Jade Boyd, Rice University02.27.18
The National Science Foundation has awarded $10 million to a Rice University-led team that hopes to create wearable and point-of-care microscopes that use on-chip illumination and sensing to non-invasively aid in the diagnosis and monitoring of nearly 100 health conditions that today require a biopsy or blood test.
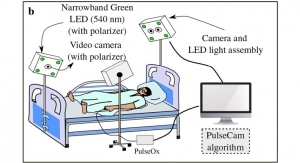
“The project will produce a platform technology for in vivo, 3D tissue imaging, with the aim of being able to point a camera to a part of the body and see live biology below the skin without making an incision or drawing blood,” said Rice Professor Ashutosh Sabharwal, the principal investigator on the grant.
Sabharwal’s team, which includes 11 co-investigators from Rice, Carnegie Mellon, Harvard, MIT and Cornell, is one of three groups to win new five-year grants today from the NSF’s Expeditions in Computing program. Expeditions is an interdisciplinary NSF effort that constitutes the agency’s largest single investment in computer and information science research. Since 2008, NSF has invested more than $200 million in Expeditions projects.
“Expeditions supports transformative research, and our goal is to create miniaturized, light-based microscopes for use in wearables, point-of-care, bedside diagnostics, ambulances, operating rooms and more,” said Sabharwal, professor of electrical and computer engineering.
Anyone who has pointed a flashlight at their palm to make their hand glow knows that light can travel through the body. But visible light scatters so much as it passes through soft tissue that it has not been useful for medical imaging.
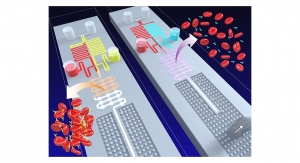
Sabharwal’s team will attempt to unravel this scattered light puzzle with a technique called “computational scatterography.” They’ll use a combination of mathematical algorithms, camera design and imaging sensors to reverse engineer the path of scattered light.

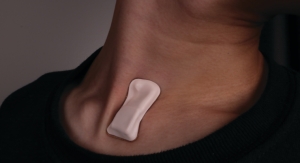
As this image illustrates, light from a smartphone LED flash can travel through more than a centimeter of skin and soft tissue. This low-power, non-ionizing light is safe for biomedical imaging and cheap to produce, control and sense. Image courtesy of A. Sabharwal/Rice University.
“Basically, we’re trying to ‘de-scatter’ the light,” said computational imaging expert and Rice co-investigator Ashok Veeraraghavan, associate professor of electrical and computer engineering. “In engineering, we call this an inverse problem. Geoscientists use similar inverse techniques on seismic waves to resolve pictures of Earth’s deep interior. Our task, in some ways, is even more complicated because the amount of light scattering that takes place in even a few millimeters of tissue far exceeds other problems.”
Sabharwal pointed to white blood cell count (WBC) tests as an example of the project’s potential impact. In the U.S., oncologists use millions of WBC tests each week to monitor chemotherapy patients. WBC tests require a finger prick or blood draw and a laboratory, which means they can be performed only at hospitals and clinics.
“Imagine a wearable device no larger than a watch that uses sensors to continuously measure white blood cell count and wirelessly communicate with the oncologist’s office,” Sabharwal said. “The patient could go about their daily life. They’d only have to go to the hospital if there was a problem.”
Sabharwal said a crucial thing to understand about the scatterography project is that it won’t aid in managing just one or two health care problems.
“If we succeed, this isn’t just one product,” he said. “It’s a platform technology that will be able spinoff into many products that can be used in the care of nearly 100 health conditions.”
“The project will produce a platform technology for in vivo, 3D tissue imaging, with the aim of being able to point a camera to a part of the body and see live biology below the skin without making an incision or drawing blood,” said Rice Professor Ashutosh Sabharwal, the principal investigator on the grant.
Sabharwal’s team, which includes 11 co-investigators from Rice, Carnegie Mellon, Harvard, MIT and Cornell, is one of three groups to win new five-year grants today from the NSF’s Expeditions in Computing program. Expeditions is an interdisciplinary NSF effort that constitutes the agency’s largest single investment in computer and information science research. Since 2008, NSF has invested more than $200 million in Expeditions projects.
“Expeditions supports transformative research, and our goal is to create miniaturized, light-based microscopes for use in wearables, point-of-care, bedside diagnostics, ambulances, operating rooms and more,” said Sabharwal, professor of electrical and computer engineering.
Anyone who has pointed a flashlight at their palm to make their hand glow knows that light can travel through the body. But visible light scatters so much as it passes through soft tissue that it has not been useful for medical imaging.
Sabharwal’s team will attempt to unravel this scattered light puzzle with a technique called “computational scatterography.” They’ll use a combination of mathematical algorithms, camera design and imaging sensors to reverse engineer the path of scattered light.

As this image illustrates, light from a smartphone LED flash can travel through more than a centimeter of skin and soft tissue. This low-power, non-ionizing light is safe for biomedical imaging and cheap to produce, control and sense. Image courtesy of A. Sabharwal/Rice University.
“Basically, we’re trying to ‘de-scatter’ the light,” said computational imaging expert and Rice co-investigator Ashok Veeraraghavan, associate professor of electrical and computer engineering. “In engineering, we call this an inverse problem. Geoscientists use similar inverse techniques on seismic waves to resolve pictures of Earth’s deep interior. Our task, in some ways, is even more complicated because the amount of light scattering that takes place in even a few millimeters of tissue far exceeds other problems.”
Sabharwal pointed to white blood cell count (WBC) tests as an example of the project’s potential impact. In the U.S., oncologists use millions of WBC tests each week to monitor chemotherapy patients. WBC tests require a finger prick or blood draw and a laboratory, which means they can be performed only at hospitals and clinics.
“Imagine a wearable device no larger than a watch that uses sensors to continuously measure white blood cell count and wirelessly communicate with the oncologist’s office,” Sabharwal said. “The patient could go about their daily life. They’d only have to go to the hospital if there was a problem.”
Sabharwal said a crucial thing to understand about the scatterography project is that it won’t aid in managing just one or two health care problems.
“If we succeed, this isn’t just one product,” he said. “It’s a platform technology that will be able spinoff into many products that can be used in the care of nearly 100 health conditions.”