Leo Gelera, Quality Manager, FMI12.21.17
Medical device manufacturers are responsible for ensuring that all components, even those produced externally, comply with all relevant ISO guidelines. To this end, they must verify the quality management systems of their suppliers fulfill all the necessary requirements. This is all the more urgent now as two crucial standards have recently been revised. Suppliers must ensure their processes conform to the new EN ISO 9001 by September 2018 and to the revised EN ISO 13485 by March 2019. If a component manufacturer doesn’t obtain certification in time, the OEM will have to switch suppliers, at least in the short term. If this is not an option, the worst-case scenario means the manufacturer will be unable to market their product in Europe.
For OEMs, it is not always easy to ensure that vendor parts conform to ISO standards. In the best-case scenario, the quality management systems of a firm’s suppliers are efficient enough to recognize risks and prevent faults and defects. The medical device manufacturer recognizes how effective the internal processes are using factors such as certification per ISO standards, risk management for product realization, the use of a Corrective and Preventive Actions (CAPA) program, and the significance of quality as part of the corporate culture.
Certification According to the Revised Standards Is Essential
As both EN ISO 9001, which specifies the minimum requirements on QM systems, and EN ISO 13485 have been recently revised, the priority for OEMs at the moment is to ensure that suppliers comply with the deadlines for certifications according to these revised standards. The key objective of the new standards is to improve the risk management among suppliers of the medical industry. Among other things, this is accomplished with a more intensive focus on the need for controls throughout the entire supplier process chain.
In order to complete the certification process successfully within the deadline, the supplier can engage an external consultant or use internal personnel resources. If the latter approach is chosen, the office responsible for the certification should be contacted. This office will provide advice on the best process and provide the checklists, which are also used for later evaluation. In addition, the quality manager responsible for the project should attend a training session about the requirements of the new standards and be certified as the lead auditor. If this occurs, the next step is to carry out a gap analysis. In doing so, the requirements of the new guidelines are compared with the current processes at the supplier’s premises and steps for their adjustment are identified.
Pressing Deadline
The companies should not dawdle. The regulatory bodies are allowing the exact amount of time required for successful certification between the publication of the standard and the end of the deadline. By September 2017, for example, the gap analysis should have been performed and a precise plan for the upgrade should have been developed as well. The key elements of ISO 13485:2016 are the training and CAPA program along with more accurate supplier checks.
There can be grave consequences for an OEM if it obtains components from a supplier that has a quality management system not certified in accordance with ISO 13485:2016. This certification is a fundamental prerequisite for being able to market a medical device in the European Union. As a result, it is one of the standard requirements of suppliers for many OEMs. If the deadline is not complied with, the medical device manufacturer must not use these components in its production processes until the non-compliance is resolved. As OEMs normally only have one supplier for a specific component, there is the risk that existing orders might not be fulfilled. If the medical device manufacturer has the impression that its supplier is not currently far enough into the certification process, the OEM should at least request the supplier’s action plan and schedule for the adjustments in order to get a more accurate overview and be able to take action in good time.
Related Questions and Answers
Following is a brief Q&A that further addresses common questions related to this topic that should be of interest to medical device manufacturers or, at the very least, encourage a discussion between an OEM and its supply chain partners.
Q: ISO certification is just one factor that provides OEMs with information about how good the quality management of a supplier is. What about the implementation of risk management processes into product realization?
A: In the ISO standards in question, suppliers are required to implement risk management processes into the field of product realization. However, what these processes should look like exactly is kept deliberately vague. As a result, companies have more creative leeway and can take the most effective measures. Naturally, this is connected with a continual learning process, which can still be accelerated a little—for example, through comparison with the process of similar suppliers. Typical questions are:
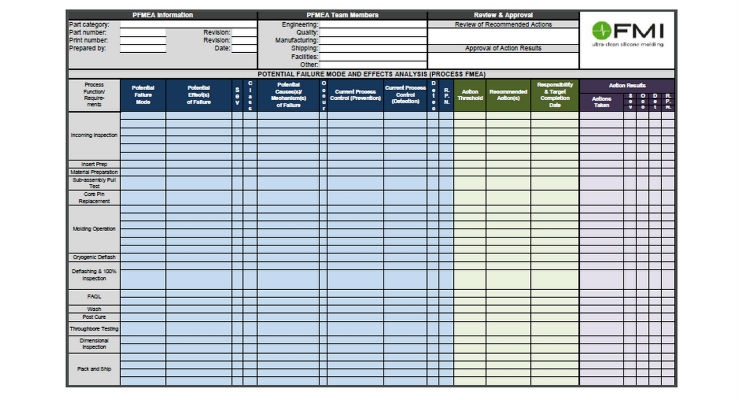
The answers to these questions also provide OEMs with information for their appraisal of supplier processes. FMI, for example, has incorporated various processes over the entire product realization stage, including various Failure Mode and Effects Analyses (FMEAs), part-specific control plans and operating instructions, error recognition in each process, dimensional checks, and FAQL and Final Lot Release Inspections. The implementation of process FMEAs is particularly recommended. Their advantage is that potential error sources are identified before the actual production and countermeasures can be taken as early as possible in the process chain. This prevents any faulty products being delivered.
Q: How important are CAPA programs?
A: Having an efficient CAPA system is ultimately essential for any company and any organization. CAPA are generally triggered when an error occurs, whether internally or externally. Its purpose is to understand the cause, the scope, and the effects of the incident. In the best-case scenario, it can help to correct arising errors and specify measures that will prevent a reoccurrence of the fault or defect in the future. Subsequently, the effectiveness of the countermeasure should also be checked. If such an analysis including the derived measures is not carried out, there is the risk the error will reoccur repeatedly.
Q: What role must quality play as part of the corporate culture?
A: The aim of a supplier must ultimately be to make collaboration with the OEM as simple and low maintenance as possible. Preferably, the supplier shouldn’t even appear on the radar of the medical device manufacturer because its quality performance is flawless. This is where the “quality culture” is crucial for a supplier. Every employee must understand the central role he or she plays in quality and what far-reaching consequences there can be if just one component is defective. Within the industry, many components are manufactured that later contribute to saving or preserving human life. Employees should be given precise information about the significance of a component and how much depends on it functioning accurately. This also enhances an employee’s appreciation of their own work.
Leo Gelera is the quality manager at FMI, a business unit of Flexan LLC. Founded in 1946, Flexan LLC is a global manufacturer of high-precision elastomer parts for a wide range of industry applications. It operates out of four manufacturing facilities with about 800 employees. Its Flexan unit focuses on custom molding while its FMI business delivers cleanroom-manufactured silicone rubber components for use in Class II disposable and Class III implantable medical devices. High-volume custom molded elastomer and cleanroom silicone rubber is offered from the Flexan-Suzhou factory. Flexan’s MEDRON division serves a wide range of outsourcing capabilities, including high volume manufacturing, customer private label capability, design engineering, product development, and prototyping. MEDRON's expertise comprises a wide range of materials, including medical grade urethanes and engineering thermoplastics. The firm is owned by Linden Capital Partners, a Chicago-based private equity firm focused exclusively on leveraged buyouts in the healthcare and life sciences industries.
For OEMs, it is not always easy to ensure that vendor parts conform to ISO standards. In the best-case scenario, the quality management systems of a firm’s suppliers are efficient enough to recognize risks and prevent faults and defects. The medical device manufacturer recognizes how effective the internal processes are using factors such as certification per ISO standards, risk management for product realization, the use of a Corrective and Preventive Actions (CAPA) program, and the significance of quality as part of the corporate culture.
Certification According to the Revised Standards Is Essential
As both EN ISO 9001, which specifies the minimum requirements on QM systems, and EN ISO 13485 have been recently revised, the priority for OEMs at the moment is to ensure that suppliers comply with the deadlines for certifications according to these revised standards. The key objective of the new standards is to improve the risk management among suppliers of the medical industry. Among other things, this is accomplished with a more intensive focus on the need for controls throughout the entire supplier process chain.
In order to complete the certification process successfully within the deadline, the supplier can engage an external consultant or use internal personnel resources. If the latter approach is chosen, the office responsible for the certification should be contacted. This office will provide advice on the best process and provide the checklists, which are also used for later evaluation. In addition, the quality manager responsible for the project should attend a training session about the requirements of the new standards and be certified as the lead auditor. If this occurs, the next step is to carry out a gap analysis. In doing so, the requirements of the new guidelines are compared with the current processes at the supplier’s premises and steps for their adjustment are identified.
Pressing Deadline
The companies should not dawdle. The regulatory bodies are allowing the exact amount of time required for successful certification between the publication of the standard and the end of the deadline. By September 2017, for example, the gap analysis should have been performed and a precise plan for the upgrade should have been developed as well. The key elements of ISO 13485:2016 are the training and CAPA program along with more accurate supplier checks.
There can be grave consequences for an OEM if it obtains components from a supplier that has a quality management system not certified in accordance with ISO 13485:2016. This certification is a fundamental prerequisite for being able to market a medical device in the European Union. As a result, it is one of the standard requirements of suppliers for many OEMs. If the deadline is not complied with, the medical device manufacturer must not use these components in its production processes until the non-compliance is resolved. As OEMs normally only have one supplier for a specific component, there is the risk that existing orders might not be fulfilled. If the medical device manufacturer has the impression that its supplier is not currently far enough into the certification process, the OEM should at least request the supplier’s action plan and schedule for the adjustments in order to get a more accurate overview and be able to take action in good time.
Related Questions and Answers
Following is a brief Q&A that further addresses common questions related to this topic that should be of interest to medical device manufacturers or, at the very least, encourage a discussion between an OEM and its supply chain partners.
Q: ISO certification is just one factor that provides OEMs with information about how good the quality management of a supplier is. What about the implementation of risk management processes into product realization?
A: In the ISO standards in question, suppliers are required to implement risk management processes into the field of product realization. However, what these processes should look like exactly is kept deliberately vague. As a result, companies have more creative leeway and can take the most effective measures. Naturally, this is connected with a continual learning process, which can still be accelerated a little—for example, through comparison with the process of similar suppliers. Typical questions are:
- What risk management tools are used?
- Are risk management practices used during the entire production process?
- How efficient are these?
The answers to these questions also provide OEMs with information for their appraisal of supplier processes. FMI, for example, has incorporated various processes over the entire product realization stage, including various Failure Mode and Effects Analyses (FMEAs), part-specific control plans and operating instructions, error recognition in each process, dimensional checks, and FAQL and Final Lot Release Inspections. The implementation of process FMEAs is particularly recommended. Their advantage is that potential error sources are identified before the actual production and countermeasures can be taken as early as possible in the process chain. This prevents any faulty products being delivered.
Q: How important are CAPA programs?
A: Having an efficient CAPA system is ultimately essential for any company and any organization. CAPA are generally triggered when an error occurs, whether internally or externally. Its purpose is to understand the cause, the scope, and the effects of the incident. In the best-case scenario, it can help to correct arising errors and specify measures that will prevent a reoccurrence of the fault or defect in the future. Subsequently, the effectiveness of the countermeasure should also be checked. If such an analysis including the derived measures is not carried out, there is the risk the error will reoccur repeatedly.
Q: What role must quality play as part of the corporate culture?
A: The aim of a supplier must ultimately be to make collaboration with the OEM as simple and low maintenance as possible. Preferably, the supplier shouldn’t even appear on the radar of the medical device manufacturer because its quality performance is flawless. This is where the “quality culture” is crucial for a supplier. Every employee must understand the central role he or she plays in quality and what far-reaching consequences there can be if just one component is defective. Within the industry, many components are manufactured that later contribute to saving or preserving human life. Employees should be given precise information about the significance of a component and how much depends on it functioning accurately. This also enhances an employee’s appreciation of their own work.
Leo Gelera is the quality manager at FMI, a business unit of Flexan LLC. Founded in 1946, Flexan LLC is a global manufacturer of high-precision elastomer parts for a wide range of industry applications. It operates out of four manufacturing facilities with about 800 employees. Its Flexan unit focuses on custom molding while its FMI business delivers cleanroom-manufactured silicone rubber components for use in Class II disposable and Class III implantable medical devices. High-volume custom molded elastomer and cleanroom silicone rubber is offered from the Flexan-Suzhou factory. Flexan’s MEDRON division serves a wide range of outsourcing capabilities, including high volume manufacturing, customer private label capability, design engineering, product development, and prototyping. MEDRON's expertise comprises a wide range of materials, including medical grade urethanes and engineering thermoplastics. The firm is owned by Linden Capital Partners, a Chicago-based private equity firm focused exclusively on leveraged buyouts in the healthcare and life sciences industries.