ruth: Roechling provides finished convenience kits for IVD applications. These tests identify many different diseases all with one swab of saliva, urine, or other bodily fluids.
Eileen Williams: Silgan Unicep manufactures blow-fill-seal units used to deliver liquids in diagnostic test workflows. We also offer turnkey services, including mixing the solution as well as molding and filling the primary package. Our unit-dose designs can provide a specified volume of liquid in a simple and easy-to-use format. Our designs are particularly well-suited for point-of-care and at-home tests.
John Woodhouse: Medbio manufactures a range of injection-molded components used for IVD devices, many in high volumes. A large portion of our business is in the IVD space, ranging from simple shoot-and-ship vials, to almost fully assembled multi-component cartridges that will hold reagents and patient samples, to microfluidic plates used in sampling kits. Some of the larger OEMs use these devices to test for COVID and other respiratory ailments, as well as an increasing array of diseases, sensitivities, or conditions that can be ascertained with genomic detection.
Brusco: How do you ensure the highest quality devices, components, and services for IVD customers?
Dr. Ewing: Our product development teams work diligently with both our customers and manufacturing teams to ensure all products are designed in a scalable manner. We have established a quality management system to manage design, development, and manufacturing of sintered porous plastics and fiber products. In addition, all our facilities have been certified to International Standards Organization (ISO) standards.
Narayanan: Over the years, we have learned and met the needs of the OEM and end-users of the IVD industry. We make most of our products in a 14644 Class 8 clean room. We have strict quality standards for our components including flash control, gate vestige, particulate standards, etc. We also don’t use re-grind materials in end products. Our injection molding machines are electric, relieving worry about oil spillage. Our facility and quality standards are collaboratively audited by customers in the entire value chain, which allows us to learn their needs and incorporate best practices in our business processes.
Ruth: We have very stringent quality guidelines and cleanliness requirements in our cleanrooms. We feel educating our employees on the end-use of the products helps to ensure their commitment to quality throughout the manufacturing process.
Williams: Our facilities are FDA-registered and ISO-13485 certified. We have a robust quality system to ensure we manufacture our products to the highest applicable regulatory standards. Our program managers work closely with customers to understand unique product requirements critical to test efficacy. Program managers then align Silgan Unicep’s quality, regulatory, and engineering resources to ensure those requirements are contemplated in process development and met in a consistent and compliant fashion during commercial production.
Woodhouse: Since many of our customers’ assays would be compromised with human RNA/DNA contamination, we must ensure quality and cleanliness with as little human interaction as possible. Robots remove many parts from the molds. These are also packaged robotically and never touched by our employees. Measurement samples are set aside automatically, at specific intervals, and discarded after assessment. Multi-cavity tooling is built with cavity separation to allow the greatest flexibility during production, in the event one or more cavities start trending out of tolerance or incur damage. We have added cameras for inline inspection to some of our automated molding cells and many poka-yokes and sensors to high-volume laser-welding cells for consistent operation. High-volume assembly equipment is strictly validated to ensure a good part emerges about every two seconds. We continue to upgrade our CMM (coordinate measurement machine) equipment for rapid and accurate inspection of these tight-tolerance, multi-cavity parts so we can confidently ship the millions of parts per month demanded of our operation.
But COVID-19 hasn’t just increased the scale and demand for disease testing for pretty much everyone; it’s also spurred adopting more advanced versions of the tests. Hospital systems have begun to purchase PCR (polymerase chain reaction) machines small enough to install in a clinic so samples don’t have to be shipped to a big, centralized lab. This meant patients could get a diagnosis on the spot and isolate immediately afterward. Companies and university researchers working on PCR technologies have reported there’s growing demand for their innovations, like handheld versions that would make testing pretty much anywhere more feasible.
The benefits of this research may extend beyond individual patients. The quick-spreading Omicron variant that emerged in late 2021 showed that testing at the population level was integral to track how COVID-19 might transform and push healthcare systems to a breaking point. The proliferation of PCR testing for COVID-19 could stimulate stronger public health surveillance that can identify future pandemics by testing for dozens of pathogens at one time.
At the time of writing, the U.S. Food and Drug Administration (FDA) has authorized under its emergency use authorization (EUA) over 400 COVID-19 tests and collection kits, comprised of 235 molecular (PCR) tests, 88 antibody tests, and 34 antigen (rapid) tests. Sixty-three of the tests are authorized for home collection, 32 for sample pooling, 55 at the point of care, 19 multi-analyte tests, (COVID-19 and other viruses like the flu), and 13 at-home tests.
PCR testing is considered the gold standard for SARS-CoV-2 detection. The tests detects RNA (or genetic material) specific to the virus via a nasal swab sample and can spot it within days of infection. Turnaround time is generally two to three days but results can arrive in as little as 24 hours. The PCR test is considered the most accurate and reliable test for COVID-19.
Further, once scientists identify new COVID variants they can use PCR testing to track those variants’ spread. Antigen-based methods can’t do this. The Omicron variant’s emergence showed how crucial it was to track variants—data streaming in from PCR tests indicated Omicron was spreading much more quickly compared to its Delta variant predecessor. Because of this data, some governments updated pandemic guidelines and encouraged more booster shots. Some people took the data as a cue to reconsider social interactions and ugrpade their masks’ efficacy as well.
Antigen testing detects protein fragments (antigens) specific to the SARS-CoV-2 virus. It can be done in a clinic, doctor’s office, hospital, or even at home. The turnaround time for antigen test results is usually very quick—because results can be reported in as little as 15 minutes, these tests are also referred to as rapid tests.
In order to boost access to testing, on Jan. 14 the U.S. government purchased 1 billion at-home, rapid COVID-19 tests to give to Americans for free. The tests became available on Jan. 19 and could be mailed directly to U.S. households, with a maximum of four tests per household. The Administration also announced beginning Jan. 15 that private health insurance companies were mandated to cover at-home COVID-19 tests for free and made an additional 10 million tests available to schools nationwide each month.
Medical device and diagnostics firm Abbott Laboratories was and continues to be a significant provider of SARS-CoV-2 diagnostic tests. The firm’s RealTime SARS-CoV-2 molecular test earned FDA emergency use authorization on March 18, 2020. Ten days later the company gained EUA for the ID NOW COVID-19 test, which generates a diagnosis in 13 minutes. In June, EUA was granted for Abbott’s Alinity m molecular lab instrument to test for COVID-19.
An IgG serology test was launched in April 2020, gained EUA a month later, then acquired a CE mark in December 2020. The AdviseDx SARS-CoV-2 IgM antibody test joined the list in October 2020.
The momentous EUA for the BinaxNow COVID-19 Ag Card—a credit card-sized, five-dollar, 15-minute COVID-19 lateral flow antigen test—came in August 2020. In December 2020, EUA for the test was expanded to virtually-guided home use. Abbott fulfilled the federal government’s order of 150 million tests in January 2021. The test was further expanded to over-the-counter, non-prescription, asymptomatic use in March 2021.
Everyone aged 15 and older are authorized to self-collect samples. Adults can collect samples for children as young as 2. The BinaxNow COVID-19 Ag self-test began shipment to retailers on April 19, 2021.
January 2021 saw a CE mark for the Panbio COVID-19 Ag Rapid test for asymptomatic testing and self-swabbing, supporting mass testing in congregate, asymptomatic populations. A self-test for sale directly to consumers secured CE marking last June.
Abbott CEO Robert Ford joined the White House task force in April 2020 to guide the safe reopening of the U.S. economy. And in March 2021, the company formed the Abbott Pandemic Defense coalition, a global scientific and public health partnership to detect and respond to future pandemic threats. The program aims to connect lab experts, genetic sequencing experts, and public health research experts to identify new pathogens, analyze potential risks, rapidly develop and deploy new diagnostic tests, and assess the impact on public health. That same month the company nabbed EUA for the Alinity m Resp-4-Plex molecular assay, which identifies SARS-CoV-2, influenza A, influenza B, and respiratory syncytial virus in one test.
“We’ve been working 24/7 to scale our operations, producing 70 million tests in January and further scaling toward 100 million a month in March,” an Abbott spokesperson told MPO. “We self-invested to build two new U.S. manufacturing facilities in Maine and Illinois that today employ more than 5,000 people.”
To respond to the variant of concern Omicron, Abbott conducted lab analyses and tests from a live virus, including from the first U.S. Omicron case. BinaxNOW spotted the virus in all tests performed, according to the company, at equal sensitivity as other variants. Data from Abbott customer use did not show a change in test performance, the company reported.
Diagnostics and imaging firm Hologic was also among the first to develop and distribute molecular assays for COVID-19. The company’s Panther Fusion system, which can process up to 1,000 tests in 24 hours, gained FDA emergency use authorization for the Panther Fusion SARS-CoV-2 assay on March 16, 2020. The Biomedical Advanced Research and Development Authority (BARDA) contributed financing to accelerate development of the assay. On May 15, 2020, the firm’s Aptima SARS-CoV-2 assay gained an EUA for the Panther system. In July 2021, the assay secured CE mark was achieved for use of saliva samples.
In September 2020, the Panther Fusion SARS-CoV-2 assay’s EUA was expanded to asymptomatic COVID-19 testing, as well as testing of pooled samples. A month later, the Aptima SARS-CoV-2 assay followed suit. The company was also awarded a $119 million U.S. government contract in October 2020 to support provision of 13 million COVID-19 tests per month in the U.S. market by January 2022.
“In the beginning of the pandemic, Hologic was able to quickly shift production capacity from other diagnostic tests as we worked to develop, then scale up manufacturing to meet the unprecedented demand for COVID-19 tests,” Kevin Thornal, Hologic’s division president of Diagnostic Solutions, told MPO. “Before the pandemic, we were producing approximately 20 million tests per quarter; that number more than doubled by the end of 2021 due to investments in new construction and expansion of production lines. This increase in capacity represents what would normally have taken place over a time period of 10 years. Both the production expansion and test development were supported in part by grants from the Department of Defense, in coordination with the Department of Health and Human Services (HHS) and the Biomedical Advanced Research and Development Authority within HHS.”
In October 2021, Hologic released the Aptima SARS-CoV-2/Flu assay in North America and Europe due to FDA EUA, a CE mark, and Health Canada Interim Order. It can simultaneously spot SARS-CoV-2, influenza A, and influenza B, which all present with similar symptoms.
The World Health Organization designated the latest significant COVID-19 variant of concern—B.1.1.529, also known as Omicron—on Nov. 26, 2021. Because it had about 30 genetic mutations, there was concern of the effect on diagnostic tests’ accuracy. Thankfully, widely used PCR tests continued to spot the infection.
“Due to the natural biology of viruses, which continually mutate and generate new variants, Hologic designed its assays with potential emergent variants in mind,” said Thornal. “To date, Hologic’s Aptima SARS-CoV-2 Assay, Aptima SARS-CoV-2/Flu Assay, and Panther Fusion SARS-CoV-2 Assay can identify all strains of COVID-19. When Omicron first emerged, to ensure accuracy, we tested more than 175 omicron-infected samples, obtained through GISAID (Global Initiative On Sharing All Influenza Data). We found none of the new mutations occur within regions of the genome targeted by our assays. We will continue to test the efficacy of our tests against any new emerging variants.”
This past January, Hologic added the Aptima SARS-CoV-2 assay to its Global Access Inititative, a program aiming to expand access to diagnostic testing in countries with limited resources. The assay is also provided by the WHO Diagnostics Consortium for countries with limited market access. The firm also partners with UNICEF, the Global Fund to Fight AIDS, Tuberculosis, and Malaria, and the U.S. President’s Emergency Plan for AIDS Relief (PEPFAR) to help countries in need obtain COVID-19 tests.
Teammates in Testing
An IVD device and component manufacturing partnership can be a valid strategic choice because of the significant capital needed for in-house manufacturing. In addition to equipment costs, there’s the need to build a quality management system aligned with regulatory requirements, personnel hiring, and acquiring the appropriate certifications. Many companies choose outsourcing to redeploy capital toward growing their business and developing new products. It’s important that an IVD manufacturing partner be able to master supply chain management, assay scale-up to manufacture, and regulatory compliance.
According to a February Research and Market report, the global IVD contract manufacturing services market is expected to grow 7.7 percent per year from 2021-2028 to reach $20.6 billion by 2028. The driver for this need is primarily due to the rising prevalence of infectious diseases like COVID-19, the shift from centralized laboratories to point-of-care testing, regulatory complexities, and cost-effective IVD test manufacturing.
This market includes not just complete IVD devices but their various components—sample collection, fluid management, diagnostic cartridges, convenience kits, and many others. It also covers ancillary services for IVD device and component design and manufacturing. To look more closely into this market, MPO spoke to several IVD manufacturing partners over the last few weeks:
Krista Ewing, Ph.D., diagnostics product manager at Porex Filtration Group, a Fairburn, Ga.-based developer of custom-engineered porous polymer solutions.
Ravi Narayanan, global product manager at Nordson Medical, a Minneapolis, Minn.-based manufacturer of medical balloons, medical tubing, catheters and cannulae, fluid management components, and nitinol components.
Bill Ruth, director of global sales, Diagnostics, at Roechling Medical, a Rochester, N.Y.-based supplier of high-quality plastic components, primary packaging, and system solutions for pharma, diagnostics, surgery, and medical technology.
Eileen Williams, senior vice president of Silgan Unicep, a Stamford, Conn.-based supplier of sustainable rigid packaging as well as precision dosing dispensing packaging solutions.
John Woodhouse, director of sales and marketing at Medbio, a Grand Rapids, Mich.-based full-service medical contract manufacturer.
Sam Brusco: Which in-vitro diagnostic (IVD) devices, components, or services does your company offer, and what purpose do they serve in IVD devices?
Krista Ewing, Ph.D.: Porex offers a variety of sample collection components focused mainly on absorption, wicking, and filtration of various of sample types including saliva, nasal, blood, and stool. In terms of absorption and wicking, one of our main product functions is as a sample pad, such as a urine wick on a pregnancy test, along with our other conjugate and waste pad components for lateral flow assays. When it comes to filtration, these offerings can be a pre-filter upstream of the IVD test, like our SQeasy product where the sample is filtered by squeezing the sample through a filter (similar to a dropper bottle) or the filter can be a custom component built into the sample intake of a cartridge-based IVD device. In addition to sample collection, many IVD devices require venting to prevent biological samples from exiting the device, where we offer porous PTFE membranes that work very well in many types of IVD devices, including microfluidic cartridges.
Ravi Narayanan: Nordson Medical manufactures hundreds of fluid management components used in IVD devices. These components could be Luers for fluid connections, tube-to-tube fittings used in flow control, manifolds for branching fluids in multiple directions, and/or quick connects to facilitate faster connections and disconnections. Having served IVD customers for over 50 years, we enjoy the breadth and depth in our portfolio offering components in various plastic materials, helping IVD applications adopt caustic reagents and solutions.
Bill Ruth: Roechling provides finished convenience kits for IVD applications. These tests identify many different diseases all with one swab of saliva, urine, or other bodily fluids.
Eileen Williams: Silgan Unicep manufactures blow-fill-seal units used to deliver liquids in diagnostic test workflows. We also offer turnkey services, including mixing the solution as well as molding and filling the primary package. Our unit-dose designs can provide a specified volume of liquid in a simple and easy-to-use format. Our designs are particularly well-suited for point-of-care and at-home tests.
John Woodhouse: Medbio manufactures a range of injection-molded components used for IVD devices, many in high volumes. A large portion of our business is in the IVD space, ranging from simple shoot-and-ship vials, to almost fully assembled multi-component cartridges that will hold reagents and patient samples, to microfluidic plates used in sampling kits. Some of the larger OEMs use these devices to test for COVID and other respiratory ailments, as well as an increasing array of diseases, sensitivities, or conditions that can be ascertained with genomic detection.
Brusco: How do you ensure the highest quality devices, components, and services for IVD customers?
Dr. Ewing: Our product development teams work diligently with both our customers and manufacturing teams to ensure all products are designed in a scalable manner. We have established a quality management system to manage design, development, and manufacturing of sintered porous plastics and fiber products. In addition, all our facilities have been certified to International Standards Organization (ISO) standards.
Narayanan: Over the years, we have learned and met the needs of the OEM and end-users of the IVD industry. We make most of our products in a 14644 Class 8 clean room. We have strict quality standards for our components including flash control, gate vestige, particulate standards, etc. We also don’t use re-grind materials in end products. Our injection molding machines are electric, relieving worry about oil spillage. Our facility and quality standards are collaboratively audited by customers in the entire value chain, which allows us to learn their needs and incorporate best practices in our business processes.
Ruth: We have very stringent quality guidelines and cleanliness requirements in our cleanrooms. We feel educating our employees on the end-use of the products helps to ensure their commitment to quality throughout the manufacturing process.
Williams: Our facilities are FDA-registered and ISO-13485 certified. We have a robust quality system to ensure we manufacture our products to the highest applicable regulatory standards. Our program managers work closely with customers to understand unique product requirements critical to test efficacy. Program managers then align Silgan Unicep’s quality, regulatory, and engineering resources to ensure those requirements are contemplated in process development and met in a consistent and compliant fashion during commercial production.
Woodhouse: Since many of our customers’ assays would be compromised with human RNA/DNA contamination, we must ensure quality and cleanliness with as little human interaction as possible. Robots remove many parts from the molds. These are also packaged robotically and never touched by our employees. Measurement samples are set aside automatically, at specific intervals, and discarded after assessment. Multi-cavity tooling is built with cavity separation to allow the greatest flexibility during production, in the event one or more cavities start trending out of tolerance or incur damage. We have added cameras for inline inspection to some of our automated molding cells and many poka-yokes and sensors to high-volume laser-welding cells for consistent operation. High-volume assembly equipment is strictly validated to ensure a good part emerges about every two seconds. We continue to upgrade our CMM (coordinate measurement machine) equipment for rapid and accurate inspection of these tight-tolerance, multi-cavity parts so we can confidently ship the millions of parts per month demanded of our operation.