National Institute of Biomedical Imaging and Bioengineering12.14.16
Researchers funded by the National Institute of Biomedical Imaging and Bioengineering have created a microfluidic device that could lead to faster, more sophisticated, and lower cost methods for screening drugs for liver toxicity—before the drugs are moved into human trials. The device produces millions of droplets containing microtissues that are made up of two different types of liver cells organized to mimic real liver tissue. The researchers detailed their new technology in the March 2016 issue of the journal Lab on a Chip.
Currently, scientists assess drugs for liver toxicity either by testing them in animals or by applying them directly to liver cells grown in and adhering to the bottom of a plastic dish. While the latter approach enables high-throughput screening, it fails to consider the complex 3D organization of liver tissue, which involves multiple types of cells and an extracellular matrix—the collection of molecules that surrounds cells to provide structural and biochemical support. Interactions among different cell types and with the extracellular matrix all contribute to a normally functioning organ. Thus, testing drugs on liver cells in a dish is generally not an accurate predictor of how a drug will affect the liver in real life.
Recent research by other teams has led to the development of “organ on a chip” models of the liver that more closely resemble the intact organ. The chips are platforms (about the size of a thumbdrive) that are engineered to support multiple types of liver cells in a 3D environment. Tiny channels in the platform carry nutrients to the cells in order to keep them alive and healthy. Yet, these chips can be difficult to make, may lack uniformity, and aren’t easily modified. This limits the number of drugs and conditions that can be screened using the chips.
In an effort to overcome these limitations, researchers led by David Weitz, Ph.D., Professor of Physics and Applied Physics at Harvard University, have created a microfluidic chip that can quickly and precisely generate functioning human liver microtissues inside of droplets. The system can generate up to one thousand droplets per second, which can then be used to screen a large number of drugs in different combinations and at different doses.
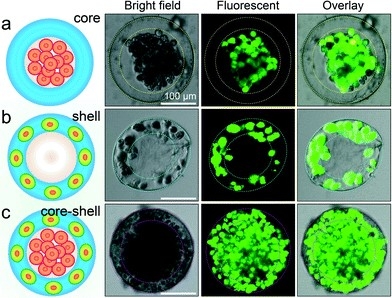
This figure shows a series of images taken with a microscope of a) hepatocytes only in the core of the droplet b) fibroblasts only in the shell of the droplet and c) hepatocytes and fibroblasts combined within different compartments of the same droplet. The cells were visualized using fluorescent markers.
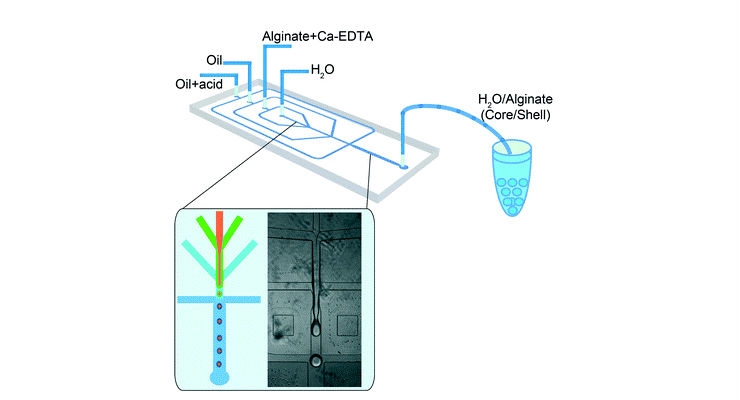
Weitz’ microfluidic chip is a platform that contains a system of extremely narrow, interconnected concentric channels (each channel is about the diameter of a strand of hair). In the first step of the platform, a saline-based solution of hepatocytes, the primary cells that contribute to the liver’s function, flows down a channel until it intersects with a gel-like solution of fibroblasts, the cells found in the liver’s extracellular matrix that secrete collagen and provide structural support to hepatocytes. Due to the chemical properties of the two different solutions and the physics of fluids travelling in narrow spaces, the fibroblasts hug the sides of the channel while the hepatocytes flow down the middle.
Next, this mixture of cells intersects with a solution of oil, which acts as a brake and causes a droplet to pinch off. Finally, these newly made droplets meet a mildly acidic solution, which causes their outer gel layer to become set, locking the cells into their respective positions. The end result is a droplet with a watery core filled with hepatocytes and a gelatinous shell comprised of fibroblasts.
While droplets containing hepatocytes have previously been created, this is the first time a microfluidic device has been able to produce droplets containing two types of cells confined to different regions, with high viability, in a highly reproducible way, and at such a fast speed.
Once made, the droplets can be used in a variety of settings in which they are exposed to a drug or combination of drugs to assess liver toxicity. Weitz said this type of system increases the number of experiments that can be carried out by several orders of magnitude:
“Each droplet is like a mini experiment. Normally, if we are running experiments, say in test tubes, we need a milliliter of fluid per test tube. If we were to do a million experiments, we would need a thousand liters of fluid. That’s the equivalent of a thousand milk jugs! Here, each droplet is only a nanoliter, so we can do the whole experiment with one milliliter of fluid, meaning we can do a million more experiments with the same amount of fluid.”
And because so many experiments can be run in such a short amount of time and for so little cost, more drugs can be screened at different doses and in combination with other drugs. This is important because many drugs are only toxic to the liver at a high dose or when taken with another drug.
“This new process gives researchers the flexibility to assemble some of the cellular components of the liver in different combinations and proportions to see how they influence each other, and how they might work together to make a functional tissue. Plus, the assembly is faster, more reliable, and less expensive than current methods of making liver tissue models,” said Rosemarie Hunziker, Ph.D., program director of Tissue Engineering at NIBIB.
The work was funded in part by the National Institute of Biomedical Imaging and Bioengineering, part of the National Institutes of Health (NIH) through grants EB014703.
Find more information on the study here.
Currently, scientists assess drugs for liver toxicity either by testing them in animals or by applying them directly to liver cells grown in and adhering to the bottom of a plastic dish. While the latter approach enables high-throughput screening, it fails to consider the complex 3D organization of liver tissue, which involves multiple types of cells and an extracellular matrix—the collection of molecules that surrounds cells to provide structural and biochemical support. Interactions among different cell types and with the extracellular matrix all contribute to a normally functioning organ. Thus, testing drugs on liver cells in a dish is generally not an accurate predictor of how a drug will affect the liver in real life.
Recent research by other teams has led to the development of “organ on a chip” models of the liver that more closely resemble the intact organ. The chips are platforms (about the size of a thumbdrive) that are engineered to support multiple types of liver cells in a 3D environment. Tiny channels in the platform carry nutrients to the cells in order to keep them alive and healthy. Yet, these chips can be difficult to make, may lack uniformity, and aren’t easily modified. This limits the number of drugs and conditions that can be screened using the chips.
In an effort to overcome these limitations, researchers led by David Weitz, Ph.D., Professor of Physics and Applied Physics at Harvard University, have created a microfluidic chip that can quickly and precisely generate functioning human liver microtissues inside of droplets. The system can generate up to one thousand droplets per second, which can then be used to screen a large number of drugs in different combinations and at different doses.

This figure shows a series of images taken with a microscope of a) hepatocytes only in the core of the droplet b) fibroblasts only in the shell of the droplet and c) hepatocytes and fibroblasts combined within different compartments of the same droplet. The cells were visualized using fluorescent markers.
Next, this mixture of cells intersects with a solution of oil, which acts as a brake and causes a droplet to pinch off. Finally, these newly made droplets meet a mildly acidic solution, which causes their outer gel layer to become set, locking the cells into their respective positions. The end result is a droplet with a watery core filled with hepatocytes and a gelatinous shell comprised of fibroblasts.
While droplets containing hepatocytes have previously been created, this is the first time a microfluidic device has been able to produce droplets containing two types of cells confined to different regions, with high viability, in a highly reproducible way, and at such a fast speed.
Once made, the droplets can be used in a variety of settings in which they are exposed to a drug or combination of drugs to assess liver toxicity. Weitz said this type of system increases the number of experiments that can be carried out by several orders of magnitude:
“Each droplet is like a mini experiment. Normally, if we are running experiments, say in test tubes, we need a milliliter of fluid per test tube. If we were to do a million experiments, we would need a thousand liters of fluid. That’s the equivalent of a thousand milk jugs! Here, each droplet is only a nanoliter, so we can do the whole experiment with one milliliter of fluid, meaning we can do a million more experiments with the same amount of fluid.”
And because so many experiments can be run in such a short amount of time and for so little cost, more drugs can be screened at different doses and in combination with other drugs. This is important because many drugs are only toxic to the liver at a high dose or when taken with another drug.
“This new process gives researchers the flexibility to assemble some of the cellular components of the liver in different combinations and proportions to see how they influence each other, and how they might work together to make a functional tissue. Plus, the assembly is faster, more reliable, and less expensive than current methods of making liver tissue models,” said Rosemarie Hunziker, Ph.D., program director of Tissue Engineering at NIBIB.
The work was funded in part by the National Institute of Biomedical Imaging and Bioengineering, part of the National Institutes of Health (NIH) through grants EB014703.
Find more information on the study here.