Maria Shepherd, President and Founder, Medi-Vantage05.09.23
Staffing obstacles such as workforce shortages were the top pain point for CEOs in community hospitals in 2022, overshadowing the persistent issue of financial problems for the second year in the American College of Healthcare Executives' (ACHE) most recent annual survey.1 This data was corroborated by hospital administrator presentations at this year’s JP Morgan Healthcare Meeting in San Francisco.
The ACHE survey from member CEOs (n=281) ranked issues of immediate concern to hospital principals. Before staffing topped the list in the previous year’s survey, financial challenges had rated first for 16 years.
“Hospitals need to take both long- and short-term measures to address critical workforce issues so they can continue to provide safe, high-quality care now and in the future,” said Deborah J. Bowen, president and CEO of ACHE.
“Longer-term solutions include strengthening the workforce pipeline through creative partnerships, such as those with colleges to grow the number of nurses and technicians. More immediate solutions include supporting and developing all staff, building staff resilience, organizing services to reflect the realities of the labor market, and exploring alternative models of care.”2
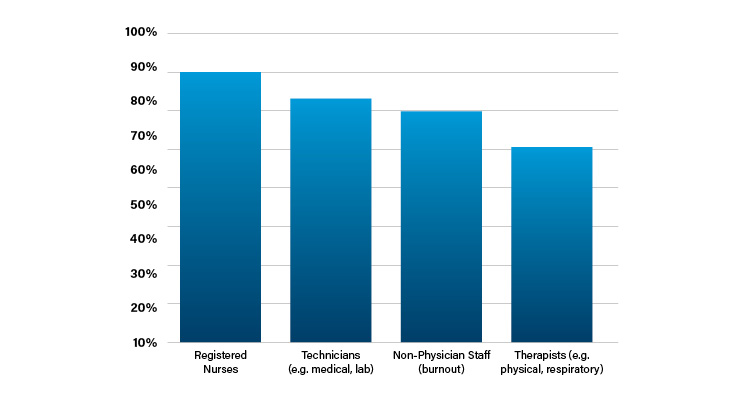
That doesn’t mean financial challenges don’t still exist. Eighty-nine percent of CEOs reported increasing costs for workforce, supplies, etc. Approximately 66% stated they were troubled about reducing operating costs, 63% cited ongoing issues with Medicaid reimbursement, 58% identified managed care and other commercial insurance payments, and 52% pointed to reductions to government funding.1
A light at the end of the tunnel is ACHE’s survey on hospital CEO turnover.3 In the roughly 4,400 hospitals tracked by the ACHE organization, hospital CEO turnover has remained consistent through the COVID years and from before (Table 2). This is important information. These are the leaders of our hospitals and the people that have the institutional knowledge needed to take us through these difficult years.
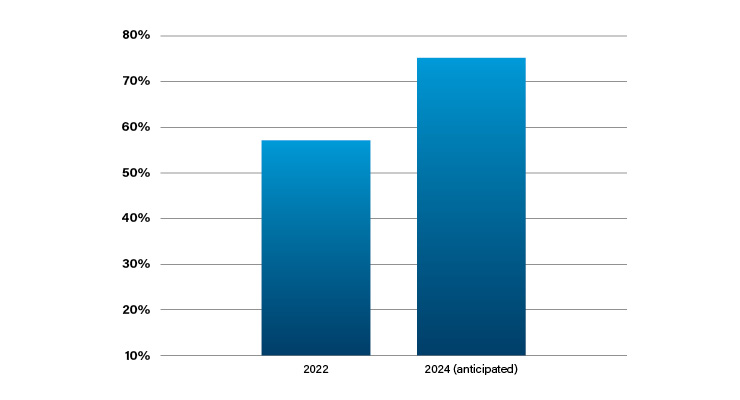
According to a recent survey, the use of remote physiologic monitoring (RPM) is growing. RPM is a virtual care patient tool enabling physicians to remotely monitor a patient’s vital signs such as heart rate and blood pressure. The survey revealed the current (i.e., 2022) usage of RPM as well as the anticipated number within two years. Twenty-five percent of those surveyed reported not yet using RPM, but expected to start within the next two years (Table 3).4 For the healthcare industry, this is rapid adoption.
The majority of RPM users indicated remote physiologic monitoring offers substantial benefits to patients, staff, and ROI.4
RPM devices help patients better understand their health on a long-term basis. When a patient is engaging with their health on a routine basis using RPM medical devices, they are more likely to see positive health outcomes.
The question for medtech developers is how and when to develop an RPM component for their medical device. There are many examples of RPM with devices like CPAP or joint replacement, where the development of an RPM device brings meaningful patient data that helps all stakeholders in patient care.
References
Maria Shepherd has more than 20 years of experience in marketing in small startups and top-tier companies. She founded Medi-Vantage, which provides marketing and business strategy for the medical device industry. She can be reached at mshepherd@medi-vantage.com. Visit her website at www.medi-vantage.com.
The ACHE survey from member CEOs (n=281) ranked issues of immediate concern to hospital principals. Before staffing topped the list in the previous year’s survey, financial challenges had rated first for 16 years.
“Hospitals need to take both long- and short-term measures to address critical workforce issues so they can continue to provide safe, high-quality care now and in the future,” said Deborah J. Bowen, president and CEO of ACHE.
“Longer-term solutions include strengthening the workforce pipeline through creative partnerships, such as those with colleges to grow the number of nurses and technicians. More immediate solutions include supporting and developing all staff, building staff resilience, organizing services to reflect the realities of the labor market, and exploring alternative models of care.”2
Why This Is Important
Under the category of workforce challenges, CEOs identified shortages of several groups at the top of the list—registered nurses, technicians, non-physician staff, and therapists (Table 1).1That doesn’t mean financial challenges don’t still exist. Eighty-nine percent of CEOs reported increasing costs for workforce, supplies, etc. Approximately 66% stated they were troubled about reducing operating costs, 63% cited ongoing issues with Medicaid reimbursement, 58% identified managed care and other commercial insurance payments, and 52% pointed to reductions to government funding.1
A light at the end of the tunnel is ACHE’s survey on hospital CEO turnover.3 In the roughly 4,400 hospitals tracked by the ACHE organization, hospital CEO turnover has remained consistent through the COVID years and from before (Table 2). This is important information. These are the leaders of our hospitals and the people that have the institutional knowledge needed to take us through these difficult years.
How Can Medtech Help?
Amid all the disruption of the past three years, alternative care delivery methods such as telehealth, virtual care, and in-home care have materialized as practical options for alleviating many of the challenges of the pandemic, but also overload in the U.S. healthcare system. Remote patient monitoring and remote therapeutic monitoring are two of these reimbursable alternative care delivery tools that support telehealth, virtual care, and in-home care.According to a recent survey, the use of remote physiologic monitoring (RPM) is growing. RPM is a virtual care patient tool enabling physicians to remotely monitor a patient’s vital signs such as heart rate and blood pressure. The survey revealed the current (i.e., 2022) usage of RPM as well as the anticipated number within two years. Twenty-five percent of those surveyed reported not yet using RPM, but expected to start within the next two years (Table 3).4 For the healthcare industry, this is rapid adoption.
The majority of RPM users indicated remote physiologic monitoring offers substantial benefits to patients, staff, and ROI.4
- 79%—Positive impact on patient care
- 73%—Improves patient satisfaction
- 66%—Improves patient outcomes
- 64%—Improves staff satisfaction
- 60%—Has a high ROI
- 43%—Leads to fewer emergency department visits or hospital admissions
Devices Approved for RPM
Any device used (and billed) must meet FDA’s definition of a medical device. The RPM device must digitally collect and automatically upload the physiologic data of the patient. It is unclear if patient data can be self-recorded or self-reported by the patient. Devices must transmit valid physiologic data necessary to diagnose or treat, and allow understanding of the patient’s condition so physicians can create a plan of treatment and further manage it through RPM.5 Examples include:- Spirometer
- Blood pressure cuff
- Pulse oximeter
- Glucometer
- Thermometer
- Heart rate monitor
Challenges of Using RPM
While the aforementioned survey is an indicator RPM growth is trending and needed, it also shows all is not perfect in the RPM world. The majority of survey respondents from practices using RPM say it can help improve patient outcomes and may contribute to patient satisfaction. However, respondents also mentioned considerable challenges associated with implementing RPM, including changes in staff workflows, poor patient engagement, and reimbursement challenges.The Medi-Vantage Perspective
The challenges cited for RPM sound like opportunities. Remote patient monitoring medical devices allow healthcare providers to monitor, analyze, and report on any patient’s acute or chronic condition from outside of a hospital or clinic. RPM devices enable care providers real-time ability to check on a patient’s condition, empowering proactive clinical decisions.RPM devices help patients better understand their health on a long-term basis. When a patient is engaging with their health on a routine basis using RPM medical devices, they are more likely to see positive health outcomes.
The question for medtech developers is how and when to develop an RPM component for their medical device. There are many examples of RPM with devices like CPAP or joint replacement, where the development of an RPM device brings meaningful patient data that helps all stakeholders in patient care.
References
Maria Shepherd has more than 20 years of experience in marketing in small startups and top-tier companies. She founded Medi-Vantage, which provides marketing and business strategy for the medical device industry. She can be reached at mshepherd@medi-vantage.com. Visit her website at www.medi-vantage.com.