10.29.15
St. Paul, Minn.-based Cardiovascular Systems Inc. (CSI) has enrolled its first two patients in the Optimize peripheral orbital atherectomy system study. Taking place in Europe, Optimize will evaluate the acute and long-term clinical outcomes of orbital atherectomy with adjunctive drug-coated balloon (DCB) angioplasty versus DCB angioplasty alone for treatment of peripheral artery disease (PAD). Specifically, the study will look at patients with calcified below the knee (BTK) lesions. Optimize also will compare the economic outcomes between the patient groups.
Marianne Brodmann, M.D., director of the division of angiology, Medical University of Graz, Austria, performed the first procedure on October 28 together with Hannes Deutschmann, M.D., director of the vascular and interventional department of radiology, and Franz Hafner, M.D.
“We are excited to spearhead the study of CSI’s orbital atherectomy technology in Europe,” said Brodmann. “Below the knee PAD is associated with a higher prevalence of calcium than above the knee PAD. We look forward to evaluating the potential outcome benefit of using CSI’s orbital atherectomy system to remove calcified plaque prior to DCB angioplasty in this high-risk patient population.”
Optimize is a prospective, randomized, multi-center, post-market pilot study using CSI’s peripheral OAS to perform atherectomy procedures in conjunction with drug coated balloons. Up to 50 subjects may be enrolled at up to 10 study sites throughout the continent.
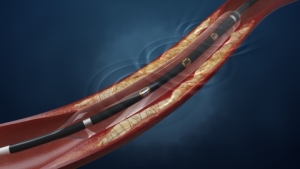
Millions of patients with PAD may benefit from treatment with orbital atherectomy utilizing the peripheral OAS, minimally invasive catheter systems developed and manufactured by CSI. The orbital atherectomy systems use a diamond-coated crown, attached to an orbiting shaft, which sands away plaque while preserving healthy vessel tissue — a critical factor in preventing reoccurrences. Balloon angioplasty and stents have significant shortcomings in treating hard, calcified lesions. Stents are prone to fractures and high recurrence rates, and treatment of hard, calcified lesions may lead to vessel damage and suboptimal results.
“Studying the combination of orbital atherectomy and drug-coated balloon angioplasty is an important step in our commitment to minimizing the adverse consequences of PAD for the millions of people afflicted with the disease,” said David L. Martin, president and CEO of CSI. “Our goal is to show that for calcified BTK arteries, pre-treatment with orbital atherectomy followed with DCB, will provide incremental benefits versus DCB angioplasty alone.”
CSI makes technology to treat vascular and coronary disease.
Marianne Brodmann, M.D., director of the division of angiology, Medical University of Graz, Austria, performed the first procedure on October 28 together with Hannes Deutschmann, M.D., director of the vascular and interventional department of radiology, and Franz Hafner, M.D.
“We are excited to spearhead the study of CSI’s orbital atherectomy technology in Europe,” said Brodmann. “Below the knee PAD is associated with a higher prevalence of calcium than above the knee PAD. We look forward to evaluating the potential outcome benefit of using CSI’s orbital atherectomy system to remove calcified plaque prior to DCB angioplasty in this high-risk patient population.”
Optimize is a prospective, randomized, multi-center, post-market pilot study using CSI’s peripheral OAS to perform atherectomy procedures in conjunction with drug coated balloons. Up to 50 subjects may be enrolled at up to 10 study sites throughout the continent.
Millions of patients with PAD may benefit from treatment with orbital atherectomy utilizing the peripheral OAS, minimally invasive catheter systems developed and manufactured by CSI. The orbital atherectomy systems use a diamond-coated crown, attached to an orbiting shaft, which sands away plaque while preserving healthy vessel tissue — a critical factor in preventing reoccurrences. Balloon angioplasty and stents have significant shortcomings in treating hard, calcified lesions. Stents are prone to fractures and high recurrence rates, and treatment of hard, calcified lesions may lead to vessel damage and suboptimal results.
“Studying the combination of orbital atherectomy and drug-coated balloon angioplasty is an important step in our commitment to minimizing the adverse consequences of PAD for the millions of people afflicted with the disease,” said David L. Martin, president and CEO of CSI. “Our goal is to show that for calcified BTK arteries, pre-treatment with orbital atherectomy followed with DCB, will provide incremental benefits versus DCB angioplasty alone.”
CSI makes technology to treat vascular and coronary disease.