01.08.14
Palo Alto, Calif.-based SinuSys Corporation, a sinus health company, has earned 510(k) clearance from the U.S. Food and Drug Administration (FDA) for its Vent-Os sinus dilation system. The device is designed to resolve sinusitis symptoms in a two-step interventional procedure. According to the company, Vent-Os enables low-pressure, gradual dilation of the maxillary sinus ostia, which is intended to maximize patient tolerability of the procedure in an office setting under local anesthesia. SinuSys plans to commercialize the device immediately in select markets in the United States.
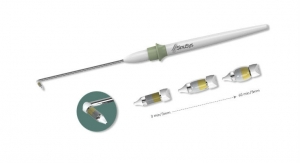
Unlike balloon dilation devices that use rapid, high-pressure inflation, Vent-Os is a small, low-pressure, self-expanding insert designed to gently and gradually open the maxillary ostia. The Vent-Os system incorporates the SinuSys’ proprietary osmotic technology, which uses the body’s natural mucosal fluids to expand the insert before removal. In an office setting, patients can be comfortably relocated to the waiting room between insertion and removal of the device.
The Vent-Os system achieved post-procedural patency in 95 percent of the sinus ostia treated in a multi-center study and submitted as part of the company’s FDA application; five percent of the treated ostia could not be visualized. In the study, the Vent-Os device was inserted into the maxillary sinus opening at the beginning of the procedure and removed after 60 minutes. No adverse events occurred during insertion or removal of the device. Three-month follow-up was completed in 33 patients (55 ostia), with 93 percent of the treated ostia remaining patent and seven percent that could not be visualized. No ostia were reported to be occluded.
Fifteen percent of patients in the study were treated in an office setting after pre-procedural injection of anesthesia; no additional anesthesia or medication was required for these patients for the duration of the procedure. This is in contrast to balloon dilation devices, which often require administration of anxiolytics, analgesics and/or additional local injections of anesthetics during the procedure to increase patient tolerability. The remaining patients were treated in the operating room adjunctive to functional endoscopic sinus surgery.
“In my opinion, the SinuSys team has demonstrated that gradual, low pressure can dilate the maxillary sinus ostium,” said Peter Catalano, M.D., FACS, professor of otolaryngology at Tufts University, chief of otolaryngology at St. Elizabeth’s Medical Center in Boston and an investigator in the Vent-Os study. “The Vent-Os system is very easy to deploy and is exceptionally well-tolerated by patients under local anesthesia. SinuSys’ unique osmotic expansion technology appears to be an ideal intervention for patients requiring ventilation and drainage of the maxillary sinus, especially for procedures to be performed in an office setting.”
“With the Vent-Os System, it was our intent to design a device that solved the current clinical challenges with treating sinus disease in a way that was easy for both physicians and their patients,” said SinuSys’ CEO Tom Schreck added. “Our maxillary sinus device is showing initial clinical success and we look forward to developing the same simple, gentle technology for use in other sinus anatomy.”
The FDA cleared the Vent-Os Sinus Dilation System for dilation of the maxillary sinus ostia and associated spaces in adults for diagnostic and therapeutic procedures. The Vent-Os System has also received the CE mark (European Union), Health Canada license and Australian Therapeutic Goods Administration certificate, and is currently being commercialized in those regions.
Chronic sinusitis affects more than 31 million people in the United States. It is more prevalent than heart disease and asthma, and has a greater impact on patients’ quality of life than chronic back pain or congestive heart failure. The majority of patients with chronic sinusitis are treated with oral antibiotics and/or nasal steroids, which can increase the risk of antibiotic resistance and cause unwanted side effects such as epistaxis (nose bleeds), nasal ulcers, and nasal and oral infections. The most effective surgical treatment is Functional Endoscopic Sinus Surgery (FESS), which is conducted in a surgical suite under general anesthesia or IV sedation. The United States healthcare system currently spends more than $8 billion annually on improving the health of patients with sinus conditions.
Unlike balloon dilation devices that use rapid, high-pressure inflation, Vent-Os is a small, low-pressure, self-expanding insert designed to gently and gradually open the maxillary ostia. The Vent-Os system incorporates the SinuSys’ proprietary osmotic technology, which uses the body’s natural mucosal fluids to expand the insert before removal. In an office setting, patients can be comfortably relocated to the waiting room between insertion and removal of the device.
The Vent-Os system achieved post-procedural patency in 95 percent of the sinus ostia treated in a multi-center study and submitted as part of the company’s FDA application; five percent of the treated ostia could not be visualized. In the study, the Vent-Os device was inserted into the maxillary sinus opening at the beginning of the procedure and removed after 60 minutes. No adverse events occurred during insertion or removal of the device. Three-month follow-up was completed in 33 patients (55 ostia), with 93 percent of the treated ostia remaining patent and seven percent that could not be visualized. No ostia were reported to be occluded.
Fifteen percent of patients in the study were treated in an office setting after pre-procedural injection of anesthesia; no additional anesthesia or medication was required for these patients for the duration of the procedure. This is in contrast to balloon dilation devices, which often require administration of anxiolytics, analgesics and/or additional local injections of anesthetics during the procedure to increase patient tolerability. The remaining patients were treated in the operating room adjunctive to functional endoscopic sinus surgery.
“In my opinion, the SinuSys team has demonstrated that gradual, low pressure can dilate the maxillary sinus ostium,” said Peter Catalano, M.D., FACS, professor of otolaryngology at Tufts University, chief of otolaryngology at St. Elizabeth’s Medical Center in Boston and an investigator in the Vent-Os study. “The Vent-Os system is very easy to deploy and is exceptionally well-tolerated by patients under local anesthesia. SinuSys’ unique osmotic expansion technology appears to be an ideal intervention for patients requiring ventilation and drainage of the maxillary sinus, especially for procedures to be performed in an office setting.”
“With the Vent-Os System, it was our intent to design a device that solved the current clinical challenges with treating sinus disease in a way that was easy for both physicians and their patients,” said SinuSys’ CEO Tom Schreck added. “Our maxillary sinus device is showing initial clinical success and we look forward to developing the same simple, gentle technology for use in other sinus anatomy.”
The FDA cleared the Vent-Os Sinus Dilation System for dilation of the maxillary sinus ostia and associated spaces in adults for diagnostic and therapeutic procedures. The Vent-Os System has also received the CE mark (European Union), Health Canada license and Australian Therapeutic Goods Administration certificate, and is currently being commercialized in those regions.
Chronic sinusitis affects more than 31 million people in the United States. It is more prevalent than heart disease and asthma, and has a greater impact on patients’ quality of life than chronic back pain or congestive heart failure. The majority of patients with chronic sinusitis are treated with oral antibiotics and/or nasal steroids, which can increase the risk of antibiotic resistance and cause unwanted side effects such as epistaxis (nose bleeds), nasal ulcers, and nasal and oral infections. The most effective surgical treatment is Functional Endoscopic Sinus Surgery (FESS), which is conducted in a surgical suite under general anesthesia or IV sedation. The United States healthcare system currently spends more than $8 billion annually on improving the health of patients with sinus conditions.