Maria Shepherd, President and Founder, Medi-Vantage01.29.20
Digital health represents a holy grail within the medical device industry: a solution that improves patient outcomes at a lower cost. It presents an enormous growth opportunity for many companies. In addition, digital health will be further advanced through a convergence of enabling technologies—5G, artificial intelligence, machine learning, and wearables—all of which are becoming commonplace (or at least soon will be) among patients within their homes.
5G healthcare technology will be enabled by broadband speeds of greater than one gigabit per second. With a lower cost of installing broadband and a growing 5G footprint, costs will be further reduced.
Why This Is Important
The average patient cost of care within the home as compared to within the hospital was 38 percent less, according to a study in the Annals of Internal Medicine (n=91) that compared outcomes and costs of hospital-level care provided in the home. Compared with traditional care patients, home patients had fewer laboratory orders (median per admission, 3 vs. 15), imaging studies (median, 14 percent vs. 44 percent), and consultations (median, 2 percent vs. 31 percent) (Table 1).1
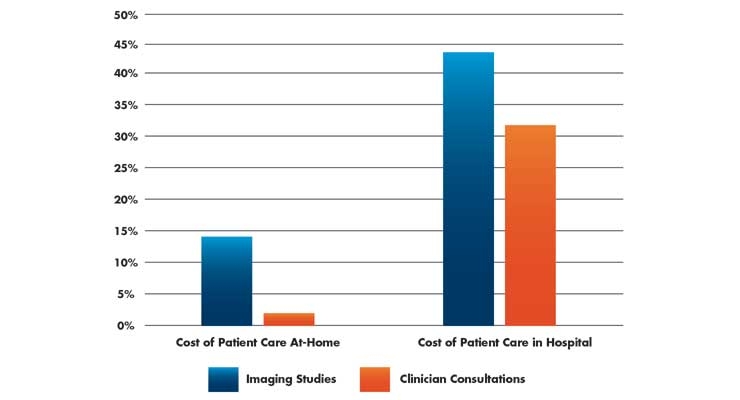
Table 1: The cost of patient care at home vs. in hospital1
The data also paints a positive picture regarding 30-day readmissions. Readmission rates to the hospital were lower among the at-home patients compared to those receiving traditional care (i.e., in hospital; 7 percent vs. 23 percent) (Table 2). Further, it was reported the at-home patients spent a smaller proportion of the day sedentary (median, 12 percent vs. 23 percent) or lying down (median, 18 percent vs. 55 percent).1
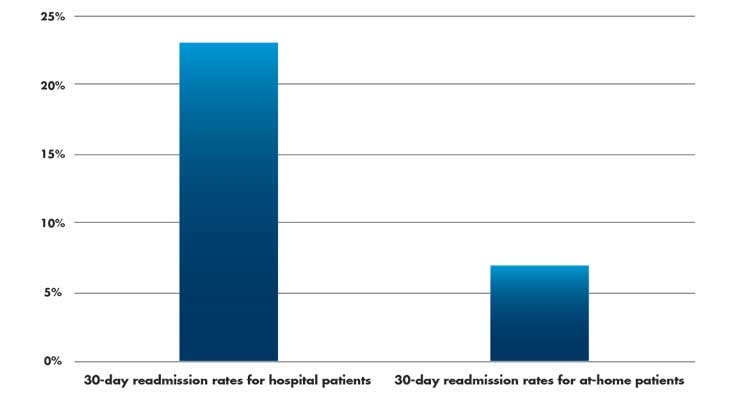
Table 2: 30-day readmission rates for patients at-home vs. in-hospital1
U.S. health systems want to find ways to reduce costs; however, the shift to treating patients at home instead of admitting them to a hospital is new. Traditionally, Medi-Vantage’s strategy research has yielded data showing administrators were most concerned with ensuring beds were occupied. Now, we are seeing another trend emerge—new business models that lower costs. There are currently several joint ventures underway to evaluate the costs and reimbursements associated with bringing hospital care to at-home patients.
Another driver of home healthcare is the aging of baby boomers. If hospital costs are higher, as shown in the Annals of Internal Medicine study, and hospital administrators are compelled to reduce the costs of care while improving quality and outcomes, caring for patients at home is sensible to investigate. Further, CMS is getting on board with new policies that facilitate home healthcare and remote patient monitoring. For many years, Medicare hesitated to reimburse doctors for remote patient monitoring. All that has changed since CMS launched remote monitoring reimbursement codes for chronic care.
Home Healthcare for Patients Is the Newest Channel
There is great opportunity in home healthcare for the medical device industry. For example, in 2019, LHC Group set a goal to shift more care to the home. The home healthcare leader has announced a new joint venture in Arkansas with Unity Health. The Lafayette, La.-based company has a broad partnership and joint-venture strategy, and should execute more deals like this in the future.
Home healthcare management is becoming simpler for hospitals. Costs are reduced through remote monitoring, which shares patient data with hospitals, clinics, and/or doctors. Physicians can assess the data, taking appropriate steps to return the patient to the hospital, clinic, or doctor’s office, if necessary, to ensure the patient is getting care in the right place at the right time.
Machine Learning and AI Will Broaden the Boundaries of Home Healthcare
It is a perfect storm. The surge in digital health technology will drive data from multiple sources to create future innovations in medical device connectivity. Cost pressures push hospitals to identify new care management strategies as chronic conditions continue to grow. Prices will drop as the use of digital technology drives increased unit production volumes.
This will allow the development of medical devices to gather data to recognize trends, calculate outcomes, and help to inform clinical response. Connectivity is a critical part of the equation when it comes to future medical device innovation. It can lead to true improvements in patient care and better health outcomes. It can minimize the issue of patient compliance, by making the care of the patient so seamless the monitoring of their health and the delivery of care become far less intrusive.
When patient care does involve a level of intervention, providers can make it easier for patients to engage in new, healthy habits. Behavioral economics plays a significant role here. The Nudge Theory is a Nobel Prize-winning behavioral economics model that is a proponent of indirect suggestions, gentle reminders, and positive reinforcement to influence the actions of any population.2 Applying this theory to the challenging issue of improving patient compliance with a care plan can, when applied correctly, improve that patient’s outcomes. The automated system uses push notifications to patients to encourage them to enter biometric, objective, or subjective data. This allows patients to respond at a time and place convenient for them.
The act of being “nudged” to capture and report outcomes in a consistent, seamless, and unobtrusive way can drive positive health actions at a level providers have never seen before. Patient training time will be reduced because smartphones are already in broad use and technology can imitate the push notifications already being sent to the general population on a regular basis.
CMS and Reimbursement
There are four new codes CMS is reimbursing in 2019 (Table 3).3
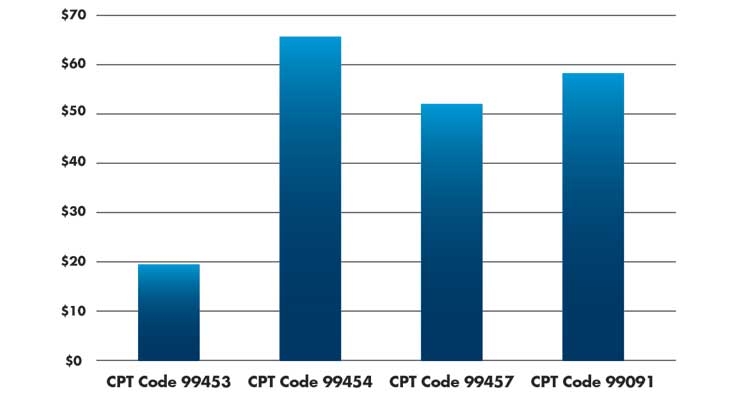
Table 3: The median national CMS payment for remote monitoring services3-5
CPT code 99453—Remote monitoring: physiologic parameters, initial; set-up, and patient education on use of equipment. Offers reimbursement for the work of onboarding new patients onto a remote patient monitoring service, setup of the equipment, and patient education.
CPT code 99454—Devices with daily recordings or programmed alerts transmission, each 30 days. Offers reimbursement for providing the patient with a remote patient monitoring device for 30 days. Can be billed every 30 days.
CPT code 99457—Remote physiologic monitoring treatment, >20 minutes of qualified healthcare professional time in one calendar month requiring interactive communication with the patient or caregiver during the month. Offers reimbursement for clinical staff time used for monitoring and communications by phone, text, and email. Reimbursement is $51.54 for non-facility and $32.44 for facility payments.
CPT code 99091—Compilation and interpretation of digitally stored or physiologic data transmitted by the patient or caregiver to a qualified healthcare professional, requiring a minimum of 30 minutes of time, each 30 days. Offers reimbursement for monitoring services without communications like 99457. Requires a physician or other qualified healthcare professional to provide service, must include 30 minutes of time every 30 days to bill. 99457 and 99091 cannot be billed in parallel.
The Medi-Vantage Perspective
There are many other rules and regulations to be followed while billing for these codes. The point is CMS is boldly moving into new territory that can be used in the development of medical devices with a digital health technology component. How can advances in communication technology change your device to make the patient and provider experience better?
References
Maria Shepherd has more than 20 years of experience in medical device marketing in small startups and top-tier companies. After her industry career, including her role as VP of marketing for Oridion Medical, where she boosted the company valuation prior to its acquisition, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing, business strategy, and innovation research for the medical device, diagnostic, and digital health industries. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.aligo.com). She can be reached at 855-343-3100. Visit her website at www.medi-vantage.com.
5G healthcare technology will be enabled by broadband speeds of greater than one gigabit per second. With a lower cost of installing broadband and a growing 5G footprint, costs will be further reduced.
Why This Is Important
The average patient cost of care within the home as compared to within the hospital was 38 percent less, according to a study in the Annals of Internal Medicine (n=91) that compared outcomes and costs of hospital-level care provided in the home. Compared with traditional care patients, home patients had fewer laboratory orders (median per admission, 3 vs. 15), imaging studies (median, 14 percent vs. 44 percent), and consultations (median, 2 percent vs. 31 percent) (Table 1).1

Table 1: The cost of patient care at home vs. in hospital1
The data also paints a positive picture regarding 30-day readmissions. Readmission rates to the hospital were lower among the at-home patients compared to those receiving traditional care (i.e., in hospital; 7 percent vs. 23 percent) (Table 2). Further, it was reported the at-home patients spent a smaller proportion of the day sedentary (median, 12 percent vs. 23 percent) or lying down (median, 18 percent vs. 55 percent).1

Table 2: 30-day readmission rates for patients at-home vs. in-hospital1
U.S. health systems want to find ways to reduce costs; however, the shift to treating patients at home instead of admitting them to a hospital is new. Traditionally, Medi-Vantage’s strategy research has yielded data showing administrators were most concerned with ensuring beds were occupied. Now, we are seeing another trend emerge—new business models that lower costs. There are currently several joint ventures underway to evaluate the costs and reimbursements associated with bringing hospital care to at-home patients.
Another driver of home healthcare is the aging of baby boomers. If hospital costs are higher, as shown in the Annals of Internal Medicine study, and hospital administrators are compelled to reduce the costs of care while improving quality and outcomes, caring for patients at home is sensible to investigate. Further, CMS is getting on board with new policies that facilitate home healthcare and remote patient monitoring. For many years, Medicare hesitated to reimburse doctors for remote patient monitoring. All that has changed since CMS launched remote monitoring reimbursement codes for chronic care.
Home Healthcare for Patients Is the Newest Channel
There is great opportunity in home healthcare for the medical device industry. For example, in 2019, LHC Group set a goal to shift more care to the home. The home healthcare leader has announced a new joint venture in Arkansas with Unity Health. The Lafayette, La.-based company has a broad partnership and joint-venture strategy, and should execute more deals like this in the future.
Home healthcare management is becoming simpler for hospitals. Costs are reduced through remote monitoring, which shares patient data with hospitals, clinics, and/or doctors. Physicians can assess the data, taking appropriate steps to return the patient to the hospital, clinic, or doctor’s office, if necessary, to ensure the patient is getting care in the right place at the right time.
Machine Learning and AI Will Broaden the Boundaries of Home Healthcare
It is a perfect storm. The surge in digital health technology will drive data from multiple sources to create future innovations in medical device connectivity. Cost pressures push hospitals to identify new care management strategies as chronic conditions continue to grow. Prices will drop as the use of digital technology drives increased unit production volumes.
This will allow the development of medical devices to gather data to recognize trends, calculate outcomes, and help to inform clinical response. Connectivity is a critical part of the equation when it comes to future medical device innovation. It can lead to true improvements in patient care and better health outcomes. It can minimize the issue of patient compliance, by making the care of the patient so seamless the monitoring of their health and the delivery of care become far less intrusive.
When patient care does involve a level of intervention, providers can make it easier for patients to engage in new, healthy habits. Behavioral economics plays a significant role here. The Nudge Theory is a Nobel Prize-winning behavioral economics model that is a proponent of indirect suggestions, gentle reminders, and positive reinforcement to influence the actions of any population.2 Applying this theory to the challenging issue of improving patient compliance with a care plan can, when applied correctly, improve that patient’s outcomes. The automated system uses push notifications to patients to encourage them to enter biometric, objective, or subjective data. This allows patients to respond at a time and place convenient for them.
The act of being “nudged” to capture and report outcomes in a consistent, seamless, and unobtrusive way can drive positive health actions at a level providers have never seen before. Patient training time will be reduced because smartphones are already in broad use and technology can imitate the push notifications already being sent to the general population on a regular basis.
CMS and Reimbursement
There are four new codes CMS is reimbursing in 2019 (Table 3).3

Table 3: The median national CMS payment for remote monitoring services3-5
CPT code 99453—Remote monitoring: physiologic parameters, initial; set-up, and patient education on use of equipment. Offers reimbursement for the work of onboarding new patients onto a remote patient monitoring service, setup of the equipment, and patient education.
CPT code 99454—Devices with daily recordings or programmed alerts transmission, each 30 days. Offers reimbursement for providing the patient with a remote patient monitoring device for 30 days. Can be billed every 30 days.
CPT code 99457—Remote physiologic monitoring treatment, >20 minutes of qualified healthcare professional time in one calendar month requiring interactive communication with the patient or caregiver during the month. Offers reimbursement for clinical staff time used for monitoring and communications by phone, text, and email. Reimbursement is $51.54 for non-facility and $32.44 for facility payments.
CPT code 99091—Compilation and interpretation of digitally stored or physiologic data transmitted by the patient or caregiver to a qualified healthcare professional, requiring a minimum of 30 minutes of time, each 30 days. Offers reimbursement for monitoring services without communications like 99457. Requires a physician or other qualified healthcare professional to provide service, must include 30 minutes of time every 30 days to bill. 99457 and 99091 cannot be billed in parallel.
The Medi-Vantage Perspective
There are many other rules and regulations to be followed while billing for these codes. The point is CMS is boldly moving into new territory that can be used in the development of medical devices with a digital health technology component. How can advances in communication technology change your device to make the patient and provider experience better?
References
Maria Shepherd has more than 20 years of experience in medical device marketing in small startups and top-tier companies. After her industry career, including her role as VP of marketing for Oridion Medical, where she boosted the company valuation prior to its acquisition, director of marketing for Philips Medical, and senior management roles at Boston Scientific Corp., she founded Medi-Vantage. Medi-Vantage provides marketing, business strategy, and innovation research for the medical device, diagnostic, and digital health industries. The firm quantitatively and qualitatively sizes and segments opportunities, evaluates new technologies, provides marketing services, and assesses prospective acquisitions. Shepherd has taught marketing and product development courses and is a member of the Aligo Medtech Investment Committee (www.aligo.com). She can be reached at 855-343-3100. Visit her website at www.medi-vantage.com.













