Mark Crawford, Contributing Writer06.06.17
Packaging and sterilizing medical devices today is not much different than it was 20 to 30 years ago. Most devices are still sterilized using ethylene oxide sterilization (EtO), steam, or gamma radiation, with standard Tyvek or foil pouch packaging.
However, these “legacy” sterilization methods are not as effective with newer, more complex products, especially those with advanced materials or biologics. Longer lead times for the packaging development requirements for these devices must also be considered; new packaging formats or materials typically require extensive validation testing, which must be factored into the launch timeline.
Many medical device manufacturers (MDMs) are reluctant to embrace new methods of sterilization and packaging unless a strong business case exists for working outside of tried-and-tested solutions. And, even though they know it is ultimately in their best interests to move forward with new technologies, some still try to make the old ones work—mostly to save money and hasten speed to market.
This approach, however, can easily backfire.
“Medical device manufacturers are trying to make legacy packaging methods work for advanced products that have newer materials and designs, and then discover they don’t,” said Kyle Gilles, sterilization microbiology manager for REVOX Sterilization Solutions, a Plymouth, Minn.-based provider of room-temperature vaporized peracetic acid (VPA) sterilization for the medical device industry.
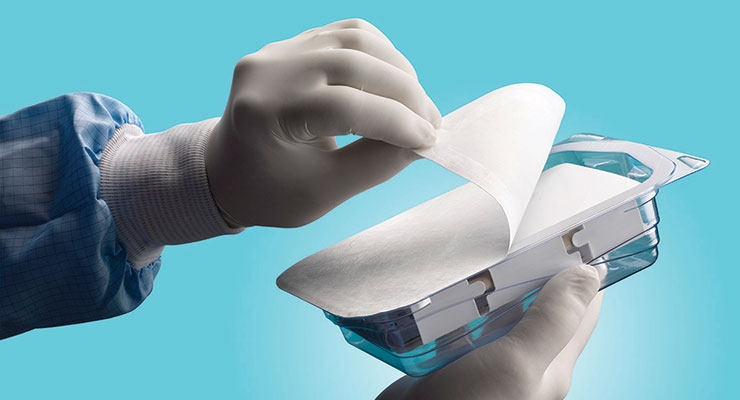
Seal integrity is a top packaging concern and becomes more challenging as products continue to rapidly evolve. Once a package is sealed, it must remain intact post-sterilization to the point of use. Careful design is critical to ensure the packaging protects the device and maintains the sterile barrier.
“Improper packaging design can result in weak seal flanges and a greater risk of the product moving and creating a void in the seal or perforating the barrier, whether it is the tray/lid combination or pouch,” said Seán Egan, director of global marketing for Nelipak Healthcare Packaging, a Cranston, R.I.-based provider of custom thermoformed packaging solutions for the healthcare industry.
A recall of a defective product can have huge negative impacts on an MDM—not only by possibly harming patients, but also damaging the brand, eroding market share, and losing the confidence of the end user. Sometimes a poor packaging decision results from a lack of insight or experience. For example, young companies and startups, which typically lack experience and capital, tend to discount the importance of packaging as a critical functioning component of their devices. Their packaging strategy might simply be to drop the device into a Tyvek/poly pouch without taking into account simulated distribution testing outcomes and potential degradation to the product.
Other poor packaging decisions are an attempt to reduce cost. Manufacturers take a big risk when they buy off-the-shelf pouches and then try to manipulate their devices to fit into the pouches.
“In cases where the pouch is too large, the manufacturer is folding the pouches, creating possible breaches in the sterile barrier system,” said Wendy Mach, packaging section leader for Nelson Laboratories, a Salt Lake City, Utah-based subsidiary of Sterigenics International that provides microbiological testing for medical technology companies. “Also, when a pouch is too large, the seal may not contain the device appropriately.”
“It is ironic that so much R&D can be spent on designing and building a device, with little thought toward packaging,” added John Walter, director of new business development for Command Medical Products, an Ormond Beach, Fla.-based contract manufacturing organization that provides subassemblies and finished devices for the medical device industry. “As the contract manufacturer, we have to respect the customer’s requirements. However, during the initial product runs, we share our concerns and provide options for the customer to consider, before building a product that has a risk of packaging failure.”
What OEMs Want
OEMs seek sterilization and packaging vendors that can be long-term strategic partners and problem-solvers. They expect these vendors to reduce overall cost and time to market by providing proof-of-concepts for proposed solutions that boost the success rate for their products. Because time to market is critical, a responsive partner that accelerates product development planning, feasibility testing, and management through validation is an extremely valuable asset. OEMs are intent on consolidating their top vendors into shorter supply chains to maximize efficiency, reduce costs, and share risk.
MDMs also want flexible sterilization technologies that meet their changing product needs, whether it is a complex geometry in a drug-delivery device, a device material issue, or a combination product with pressure and temperature sensitivities. The “one size fits all cycles” approach of large contract sterilization providers is not always the best choice, especially for more complex products. Also, more small- to medium-sized MDMs are recognizing the operational inefficiencies associated with outsourcing sterilization, such as long turnaround times and tied-up inventory.
“Manufacturers don’t like to see their projects delayed because of long queues or slow validation processes of the larger contract sterilization providers,” said Gilles. “If the product to be validated isn’t a blockbuster, or if the manufacturer isn’t a top-tier contract sterilization customer, validations can take months.”
To counter these delays, some MDMs are bringing sterilization in-house (especially for sensitive products) where modular, low-temperature sterilization units (for example, nitrogen or hydrogen peroxide) can be set up, requiring little space and infrastructure.
Latest Trends
Sustainability in packaging is a top requirement for many manufacturing companies, across a wide range of industries. “Packaging materials are extremely visible to the consumer,” stated Smithers Pira, a UK-based packaging consulting firm. “There are intense and growing pressures from consumers, retailers, packaged product suppliers, governments, regulators, non-government organizations, and environmental groups for the development of environmentally friendly or green materials, packaging designs, and end-of-life processes to improve packaging sustainability by reducing its societal and environmental impacts.”1
This trend is gaining traction in the medical device space. Sustainability is a growing focus for convertors, OEMs, and end users across the healthcare industry. Waste reduction through efficient design reduces material usage and requires less energy to manufacture product; the reduced footprint decreases sterilization and transportation costs through higher loading factors. Some companies are considering biodegradable packaging as their next step toward greener manufacturing.
Demand for increased functionality in medical devices requires improved packaging that is easier to use in the operating room or emergency room, where it helps reduce risk and delays by presenting the components in the order they are needed for the procedure—in some cases, the packaging can actually assist the preparation of the device before it is presented to the patient. Advanced packaging designs can also better protect medical devices that may have been compromised by sterilization methods such as EtO. “For example,” said Egan, “a catheter set that has relaxed during the sterilization process may lose its shape. A redesigned tray can eliminate that risk by keeping the components in their correct form during sterilization with knurling features that ensure efficient flow of the gas during the cycle to fully sterilize the device.”
OEMs are also very eager to reduce costs through various operational adjustments, such as reduced sample sizes, which shortens time to market. The standards simply suggest that companies “justify a statistically valid rationale” for the sample size; without more guidance, determining an adequate sample size can be a challenge for MDMs.
“Many of these companies do not have enough trained individuals who can manage this aspect of the validation protocols, or fully understand how the validations work, and how to run them,” said Mach. “This calls into question the appropriateness of the quantity used for testing when being reviewed by regulatory agencies, which then delays getting products to market—something these companies are not prepared for.”
Low-Temperature Sterilization Options
Most medical devices are still sterilized using EtO, steam, and gamma radiation. These are tried-and-true methods that every MDM is comfortable with. However, newer materials and drug-device combination products (many of which are temperature- or pressure-sensitive) provide more challenges to legacy sterilization and packaging technologies.
“Many of these biologics/combination products do not lend themselves well to traditional sterilization methods,” said Maura O. Kahn, vice president of business development and marketing for Noxilizer Inc., a Baltimore, Md.-based provider of room-temperature nitrogen dioxide sterilization and decontamination equipment. “Additionally, complex device designs often require sterilization processes that offer the ability to adjust vacuum and navigate into tortuous paths. True gas technologies may present an advantage in these situations.”
“New products and materials such as moisture- and temperature-sensitive products with bioabsorbable or drug-coated materials, electronics, and wet-tissue products don’t do well with elevated temperature/humidity sterilization methods,” added Gilles. “On one end of the spectrum is the need to simplify product packaging, such as for prefilled syringes where higher temperature sterilization can often impact the active pharmaceutical ingredient; on the other end are highly complex products with various materials that may require different legacy methods for each component material.”
A growing number of biopharmaceuticals, novel medical device materials, and increasingly complex drug-delivery devices also need to be sterilized after being placed in the sterile barrier packaging. This is usually because they are administered in the sterile field or a needle path comes into contact with the drug and/or patient.
An alternative method to standard sterilization technologies is nitrogen dioxide (NO2), an ultra-low-temperature sterilization (10 degrees to 30 degrees Celsius) process that helps maintain drug integrity. NO2 is not carcinogenic, mutagenic, or explosive. Other advantages are its minimal vacuum cycle and effectiveness as a surface sterilant (no cytotoxic residuals). NO2 sterilization equipment only requires a power source and a venting system; therefore, structurally reinforced doors and walls are not required. “As a result, NO2 sterilization can be done at the contract manufacturer, which saves considerable time, shortens the supply chain, and generates incremental revenue,” said Kahn.
Other low-temperature sterilization methods gaining attention include gas plasma and vaporized hydrogen peroxide (VHP).
“Vaporized hydrogen peroxide can be used to surface sterilize any type of material,” stated James Dwyer, vice president of operations for Millstone Medical, a Fall River, Mass.-based provider of post-manufacturing services, including inspection, sterile and non-sterile packaging, and finished goods distribution. “It is a relatively new technology that is gaining in popularity because it is low temperature and safe for humidity- or radiation-sensitive drug products. However, this technology is better suited for in-house sterilization because the current equipment does not support higher volumes.”
Another low-temperature method is VPA, a newer technology that utilizes an established chemical process with a long history of safety and efficacy. “Cantel has been manufacturing liquid peracetic acid for use as a sterilant and high-level disinfectant for over 40 years,” said Gilles. “We discovered it also has great sterilization capabilities in a room-temperature, vaporized state. Its safety profile is strong from both environmental and residual standpoints, and it can be used onsite with few environmental, health, and safety concerns or capital buildout. It is also scalable, as we have shown with our new two-pallet (3,000 L) chamber. Therefore, the sterilization process can now be an integral part of a lean manufacturing process.”
Despite the advantages of these newer gas technologies, most medical products are not being transitioned to these methods because of capacity limitations. Because they are scalable, however, these low-temperature techniques are ideal for in-house sterilization of small volumes of product. In addition, long-proven legacy sterilization techniques such as radiation are not necessarily out of the running for sterilizing more sensitive products made with novel materials.
“For materials that are not radiation friendly and require lower and tighter dose ranges, we have found that fractional dosing, combined with temperature-controlled processing, can overcome some of these sensitivity issues,” said Larry Nichols, CEO for Steri-Tek, a Fremont, Calif.-based provider of high-volume, e-beam/x-ray contract sterilization for the medical device, biotech, and pharmaceutical industries.
Steri-Tek used its in-house knowledge to develop a proprietary radiation system specifically for radiation-sensitive materials such as drugs/biologics, combination devices, bioabsorbables, implantables, advanced polymers, and other complex products. Products containing electronics do not work well with radiation and are better suited for low-temperature gas methods.
MDMs can also make material adjustments in their products if they want to stay with a mainstream process like radiation. For example, irradiating products made from fluorocarbon materials can sometimes result in material degradation; polytetrafluoroethylene (PTFE) will break down and actually turn to powder with a high-enough radiation dose. Under many sterilization doses, PTFE will flake off. Therefore most MDMs choose EtO to sterilize these products. “However, when companies plan ahead, they can usually find other materials that can replace the fluorocarbons in the device and still maintain the lubricity that is required,” said Nichols. “This then gives them the option to sterilize with either EtO or radiation.”
Other Tools of the Trade
Packagers focus on using the best combination of existing sterilization and packaging technologies to implement quick and effective solutions for their customers. One way to do this is through simulation technology. Nelipak, for example, shows customers at the concept design stage predicted material distributions for rigid packaging in order to determine the best design/packaging combination, before starting prototype development.
“Package simulation gives our customers data on the package integrity during transportation testing to identify potential issues that may result in product damage and/or seal integrity breach caused by transport and handling,” said Egan. “This greatly reduces lead time by increasing the success rate of the design, before going through the costly and time-consuming physical process.”
Another way to improve packaging and sterilization is through the use of porous coatings. These coatings are required to marry a top-web (coated Tyvek) to a bottom web (film). The more porous the coating, the shorter the sterilization time. For example, Oliver Healthcare Packaging, a Grand Rapids, Mich.-based supplier of pouches, lidding, roll stock, and mounting cards for the healthcare industry, offers several different coating technologies. The Xhale coating is about 2.7 times more porous than other coating processes on the market. This shortens the total sterilization time (driven in part by less time spent in aeration), which reduces cost.
“Furthermore, customers that use autoclave sterilization modalities can also benefit from these coatings, which can withstand these rigorous sterilization cycles and still maintain quality and seal integrity,” said Aldin Velic, director of global marketing for Oliver Healthcare Packaging.
For products (dissolvable sutures, bone cement, or devices with drug coatings) that require high-barrier, moisture, and UV protective porous packaging materials, Oliver developed the Dispos-a-vent pouch, which also works for autoclave or EtO sterilization. With traditional sterilization, a device is packaged in two separate packages: one to meet the high-barrier need and the second to address sterilization. “This requires customers to validate two packages and have two separate packing processes, which adds significant cost to the overall process,” said Velic. “The Dispos-a-vent product circumvents all these additional steps by offering a complete package that lowers total landed cost, works with various sterilization modalities, and provides customers with the high-barrier protection their devices need.”
Noxilizer and two partners (Getinge and Dara Pharma) have collaborated to develop a nitrogen dioxide solution for low-speed filling lines, which are becoming increasingly important as more new biologics are developed. (Since these drugs are for smaller patient populations, they do not require the high-speed filling lines used for vaccines and insulin.) The companies launched the Moduline-BioDecontamination unit in 2016. This device uses NO2 to deliver a rapid total process time, including decontamination under the syringe tub lip (an often-overlooked source of potential contamination) and aeration to ppb residual sterilant levels within minutes, reducing risk for biologic products. “The system is designed to meet the needs of low-speed filling lines—one tub per minute, or 20 tubs in 20 minutes,” said Kahn. “The efficacy is comparable to e-beam at a much lower cost.”
Regulatory Challenges
The U.S. Food and Drug Administration (FDA) continues to focus on OEM supply chain relationships to ensure suppliers are fully integrated into OEM processes, especially quality assurance.
“The FDA is concerned about the last leg of the supply chain—how much the sterile barrier gets handled inside hospitals,” said Dwyer. “They want to know if OEMs are focused enough on what the product must withstand before point of use.”
The FDA is also concerned about particulates inside packages that can trigger a recall due to manufacturing issues; as a result, more emphasis is being placed on good manufacturing practices and manufacturing in ISO-classified cleanrooms. The FDA also wants to see more endotoxin testing of medical devices to learn more about the possible role packaging plays in contributing endotoxins that contaminate the devices at point of use. “Water-based processes in the manufacturing of packaging materials may contribute to endotoxins, something that also needs to be considered when evaluating suppliers,” added Dwyer.
Uncertainty about how the FDA will regulate newer technologies continues. The latest FDA guidance document, published in March 2016, acknowledges newer technologies such as VPA and VHP; however, until they have their own specific ISO standards (among other criteria), they are classified as “novel.”
“This term concerns some prospects, but as they see devices submitted and 510(k)-cleared using VPA or other methods, they come to understand that when ISO 14937 standards are followed, and the data packet is complete, VPA is as acceptable as any other sterilization method from a regulatory standpoint,” said Gilles.
REVOX encourages clients to request pre-submission meetings with the FDA or notified body early in the process to address any concerns about VPA. “It’s only a matter of following published standards and providing the same data you’d need to provide with any other sterilization method,” said Gilles. “It’s understandable that no project team wants to be the guinea pig with something new, but as more approvals come through, the upsides of a better process will outweigh the perceived risks.”
A growing concern among MDMs is the classification of EtO as a carcinogen. The U.S. Environmental Protection Agency, after completing a study on EtO exposure and cancer, concluded that EtO can be carcinogenic to humans through the inhalation route of exposure. Europe is moving to reduce the use of EtO as a sterilant and more U.S. hospitals are wary of the risks associated with in-house EtO sterilization.
“Although all sterilization methods have their strengths and weaknesses,” said Kahn, “the healthcare concerns regarding EtO are growing. OEMs are beginning to investigate other sterilization methods that could reduce the use of EtO.”
Moving Forward
Packaging and sterilization are absolutely critical for a successful product launch, as well as protecting the final product (and all the money invested in making it). It does not matter how well-designed or innovative a product is; if it arrives in a compromised condition, it is a failure and perhaps even a costly liability. Product design, packaging, and sterilization must be considered together to achieve an on-time launch; any packaging or sterilization problems resulting from poor planning could delay the launch, losing valuable market share.
This leaves little room for mistakes. “Recall” can be a terrifying word—not just because of the high expense of undertaking and fixing a recall, but also compromised patient safety, inconvenience and delay for the end user, and damage done to brand and market reputation.
This is why sterilization and packaging is critical for protecting the product lifecycle. However, “packaging is often left as the last aspect of the design process and given the shortest amount of time and resources to complete,” said Mach. “This puts significant pressure on the packaging teams and testing because no one prepares for failures as a result of poor planning. We always suggest that manufacturers develop prototype packaging and perform preliminary tests in the beginning to prevent these types of issues when time/money and product become critical.”
Dwyer indicated that delays of up to 12 months can occur if packaging design and validation are not given enough focus early in product development initiatives.
“There is a delicate balance between taking time to ensure the quality and package design of your product and increasing your time to market,” he said. “Failure to dedicate the appropriate time and resources during the initial stages of product design can create significant setbacks during validations. Robust design helps prevent failures during validation, and while the product is in the field.”
References
Mark Crawford is a full-time freelance business and marketing/communications writer based in Madison, Wis. His clients range from startups to global manufacturing leaders. He also writes a variety of feature articles for regional and national publications and is the author of five books.
However, these “legacy” sterilization methods are not as effective with newer, more complex products, especially those with advanced materials or biologics. Longer lead times for the packaging development requirements for these devices must also be considered; new packaging formats or materials typically require extensive validation testing, which must be factored into the launch timeline.
Many medical device manufacturers (MDMs) are reluctant to embrace new methods of sterilization and packaging unless a strong business case exists for working outside of tried-and-tested solutions. And, even though they know it is ultimately in their best interests to move forward with new technologies, some still try to make the old ones work—mostly to save money and hasten speed to market.
This approach, however, can easily backfire.
“Medical device manufacturers are trying to make legacy packaging methods work for advanced products that have newer materials and designs, and then discover they don’t,” said Kyle Gilles, sterilization microbiology manager for REVOX Sterilization Solutions, a Plymouth, Minn.-based provider of room-temperature vaporized peracetic acid (VPA) sterilization for the medical device industry.
Seal integrity is a top packaging concern and becomes more challenging as products continue to rapidly evolve. Once a package is sealed, it must remain intact post-sterilization to the point of use. Careful design is critical to ensure the packaging protects the device and maintains the sterile barrier.
“Improper packaging design can result in weak seal flanges and a greater risk of the product moving and creating a void in the seal or perforating the barrier, whether it is the tray/lid combination or pouch,” said Seán Egan, director of global marketing for Nelipak Healthcare Packaging, a Cranston, R.I.-based provider of custom thermoformed packaging solutions for the healthcare industry.
A recall of a defective product can have huge negative impacts on an MDM—not only by possibly harming patients, but also damaging the brand, eroding market share, and losing the confidence of the end user. Sometimes a poor packaging decision results from a lack of insight or experience. For example, young companies and startups, which typically lack experience and capital, tend to discount the importance of packaging as a critical functioning component of their devices. Their packaging strategy might simply be to drop the device into a Tyvek/poly pouch without taking into account simulated distribution testing outcomes and potential degradation to the product.
Other poor packaging decisions are an attempt to reduce cost. Manufacturers take a big risk when they buy off-the-shelf pouches and then try to manipulate their devices to fit into the pouches.
“In cases where the pouch is too large, the manufacturer is folding the pouches, creating possible breaches in the sterile barrier system,” said Wendy Mach, packaging section leader for Nelson Laboratories, a Salt Lake City, Utah-based subsidiary of Sterigenics International that provides microbiological testing for medical technology companies. “Also, when a pouch is too large, the seal may not contain the device appropriately.”
“It is ironic that so much R&D can be spent on designing and building a device, with little thought toward packaging,” added John Walter, director of new business development for Command Medical Products, an Ormond Beach, Fla.-based contract manufacturing organization that provides subassemblies and finished devices for the medical device industry. “As the contract manufacturer, we have to respect the customer’s requirements. However, during the initial product runs, we share our concerns and provide options for the customer to consider, before building a product that has a risk of packaging failure.”
What OEMs Want
OEMs seek sterilization and packaging vendors that can be long-term strategic partners and problem-solvers. They expect these vendors to reduce overall cost and time to market by providing proof-of-concepts for proposed solutions that boost the success rate for their products. Because time to market is critical, a responsive partner that accelerates product development planning, feasibility testing, and management through validation is an extremely valuable asset. OEMs are intent on consolidating their top vendors into shorter supply chains to maximize efficiency, reduce costs, and share risk.
MDMs also want flexible sterilization technologies that meet their changing product needs, whether it is a complex geometry in a drug-delivery device, a device material issue, or a combination product with pressure and temperature sensitivities. The “one size fits all cycles” approach of large contract sterilization providers is not always the best choice, especially for more complex products. Also, more small- to medium-sized MDMs are recognizing the operational inefficiencies associated with outsourcing sterilization, such as long turnaround times and tied-up inventory.
“Manufacturers don’t like to see their projects delayed because of long queues or slow validation processes of the larger contract sterilization providers,” said Gilles. “If the product to be validated isn’t a blockbuster, or if the manufacturer isn’t a top-tier contract sterilization customer, validations can take months.”
To counter these delays, some MDMs are bringing sterilization in-house (especially for sensitive products) where modular, low-temperature sterilization units (for example, nitrogen or hydrogen peroxide) can be set up, requiring little space and infrastructure.
Latest Trends
Sustainability in packaging is a top requirement for many manufacturing companies, across a wide range of industries. “Packaging materials are extremely visible to the consumer,” stated Smithers Pira, a UK-based packaging consulting firm. “There are intense and growing pressures from consumers, retailers, packaged product suppliers, governments, regulators, non-government organizations, and environmental groups for the development of environmentally friendly or green materials, packaging designs, and end-of-life processes to improve packaging sustainability by reducing its societal and environmental impacts.”1
This trend is gaining traction in the medical device space. Sustainability is a growing focus for convertors, OEMs, and end users across the healthcare industry. Waste reduction through efficient design reduces material usage and requires less energy to manufacture product; the reduced footprint decreases sterilization and transportation costs through higher loading factors. Some companies are considering biodegradable packaging as their next step toward greener manufacturing.
Demand for increased functionality in medical devices requires improved packaging that is easier to use in the operating room or emergency room, where it helps reduce risk and delays by presenting the components in the order they are needed for the procedure—in some cases, the packaging can actually assist the preparation of the device before it is presented to the patient. Advanced packaging designs can also better protect medical devices that may have been compromised by sterilization methods such as EtO. “For example,” said Egan, “a catheter set that has relaxed during the sterilization process may lose its shape. A redesigned tray can eliminate that risk by keeping the components in their correct form during sterilization with knurling features that ensure efficient flow of the gas during the cycle to fully sterilize the device.”
OEMs are also very eager to reduce costs through various operational adjustments, such as reduced sample sizes, which shortens time to market. The standards simply suggest that companies “justify a statistically valid rationale” for the sample size; without more guidance, determining an adequate sample size can be a challenge for MDMs.
“Many of these companies do not have enough trained individuals who can manage this aspect of the validation protocols, or fully understand how the validations work, and how to run them,” said Mach. “This calls into question the appropriateness of the quantity used for testing when being reviewed by regulatory agencies, which then delays getting products to market—something these companies are not prepared for.”
Low-Temperature Sterilization Options
Most medical devices are still sterilized using EtO, steam, and gamma radiation. These are tried-and-true methods that every MDM is comfortable with. However, newer materials and drug-device combination products (many of which are temperature- or pressure-sensitive) provide more challenges to legacy sterilization and packaging technologies.
“Many of these biologics/combination products do not lend themselves well to traditional sterilization methods,” said Maura O. Kahn, vice president of business development and marketing for Noxilizer Inc., a Baltimore, Md.-based provider of room-temperature nitrogen dioxide sterilization and decontamination equipment. “Additionally, complex device designs often require sterilization processes that offer the ability to adjust vacuum and navigate into tortuous paths. True gas technologies may present an advantage in these situations.”
“New products and materials such as moisture- and temperature-sensitive products with bioabsorbable or drug-coated materials, electronics, and wet-tissue products don’t do well with elevated temperature/humidity sterilization methods,” added Gilles. “On one end of the spectrum is the need to simplify product packaging, such as for prefilled syringes where higher temperature sterilization can often impact the active pharmaceutical ingredient; on the other end are highly complex products with various materials that may require different legacy methods for each component material.”
A growing number of biopharmaceuticals, novel medical device materials, and increasingly complex drug-delivery devices also need to be sterilized after being placed in the sterile barrier packaging. This is usually because they are administered in the sterile field or a needle path comes into contact with the drug and/or patient.
An alternative method to standard sterilization technologies is nitrogen dioxide (NO2), an ultra-low-temperature sterilization (10 degrees to 30 degrees Celsius) process that helps maintain drug integrity. NO2 is not carcinogenic, mutagenic, or explosive. Other advantages are its minimal vacuum cycle and effectiveness as a surface sterilant (no cytotoxic residuals). NO2 sterilization equipment only requires a power source and a venting system; therefore, structurally reinforced doors and walls are not required. “As a result, NO2 sterilization can be done at the contract manufacturer, which saves considerable time, shortens the supply chain, and generates incremental revenue,” said Kahn.
Other low-temperature sterilization methods gaining attention include gas plasma and vaporized hydrogen peroxide (VHP).
“Vaporized hydrogen peroxide can be used to surface sterilize any type of material,” stated James Dwyer, vice president of operations for Millstone Medical, a Fall River, Mass.-based provider of post-manufacturing services, including inspection, sterile and non-sterile packaging, and finished goods distribution. “It is a relatively new technology that is gaining in popularity because it is low temperature and safe for humidity- or radiation-sensitive drug products. However, this technology is better suited for in-house sterilization because the current equipment does not support higher volumes.”
Another low-temperature method is VPA, a newer technology that utilizes an established chemical process with a long history of safety and efficacy. “Cantel has been manufacturing liquid peracetic acid for use as a sterilant and high-level disinfectant for over 40 years,” said Gilles. “We discovered it also has great sterilization capabilities in a room-temperature, vaporized state. Its safety profile is strong from both environmental and residual standpoints, and it can be used onsite with few environmental, health, and safety concerns or capital buildout. It is also scalable, as we have shown with our new two-pallet (3,000 L) chamber. Therefore, the sterilization process can now be an integral part of a lean manufacturing process.”
Despite the advantages of these newer gas technologies, most medical products are not being transitioned to these methods because of capacity limitations. Because they are scalable, however, these low-temperature techniques are ideal for in-house sterilization of small volumes of product. In addition, long-proven legacy sterilization techniques such as radiation are not necessarily out of the running for sterilizing more sensitive products made with novel materials.
“For materials that are not radiation friendly and require lower and tighter dose ranges, we have found that fractional dosing, combined with temperature-controlled processing, can overcome some of these sensitivity issues,” said Larry Nichols, CEO for Steri-Tek, a Fremont, Calif.-based provider of high-volume, e-beam/x-ray contract sterilization for the medical device, biotech, and pharmaceutical industries.
Steri-Tek used its in-house knowledge to develop a proprietary radiation system specifically for radiation-sensitive materials such as drugs/biologics, combination devices, bioabsorbables, implantables, advanced polymers, and other complex products. Products containing electronics do not work well with radiation and are better suited for low-temperature gas methods.
MDMs can also make material adjustments in their products if they want to stay with a mainstream process like radiation. For example, irradiating products made from fluorocarbon materials can sometimes result in material degradation; polytetrafluoroethylene (PTFE) will break down and actually turn to powder with a high-enough radiation dose. Under many sterilization doses, PTFE will flake off. Therefore most MDMs choose EtO to sterilize these products. “However, when companies plan ahead, they can usually find other materials that can replace the fluorocarbons in the device and still maintain the lubricity that is required,” said Nichols. “This then gives them the option to sterilize with either EtO or radiation.”
Other Tools of the Trade
Packagers focus on using the best combination of existing sterilization and packaging technologies to implement quick and effective solutions for their customers. One way to do this is through simulation technology. Nelipak, for example, shows customers at the concept design stage predicted material distributions for rigid packaging in order to determine the best design/packaging combination, before starting prototype development.
“Package simulation gives our customers data on the package integrity during transportation testing to identify potential issues that may result in product damage and/or seal integrity breach caused by transport and handling,” said Egan. “This greatly reduces lead time by increasing the success rate of the design, before going through the costly and time-consuming physical process.”
Another way to improve packaging and sterilization is through the use of porous coatings. These coatings are required to marry a top-web (coated Tyvek) to a bottom web (film). The more porous the coating, the shorter the sterilization time. For example, Oliver Healthcare Packaging, a Grand Rapids, Mich.-based supplier of pouches, lidding, roll stock, and mounting cards for the healthcare industry, offers several different coating technologies. The Xhale coating is about 2.7 times more porous than other coating processes on the market. This shortens the total sterilization time (driven in part by less time spent in aeration), which reduces cost.
“Furthermore, customers that use autoclave sterilization modalities can also benefit from these coatings, which can withstand these rigorous sterilization cycles and still maintain quality and seal integrity,” said Aldin Velic, director of global marketing for Oliver Healthcare Packaging.
For products (dissolvable sutures, bone cement, or devices with drug coatings) that require high-barrier, moisture, and UV protective porous packaging materials, Oliver developed the Dispos-a-vent pouch, which also works for autoclave or EtO sterilization. With traditional sterilization, a device is packaged in two separate packages: one to meet the high-barrier need and the second to address sterilization. “This requires customers to validate two packages and have two separate packing processes, which adds significant cost to the overall process,” said Velic. “The Dispos-a-vent product circumvents all these additional steps by offering a complete package that lowers total landed cost, works with various sterilization modalities, and provides customers with the high-barrier protection their devices need.”
Noxilizer and two partners (Getinge and Dara Pharma) have collaborated to develop a nitrogen dioxide solution for low-speed filling lines, which are becoming increasingly important as more new biologics are developed. (Since these drugs are for smaller patient populations, they do not require the high-speed filling lines used for vaccines and insulin.) The companies launched the Moduline-BioDecontamination unit in 2016. This device uses NO2 to deliver a rapid total process time, including decontamination under the syringe tub lip (an often-overlooked source of potential contamination) and aeration to ppb residual sterilant levels within minutes, reducing risk for biologic products. “The system is designed to meet the needs of low-speed filling lines—one tub per minute, or 20 tubs in 20 minutes,” said Kahn. “The efficacy is comparable to e-beam at a much lower cost.”
Regulatory Challenges
The U.S. Food and Drug Administration (FDA) continues to focus on OEM supply chain relationships to ensure suppliers are fully integrated into OEM processes, especially quality assurance.
“The FDA is concerned about the last leg of the supply chain—how much the sterile barrier gets handled inside hospitals,” said Dwyer. “They want to know if OEMs are focused enough on what the product must withstand before point of use.”
The FDA is also concerned about particulates inside packages that can trigger a recall due to manufacturing issues; as a result, more emphasis is being placed on good manufacturing practices and manufacturing in ISO-classified cleanrooms. The FDA also wants to see more endotoxin testing of medical devices to learn more about the possible role packaging plays in contributing endotoxins that contaminate the devices at point of use. “Water-based processes in the manufacturing of packaging materials may contribute to endotoxins, something that also needs to be considered when evaluating suppliers,” added Dwyer.
Uncertainty about how the FDA will regulate newer technologies continues. The latest FDA guidance document, published in March 2016, acknowledges newer technologies such as VPA and VHP; however, until they have their own specific ISO standards (among other criteria), they are classified as “novel.”
“This term concerns some prospects, but as they see devices submitted and 510(k)-cleared using VPA or other methods, they come to understand that when ISO 14937 standards are followed, and the data packet is complete, VPA is as acceptable as any other sterilization method from a regulatory standpoint,” said Gilles.
REVOX encourages clients to request pre-submission meetings with the FDA or notified body early in the process to address any concerns about VPA. “It’s only a matter of following published standards and providing the same data you’d need to provide with any other sterilization method,” said Gilles. “It’s understandable that no project team wants to be the guinea pig with something new, but as more approvals come through, the upsides of a better process will outweigh the perceived risks.”
A growing concern among MDMs is the classification of EtO as a carcinogen. The U.S. Environmental Protection Agency, after completing a study on EtO exposure and cancer, concluded that EtO can be carcinogenic to humans through the inhalation route of exposure. Europe is moving to reduce the use of EtO as a sterilant and more U.S. hospitals are wary of the risks associated with in-house EtO sterilization.
“Although all sterilization methods have their strengths and weaknesses,” said Kahn, “the healthcare concerns regarding EtO are growing. OEMs are beginning to investigate other sterilization methods that could reduce the use of EtO.”
Moving Forward
Packaging and sterilization are absolutely critical for a successful product launch, as well as protecting the final product (and all the money invested in making it). It does not matter how well-designed or innovative a product is; if it arrives in a compromised condition, it is a failure and perhaps even a costly liability. Product design, packaging, and sterilization must be considered together to achieve an on-time launch; any packaging or sterilization problems resulting from poor planning could delay the launch, losing valuable market share.
This leaves little room for mistakes. “Recall” can be a terrifying word—not just because of the high expense of undertaking and fixing a recall, but also compromised patient safety, inconvenience and delay for the end user, and damage done to brand and market reputation.
This is why sterilization and packaging is critical for protecting the product lifecycle. However, “packaging is often left as the last aspect of the design process and given the shortest amount of time and resources to complete,” said Mach. “This puts significant pressure on the packaging teams and testing because no one prepares for failures as a result of poor planning. We always suggest that manufacturers develop prototype packaging and perform preliminary tests in the beginning to prevent these types of issues when time/money and product become critical.”
Dwyer indicated that delays of up to 12 months can occur if packaging design and validation are not given enough focus early in product development initiatives.
“There is a delicate balance between taking time to ensure the quality and package design of your product and increasing your time to market,” he said. “Failure to dedicate the appropriate time and resources during the initial stages of product design can create significant setbacks during validations. Robust design helps prevent failures during validation, and while the product is in the field.”
References
Mark Crawford is a full-time freelance business and marketing/communications writer based in Madison, Wis. His clients range from startups to global manufacturing leaders. He also writes a variety of feature articles for regional and national publications and is the author of five books.