Business Wire11.11.16
Glaukos Corporation, an ophthalmic medical technology company developing and commercializing breakthrough products and procedures for glaucoma treatment, announced that a study of 134 predominantly Hispanic eyes with open-angle glaucoma (OAG) showed mean intraocular pressure (IOP) of 12.9 mm Hg and a 61 percent decrease in mean medication burden one year following implantation of the iStent Trabecular Micro-Bypass Stent in combination with cataract surgery.
The retrospective, consecutive case series includes 168 eyes of 128 patients who underwent iStent implantation with concomitant cataract surgery, of which 134 eyes in 100 patients have been followed through one year. Study researchers reported that 87 percent of subjects had moderate to severe OAG and 80 percent were Hispanic, a population segment with a higher-than-average incidence and prevalence of OAG. Up to 21 percent of Hispanics are expected to develop OAG by age 80, according to a reference cited in the study.
All procedures in the series were performed by Mark J. Gallardo, M.D., at a single site in El Paso, Texas. Before surgery, patients were placed into three subgroups in accordance with the surgeon’s typical clinical practice and based on the patient’s IOP level, medication burden and treatment goal. In the 134 eyes with one-year postoperative follow-up, the safety profile was favorable and treatment success was achieved in all three subgroups as follows:
Group 1: Comprised of 65 eyes with controlled IOP on at least one ocular hypotensive medication preoperatively and a treatment goal to reduce medication burden while maintaining IOP control. One year following the procedure, medication burden decreased from a mean of 2.4 medications preoperatively to 0.6 at one year; this decrease was statistically significant (p<0.001). Further, mean IOP decreased to 12.7 mm Hg, compared to 13.6 mm Hg preoperatively.
Group 2: Comprised of 31 eyes with IOP not controlled on up to two ocular hypotensive medications preoperatively and a treatment goal to reduce IOP and maintain or reduce medication burden. One year following the procedure, all eyes had IOP of 18 mm Hg or lower with a statistically significant (p<0.001) reduction to a mean IOP of 12.6 mm Hg, compared to 19.1 mm Hg preoperatively. Medication burden decreased to a mean of 0.4 medications, compared to 1.1 preoperatively.
Group 3: Comprised of 40 eyes on three or more ocular hypotensive medications and/or uncontrolled IOP preoperatively with a treatment goal to reduce IOP in order to avoid filtering surgery. One year following the procedure, 95 percent (38 of 40 eyes) achieved their treatment goal. In these 38 eyes, mean IOP decreased to 13.6 mm Hg, compared to 19.3 mm Hg preoperatively, which was statistically significant (p< 0.001). Medication burden decreased to a mean of 1.8 medications, compared to 3.2 preoperatively.
“These data show that iStent in combination with cataract surgery can effectively reduce IOP and topical ocular hypotensive medication use in a mainly Hispanic patient population, including those with more advanced disease,” said Gallardo. “Importantly, these results were achieved in a real-life clinical setting, where the treatment goals differ by patient, based on their individual needs and disease state. The study’s high success rate overall and within each patient subgroup underscores the tangible benefits of using trabecular bypass stenting to manage IOP and medication burden in a demographically diverse glaucoma patient population.”
Typically associated with elevated IOP, glaucoma is characterized by progressive, irreversible and largely asymptomatic vision loss caused by optic nerve damage. It is a leading cause of blindness. According to Market Scope, more than 80 million people worldwide have glaucoma, including 4.5 million people in the United States. Open-angle glaucoma is the most common form, affecting approximately 3.6 million people in the United States.
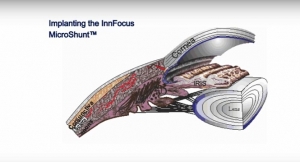
The iStent was approved by the U.S. Food & Drug Administration (FDA) in June 2012 and is indicated for use in conjunction with cataract surgery for the reduction of IOP in adult patients with mild-to-moderate open-angle glaucoma currently treated with ocular hypotensive medication. The iStent is inserted through the trabecular meshwork and into Schlemm’s canal, the eye’s drainage system, where it restores the natural, physiological outflow of aqueous humor. Made of surgical-grade non-ferromagnetic titanium that is coated with heparin, the iStent is approximately 1.0 mm long and 0.33 mm wide. Glaukos believes it is the smallest medical device ever approved by the FDA.
The iStent Trabecular Micro-Bypass Stent is indicated for use in conjunction with cataract surgery for the reduction of IOP in adult patients with mild-to-moderate open-angle glaucoma currently treated with ocular hypotensive medication. The iStent is contraindicated in eyes with primary or secondary angle closure glaucoma, including neovascular glaucoma, as well as in patients with retrobulbar tumor, thyroid eye disease, Sturge-Weber Syndrome or any other type of condition that may cause elevated episcleral venous pressure.
The most common post-operative adverse events reported in the randomized pivotal trial included early post-operative corneal edema (8 percent), BCVA loss of ≥ 1 line at or after the three-month visit (7 percent), posterior capsular opacification (6 percent), stent obstruction (4 percent) early post-operative anterior chamber cells (3 percent), and early post-operative corneal abrasion (3 percent).
Glaukos pioneered micro-invasive glaucoma surgery, or MIGS, to revolutionize the traditional glaucoma treatment and management paradigm. Glaukos launched the iStent, its first MIGS device, in the United States in July 2012 and is leveraging its platform technology to build a comprehensive and proprietary portfolio of micro-scale injectable therapies designed to address the complete range of glaucoma disease states and progression. The company believes the iStent, measuring 1.0 mm long and 0.33 mm wide, is the smallest medical device ever approved by the FDA.
The retrospective, consecutive case series includes 168 eyes of 128 patients who underwent iStent implantation with concomitant cataract surgery, of which 134 eyes in 100 patients have been followed through one year. Study researchers reported that 87 percent of subjects had moderate to severe OAG and 80 percent were Hispanic, a population segment with a higher-than-average incidence and prevalence of OAG. Up to 21 percent of Hispanics are expected to develop OAG by age 80, according to a reference cited in the study.
All procedures in the series were performed by Mark J. Gallardo, M.D., at a single site in El Paso, Texas. Before surgery, patients were placed into three subgroups in accordance with the surgeon’s typical clinical practice and based on the patient’s IOP level, medication burden and treatment goal. In the 134 eyes with one-year postoperative follow-up, the safety profile was favorable and treatment success was achieved in all three subgroups as follows:
Group 1: Comprised of 65 eyes with controlled IOP on at least one ocular hypotensive medication preoperatively and a treatment goal to reduce medication burden while maintaining IOP control. One year following the procedure, medication burden decreased from a mean of 2.4 medications preoperatively to 0.6 at one year; this decrease was statistically significant (p<0.001). Further, mean IOP decreased to 12.7 mm Hg, compared to 13.6 mm Hg preoperatively.
Group 2: Comprised of 31 eyes with IOP not controlled on up to two ocular hypotensive medications preoperatively and a treatment goal to reduce IOP and maintain or reduce medication burden. One year following the procedure, all eyes had IOP of 18 mm Hg or lower with a statistically significant (p<0.001) reduction to a mean IOP of 12.6 mm Hg, compared to 19.1 mm Hg preoperatively. Medication burden decreased to a mean of 0.4 medications, compared to 1.1 preoperatively.
Group 3: Comprised of 40 eyes on three or more ocular hypotensive medications and/or uncontrolled IOP preoperatively with a treatment goal to reduce IOP in order to avoid filtering surgery. One year following the procedure, 95 percent (38 of 40 eyes) achieved their treatment goal. In these 38 eyes, mean IOP decreased to 13.6 mm Hg, compared to 19.3 mm Hg preoperatively, which was statistically significant (p< 0.001). Medication burden decreased to a mean of 1.8 medications, compared to 3.2 preoperatively.
“These data show that iStent in combination with cataract surgery can effectively reduce IOP and topical ocular hypotensive medication use in a mainly Hispanic patient population, including those with more advanced disease,” said Gallardo. “Importantly, these results were achieved in a real-life clinical setting, where the treatment goals differ by patient, based on their individual needs and disease state. The study’s high success rate overall and within each patient subgroup underscores the tangible benefits of using trabecular bypass stenting to manage IOP and medication burden in a demographically diverse glaucoma patient population.”
Typically associated with elevated IOP, glaucoma is characterized by progressive, irreversible and largely asymptomatic vision loss caused by optic nerve damage. It is a leading cause of blindness. According to Market Scope, more than 80 million people worldwide have glaucoma, including 4.5 million people in the United States. Open-angle glaucoma is the most common form, affecting approximately 3.6 million people in the United States.
The iStent was approved by the U.S. Food & Drug Administration (FDA) in June 2012 and is indicated for use in conjunction with cataract surgery for the reduction of IOP in adult patients with mild-to-moderate open-angle glaucoma currently treated with ocular hypotensive medication. The iStent is inserted through the trabecular meshwork and into Schlemm’s canal, the eye’s drainage system, where it restores the natural, physiological outflow of aqueous humor. Made of surgical-grade non-ferromagnetic titanium that is coated with heparin, the iStent is approximately 1.0 mm long and 0.33 mm wide. Glaukos believes it is the smallest medical device ever approved by the FDA.
The iStent Trabecular Micro-Bypass Stent is indicated for use in conjunction with cataract surgery for the reduction of IOP in adult patients with mild-to-moderate open-angle glaucoma currently treated with ocular hypotensive medication. The iStent is contraindicated in eyes with primary or secondary angle closure glaucoma, including neovascular glaucoma, as well as in patients with retrobulbar tumor, thyroid eye disease, Sturge-Weber Syndrome or any other type of condition that may cause elevated episcleral venous pressure.
The most common post-operative adverse events reported in the randomized pivotal trial included early post-operative corneal edema (8 percent), BCVA loss of ≥ 1 line at or after the three-month visit (7 percent), posterior capsular opacification (6 percent), stent obstruction (4 percent) early post-operative anterior chamber cells (3 percent), and early post-operative corneal abrasion (3 percent).
Glaukos pioneered micro-invasive glaucoma surgery, or MIGS, to revolutionize the traditional glaucoma treatment and management paradigm. Glaukos launched the iStent, its first MIGS device, in the United States in July 2012 and is leveraging its platform technology to build a comprehensive and proprietary portfolio of micro-scale injectable therapies designed to address the complete range of glaucoma disease states and progression. The company believes the iStent, measuring 1.0 mm long and 0.33 mm wide, is the smallest medical device ever approved by the FDA.