Business Wire01.16.20
Masimo announced that in a study recently published in the Journal of Clinical Monitoring and Computing, researchers at Nippon Medical School in Tokyo used Masimo Patient SafetyNet and rainbow Acoustic Monitoring (RAM), acoustic respiration rate monitoring with RRa, as a centralized continuous monitoring system to identify the incidence and predictors of desaturation and bradypnea in postoperative patients—concluding that “Use of monitoring systems might provide a safety net for postoperative patients.”1
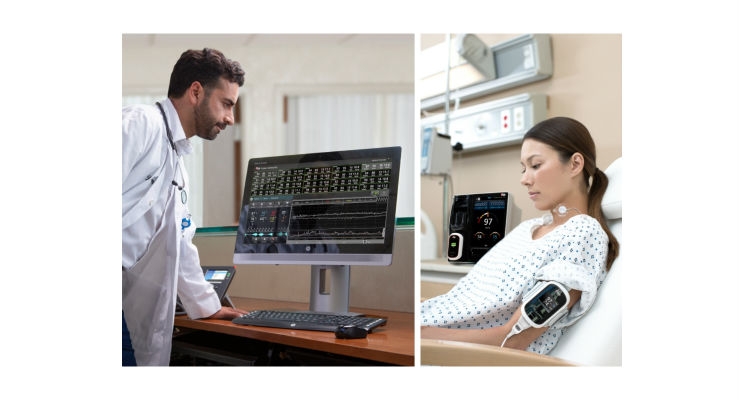
Patient SafetyNet is a supplemental remote monitoring, patient surveillance, and clinician notification system that works in conjunction with Masimo and third-party bedside monitoring devices to display near real-time data at central stations. RAM with RRa uses an acoustic transducer positioned on the patient’s neck to provide noninvasive, continuous respiration monitoring.
Hypothesizing that postoperative desaturation and bradypnea might occur even in non-ICU patients without serious complications, and in patients who did not undergo major surgery, Drs. Masashi Ishikawa and Atsuhiro Sakamoto set up a centralized postoperative monitoring system in the general ward to investigate how common these events are for such patients (and what might predict them). They analyzed demographic and monitoring data from 1,064 adult patients who underwent general anesthesia for various surgical procedures over a four-month period. The patients were monitored using a pulse oximeter and an RRa sensor for at least 8 hours after surgery, data which were automatically transferred to Patient SafetyNet.
From the data stored on the Patient SafetyNet, the researchers were able to retrospectively analyze the incidence of desaturation (defined as SpO2 < 90 percent for > 10 seconds) and bradypnea (defined as respiratory rate < eight breaths/minute for > two minutes). They found that 12.1 percent of patients exhibited desaturation (244 events among 129 patients), with most occurring after the termination of oxygen administration, and 50.8 percent of the events occurring more than eight hours after surgery. They found that 5.1 percent of the patients exhibited bradypnea (112 times among 54 patients), with 72.3 percent of the events occurring during oxygen supplementation, and with the greatest incidence within the first hour after surgery. Age, body mass index, and current smoking status were significant risk factors for desaturation. Sleep apnea syndrome and postoperative opioid administration were significant risk factors for bradypnea. Age and postoperative opioid administration were significant risk factors for the combination of desaturation and bradypnea.
The researchers concluded, “Our study suggests that use of a continuous and centralized respiratory monitoring system for overnight postoperatively is desirable for postoperative management in the general ward, which would likely improve the safety of postoperative patients, especially those with risk factors for respiratory depression.”
The researchers commented on a number of methods of respiratory rate monitoring, stating, “Continuous and centralized monitoring of oxygen saturation and respiratory rate can detect respiratory depression before it results in critical events such as cardiac arrest. Several methods of respiratory rate monitoring are currently used, including manual counting of breaths by a caregiver, capnography, and transthoracic impedance measurement. Manual counting of breaths (such as auscultation) is an intermittent, labor-intensive and unreliable method. Capnography provides accurate and continuous monitoring, but requires a nasal or facial interface, which can be uncomfortable and may lead to failure if the interface is moved. Transthoracic impedance is non-invasive and can detect respiratory efforts, but is unable to detect alveolar hypoventilation caused by airway obstruction.”2-6
Additionally, the researchers commented on RAM with RRa, the respiratory rate monitoring method used in the current study, and referenced another study in which RRa and capnography were compared, stating: “RRa is an acoustic monitoring device that continuously measures respiratory rate, and is as accurate as capnography in extubated patients.7 Patient activities, such as talking, coughing and crying, affect the results of both RRa and capnography. The measurement errors during these activities are, however, not clinically relevant because they require that the patients are awake and breathing. Further, the RRa sensor appears to be well-tolerated and no more subject to error than capnography.7 RRa was found to be a reliable device and had fewer complications in this study.”
Masimo develops and produces an array of monitoring technologies, including measurements, sensors, patient monitors, and automation and connectivity solutions. Its mission is to improve patient outcomes and reduce the cost of care. Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, introduced in 1995, has been shown in over 100 independent and objective studies to outperform other pulse oximetry technologies.8 Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,9 improve CCHD screening in newborns,10 and, when used for continuous monitoring with Masimo Patient SafetyNet in post-surgical wards, reduce rapid response team activations, ICU transfers, and costs.11-13 Masimo SET is estimated to be used on more than 100 million patients in hospitals and other healthcare settings around the world,14 and is the primary pulse oximetry at nine of the top 10 hospitals according to the 2019-20 U.S. News and World Report Best Hospitals Honor Roll.15 Masimo continues to refine SET and in 2018, announced that SpO2 accuracy on RD SET sensors during conditions of motion has been significantly improved, providing clinicians with even greater confidence that the SpO2 values they rely on accurately reflect a patient’s physiological status. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), RPVi (rainbow PVi), and Oxygen Reserve Index (ORi). In 2013, Masimo introduced the Root Patient Monitoring and Connectivity Platform, built from the ground up to be as flexible and expandable as possible to facilitate the addition of other Masimo and third-party monitoring technologies; key Masimo additions include Next Generation SedLine Brain Function Monitoring, O3 Regional Oximetry, and ISA Capnography with NomoLine sampling lines. Masimo’s family of continuous and spot-check monitoring Pulse CO-Oximeters includes devices designed for use in a variety of clinical and non-clinical scenarios, including tetherless, wearable technology, such as Radius-7 and Radius PPG, portable devices like Rad-67, fingertip pulse oximeters like MightySat Rx, and devices available for use both in the hospital and at home, such as Rad-97. Masimo hospital automation and connectivity solutions are centered around the Iris platform, and include Iris Gateway, Patient SafetyNet, Replica, Halo ION, UniView, and Doctella.
ORi and RPVi have not received U.S. Food and Drug Administration 510(k) clearance and are not available for sale in the United States.
References
1 Ishikawa M and Sakamoto A. Postoperative desaturation and bradypnea after general anesthesia in non-ICU patients: a retrospective evaluation. J Clin Monit Comput. 2 Mar 2019. https://doi.org/10.1007/s10877-019-00293-0.
2 Petterson MT, Begnoche VL, and Graybeal JM. The effect of motion on pulse oximetry and its clinical significance. Anesth Analg. 2007;105(6 Suppl):78–84.
3 Wilkinson JN, and Thanawala VU. Thoracic impedance monitoring of respiratory rate during sedation—is it safe? Anaesthesia. 2009;64(4):455–6.
4 Cohen KP, Ladd WM, Beams DM, Sheers WS, Radwin RG, Tompkins WJ, and Webster JG. Comparison of impedance and inductance ventilation sensors on adults during breathing, motion, and simulated airway obstruction. IEEE Trans Biomed Eng. 1997;44(7):555–66.
5 Drummond GB, Nimmo AF, and Elton RA. Thoracic impedance used for measuring chest wall movement in postoperative patients. Br J Anaesth. 1996;77(3):327–32.
6 Brouillette RT, Morrow AS, Weese-Mayer DE, and Hunt CE. Comparison of respiratory inductive plethysmography and thoracic impedance for apnea monitoring. J Pediatr. 1987;111(3):377–83.
7 Mimoz O, Benard T, Gaucher A, Frasca D, and Debaene B. Accuracy of respiratory rate monitoring using a non-invasive acoustic method after general anaesthesia. Br J Anaesth. 2012 May;108(5):872–5.
8 Published clinical studies on pulse oximetry and the benefits of Masimo SET® can be found on our website at http://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
9 Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
10 de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
11 Taenzer AH et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
12 Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
13 McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
14 Estimate: Masimo data on file.
15 http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.
Patient SafetyNet is a supplemental remote monitoring, patient surveillance, and clinician notification system that works in conjunction with Masimo and third-party bedside monitoring devices to display near real-time data at central stations. RAM with RRa uses an acoustic transducer positioned on the patient’s neck to provide noninvasive, continuous respiration monitoring.
Hypothesizing that postoperative desaturation and bradypnea might occur even in non-ICU patients without serious complications, and in patients who did not undergo major surgery, Drs. Masashi Ishikawa and Atsuhiro Sakamoto set up a centralized postoperative monitoring system in the general ward to investigate how common these events are for such patients (and what might predict them). They analyzed demographic and monitoring data from 1,064 adult patients who underwent general anesthesia for various surgical procedures over a four-month period. The patients were monitored using a pulse oximeter and an RRa sensor for at least 8 hours after surgery, data which were automatically transferred to Patient SafetyNet.
From the data stored on the Patient SafetyNet, the researchers were able to retrospectively analyze the incidence of desaturation (defined as SpO2 < 90 percent for > 10 seconds) and bradypnea (defined as respiratory rate < eight breaths/minute for > two minutes). They found that 12.1 percent of patients exhibited desaturation (244 events among 129 patients), with most occurring after the termination of oxygen administration, and 50.8 percent of the events occurring more than eight hours after surgery. They found that 5.1 percent of the patients exhibited bradypnea (112 times among 54 patients), with 72.3 percent of the events occurring during oxygen supplementation, and with the greatest incidence within the first hour after surgery. Age, body mass index, and current smoking status were significant risk factors for desaturation. Sleep apnea syndrome and postoperative opioid administration were significant risk factors for bradypnea. Age and postoperative opioid administration were significant risk factors for the combination of desaturation and bradypnea.
The researchers concluded, “Our study suggests that use of a continuous and centralized respiratory monitoring system for overnight postoperatively is desirable for postoperative management in the general ward, which would likely improve the safety of postoperative patients, especially those with risk factors for respiratory depression.”
The researchers commented on a number of methods of respiratory rate monitoring, stating, “Continuous and centralized monitoring of oxygen saturation and respiratory rate can detect respiratory depression before it results in critical events such as cardiac arrest. Several methods of respiratory rate monitoring are currently used, including manual counting of breaths by a caregiver, capnography, and transthoracic impedance measurement. Manual counting of breaths (such as auscultation) is an intermittent, labor-intensive and unreliable method. Capnography provides accurate and continuous monitoring, but requires a nasal or facial interface, which can be uncomfortable and may lead to failure if the interface is moved. Transthoracic impedance is non-invasive and can detect respiratory efforts, but is unable to detect alveolar hypoventilation caused by airway obstruction.”2-6
Additionally, the researchers commented on RAM with RRa, the respiratory rate monitoring method used in the current study, and referenced another study in which RRa and capnography were compared, stating: “RRa is an acoustic monitoring device that continuously measures respiratory rate, and is as accurate as capnography in extubated patients.7 Patient activities, such as talking, coughing and crying, affect the results of both RRa and capnography. The measurement errors during these activities are, however, not clinically relevant because they require that the patients are awake and breathing. Further, the RRa sensor appears to be well-tolerated and no more subject to error than capnography.7 RRa was found to be a reliable device and had fewer complications in this study.”
Masimo develops and produces an array of monitoring technologies, including measurements, sensors, patient monitors, and automation and connectivity solutions. Its mission is to improve patient outcomes and reduce the cost of care. Masimo SET Measure-through Motion and Low Perfusion pulse oximetry, introduced in 1995, has been shown in over 100 independent and objective studies to outperform other pulse oximetry technologies.8 Masimo SET has also been shown to help clinicians reduce severe retinopathy of prematurity in neonates,9 improve CCHD screening in newborns,10 and, when used for continuous monitoring with Masimo Patient SafetyNet in post-surgical wards, reduce rapid response team activations, ICU transfers, and costs.11-13 Masimo SET is estimated to be used on more than 100 million patients in hospitals and other healthcare settings around the world,14 and is the primary pulse oximetry at nine of the top 10 hospitals according to the 2019-20 U.S. News and World Report Best Hospitals Honor Roll.15 Masimo continues to refine SET and in 2018, announced that SpO2 accuracy on RD SET sensors during conditions of motion has been significantly improved, providing clinicians with even greater confidence that the SpO2 values they rely on accurately reflect a patient’s physiological status. In 2005, Masimo introduced rainbow Pulse CO-Oximetry technology, allowing noninvasive and continuous monitoring of blood constituents that previously could only be measured invasively, including total hemoglobin (SpHb), oxygen content (SpOC), carboxyhemoglobin (SpCO), methemoglobin (SpMet), Pleth Variability Index (PVi), RPVi (rainbow PVi), and Oxygen Reserve Index (ORi). In 2013, Masimo introduced the Root Patient Monitoring and Connectivity Platform, built from the ground up to be as flexible and expandable as possible to facilitate the addition of other Masimo and third-party monitoring technologies; key Masimo additions include Next Generation SedLine Brain Function Monitoring, O3 Regional Oximetry, and ISA Capnography with NomoLine sampling lines. Masimo’s family of continuous and spot-check monitoring Pulse CO-Oximeters includes devices designed for use in a variety of clinical and non-clinical scenarios, including tetherless, wearable technology, such as Radius-7 and Radius PPG, portable devices like Rad-67, fingertip pulse oximeters like MightySat Rx, and devices available for use both in the hospital and at home, such as Rad-97. Masimo hospital automation and connectivity solutions are centered around the Iris platform, and include Iris Gateway, Patient SafetyNet, Replica, Halo ION, UniView, and Doctella.
ORi and RPVi have not received U.S. Food and Drug Administration 510(k) clearance and are not available for sale in the United States.
References
1 Ishikawa M and Sakamoto A. Postoperative desaturation and bradypnea after general anesthesia in non-ICU patients: a retrospective evaluation. J Clin Monit Comput. 2 Mar 2019. https://doi.org/10.1007/s10877-019-00293-0.
2 Petterson MT, Begnoche VL, and Graybeal JM. The effect of motion on pulse oximetry and its clinical significance. Anesth Analg. 2007;105(6 Suppl):78–84.
3 Wilkinson JN, and Thanawala VU. Thoracic impedance monitoring of respiratory rate during sedation—is it safe? Anaesthesia. 2009;64(4):455–6.
4 Cohen KP, Ladd WM, Beams DM, Sheers WS, Radwin RG, Tompkins WJ, and Webster JG. Comparison of impedance and inductance ventilation sensors on adults during breathing, motion, and simulated airway obstruction. IEEE Trans Biomed Eng. 1997;44(7):555–66.
5 Drummond GB, Nimmo AF, and Elton RA. Thoracic impedance used for measuring chest wall movement in postoperative patients. Br J Anaesth. 1996;77(3):327–32.
6 Brouillette RT, Morrow AS, Weese-Mayer DE, and Hunt CE. Comparison of respiratory inductive plethysmography and thoracic impedance for apnea monitoring. J Pediatr. 1987;111(3):377–83.
7 Mimoz O, Benard T, Gaucher A, Frasca D, and Debaene B. Accuracy of respiratory rate monitoring using a non-invasive acoustic method after general anaesthesia. Br J Anaesth. 2012 May;108(5):872–5.
8 Published clinical studies on pulse oximetry and the benefits of Masimo SET® can be found on our website at http://www.masimo.com. Comparative studies include independent and objective studies which are comprised of abstracts presented at scientific meetings and peer-reviewed journal articles.
9 Castillo A et al. Prevention of Retinopathy of Prematurity in Preterm Infants through Changes in Clinical Practice and SpO2 Technology. Acta Paediatr. 2011 Feb;100(2):188-92.
10 de-Wahl Granelli A et al. Impact of pulse oximetry screening on the detection of duct dependent congenital heart disease: a Swedish prospective screening study in 39,821 newborns. BMJ. 2009;Jan 8;338.
11 Taenzer AH et al. Impact of pulse oximetry surveillance on rescue events and intensive care unit transfers: a before-and-after concurrence study. Anesthesiology. 2010:112(2):282-287.
12 Taenzer A et al. Postoperative Monitoring – The Dartmouth Experience. Anesthesia Patient Safety Foundation Newsletter. Spring-Summer 2012.
13 McGrath SP et al. Surveillance Monitoring Management for General Care Units: Strategy, Design, and Implementation. The Joint Commission Journal on Quality and Patient Safety. 2016 Jul;42(7):293-302.
14 Estimate: Masimo data on file.
15 http://health.usnews.com/health-care/best-hospitals/articles/best-hospitals-honor-roll-and-overview.