A panel of advisers to the U.S. Food and Drug Administration recommends that plastic surgical mesh—a trouble-prone medical product widely used to surgically repair women's pelvic problems —needs more stringent tests for safety and effectiveness.
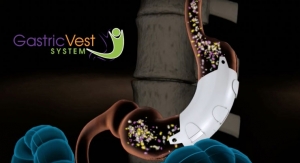
The mesh is used to repair pelvic collapse.
If the FDA agrees with the recommendation, manufacturers would be required to prove the safety and effectiveness of the products before they could continue to market them. The process, however, could take several years.
Consumer groups want the agency to issue a recall now, but medical device manufacturers say mesh offers important advantages in the hands of a trained surgeon, and the rate of serious complications is low.
An FDA review found problems that include pain, bleeding and infection, prompting the agency to warn patients and doctors. Some women have needed multiple surgeries to remove the mesh.
Safety concerns could prompt a shift back to traditional surgery with stitches to repair what is known as pelvic prolapse, a common condition affecting older women. Weakness of the muscles and tissues in the pelvic area allows the bladder, reproductive organs or rectum to bulge or slip into the vagina. The agency is considering reclassifying the mesh products for pelvic collapse, an action that would require the manufacturers to submit evidence of safety and effectiveness in order to continue to market.
The mesh products, which are made by several companies including C.R. Bard Inc., Boston Scientific Corp. and Johnson & Johnson.
Mesh products initially were seen as a high-tech improvement over traditional surgery, which also can have complications. Since similar mesh already was used in other types of surgery, the products received approval from the FDA without the tests that could now be required. Mesh was thought to make repairs last longer.
In July, the FDA issued a mea culpa, saying it was mistaken in its initial assessment that safety issues with mesh for pelvic collapse were rare. The agency said 10 percent of women experienced erosion or exposure of the mesh within 12 months of their initial surgery. More than half of these women required follow-up surgery to remove the mesh. Some required two or three surgeries. At the same time, the FDA said it saw no evidence that using mesh led to better outcomes than traditional surgery with stitches.
"If they had done studies on this product in the first place, we wouldn't be in this situation," said Diana Zuckerman, president of the National Center for Women and Families, a consumer group for women's health issues.
The FDA also is reviewing the use of mesh to treat urinary incontinence. But, according to the agency, there have been fewer complications among incontinence patients than among those who underwent surgery for pelvic collapse.
Between 2008 and 2010 the agency received more than 1,500 reports of complications from women undergoing vaginal prolapse surgery with mesh, up 500 percent from the prior three years. There were fewer complications among incontinence patients.