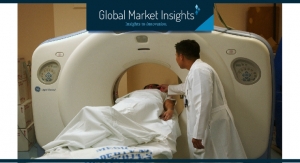
Although 2012 was a tough year for innovation, savvy medical technology companies invested in research and development in the ear, nose and throat (ENT) market, and saw opportunity in the underserved patient population that suffers from sinus disease. According to the American College of Allergy, Asthma and Immunology, sinus disease is a health issue that affects 31 million people in the United States.1 It is estimated that greater than $1 billion is spent each year on over-the-counter (OTC) medications to treat U.S. patients with sinus disease, and that it is attributable to 16 million physician visits, with $150 million spent on prescription medications. Most at risk are patients with allergies, asthma, nose or sinus blockages, or patients with weak immune systems.
Another Large Underserved Patient Population
Acute bacterial sinusitis is an infection of the sinus cavities. It occurs when the sinuses become inflamed and are unable to drain, leading to congestion and infection. Bacterial sinusitis requires a trip to the doctor for diagnosis and treatment to cure the infection and prevent future complications. Up until 2005, the options to treat sinusitis were OTC nasal sprays or drops, antibiotics or sinus surgery.2 Physicians recommend avoiding prolonged use of nasal sprays and drops, and also are concerned about antibiotic resistance, which can cause many common infections such as sinusitis, to be more challenging to treat. Untreated chronic sinusitis can cause damage to the sinuses that sometimes requires surgery to repair. In 2005, balloon dilation technology (BDT), also called balloon sinuplasty, was launched as a less-invasive alternative to functional endoscopic sinus surgery (FESS) for patients with chronic sinusitis. As seen in every market where new disruptive technology is introduced, early adopters and mainstream practitioners clashed on the podium over the clinical outcomes of the two procedures.
Improved Outcomes Through Medical Technology
There is much at stake in the sinus surgery market. Procedure volumes for diagnostic and interventional endoscopy are a critical source of income for the ENT market.
A recent retrospective clinical study of 70 patients with chronic rhinosinusitis was conducted to compare BDT to FESS outcomes.4
|
|
|
|
The following factors were measured:
- Elimination of symptoms;
- Patient satisfaction;
- Post-operative narcotic use; and
- Cost.
Less Invasive Procedures, Improved Clinical Outcomes and Lower Costs
SNOT-20 scores indicated that while BDT and FESS both had clinically meaningful outcomes, patient satisfaction was higher and postoperative narcotics usage was reduced with BDT. The cost for primary procedures was similar, whereas the cost for revision surgery using BDT was lower. The incidence of recurrent sinus infections during the follow-up period was similar for both groups. Only one patient in the BDT group required a repeat intervention within the three-month follow-up period. While long-term efficacy and final cost of BDT still needs to be studied, the less-invasive BDT shows great appeal.
Less Invasive, Lower Cost, More Convenient for Patients
For the most part, a sinus infection is not life threatening, but it is painful and debilitating. According to an editorial in Current Allergy and Asthma Reports, BDT has allowed many ENT surgeons to treat the sinus patient earlier in the disease cycle than is commonly recommended for FESS.6 This is due to its lower morbidity and the opportunity to perform BDT procedures in the office using local and topical anesthesia.
References:
- www.acaai.org/allergist/allergies/Types/sinusitis-sinus-infection/Pages/default.aspx
- Current Allergy and Asthma Reports (2013), 13:250–254
- Medtech Insight, November/December 2012
- Functional Endoscopic Dilatation of the Sinuses: Patient Satisfaction, Postoperative Pain, and Cost, American Journal of Rhinology, Vol. 22, No. 2, March/April 2008, pp. 204-209(6)
- Ibid
- Current Allergy and Asthma Reports (2013), 13:250–254
Maria Shepherd, founder of Data Decision Group, has 20 years of leadership experience in medical device and life-sciences marketing. Following a career including serving as vice president of marketing for Oridion Medical; director of marketing for Philips Medical; and senior management roles at Boston Scientific Inc., she founded Data Decision Group. Her firm quantitatively and qualitatively sizes opportunities, evaluates new technologies, and assesses prospective acquisitions for medtech companies. Shepherd teaches marketing and product development courses and recently was appointed to the board of the MSBiV Medtech Investment Committee. She can be reached at (617) 548-9892 or mshepherd@ddecisiongroup.com.