Jennifer Whitney10.20.06
Bringing Together the Best of Both Worlds
Combination Products Can Offer Better Medical Solutions,
Ease Patient Compliance and Improve Manufacturers’ Profits
Jennifer Whitney
Editor
In the medical device industry, the word “innovative” often finds its way into descriptions about many of the latest products on the market. According to a dictionary, this adjective is defined as “ahead of the times” or “being or producing something like nothing done or experienced or created before.” While it’s easy to overuse this term when describing many of today’s medical products, never has a product category been so characteristic of the word “innovative” than has been seen in the combination product market.
“The combination market helps companies create new market share by creating new applications—it’s attractive to both medical device and pharmaceutical companies, who are partnering and collaborating on these ventures,” said Christine Ford, conference director for Norwalk, CT-based Reed Life Sciences, creator of the upcoming PharmaMedDevice conference to be held next April. “What keeps us excited is that it seems in the past you had industries working in a silo, and now it comes down to patient care and the integration of these products. At the end, in the not-so-distant future, the sum of the whole, rather than the individual parts, will truly benefit patients.”
Indeed, numbers show a trend that is turning into much more than a fad. According to reports from BCC Research and Business Communications Co. Inc., the combination market is estimated to grow by 13.6% annually, reaching $11.5 billion in 2010, compared with $5.4 billion in 2004.
The number of FDA reviews for these products has increased as well. Between 2004 and 2005, the number of products under review by the agency increased by 10%, from 249 to 275.
Aside of the profitability margins this category affords device and pharmaceutical companies, other factors are contributing to the growth of this market. As the cost of healthcare continues to escalate, hospital stays are shortening and there is a greater focus on giving patients a more active role in their healthcare through self-administration of treatments. Reduced toxicity, fewer side effects, higher efficacy and better patient compliance all can be gained by some of the newer combined products on the market.
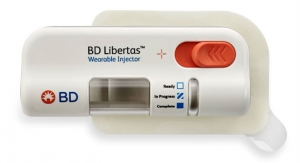
“Patient compliance and comfort have become a bigger issuer than in the past. We want to make products that are easier to administer. When you’re doing this, you want products that are more ergonomic and intuitive to make them easier for a patient to self-administer,” explained Mike Treadaway, manager of the drug delivery devices division for Scottsdale, AZ-based The Tech Group, a West Pharmaceuticals company that manufactures the delivery component for Exubera, an inhaled insulin that was launched earlier this year.
Combined Innovation
While products such as Exubera captured much of the press attention this year—just as drug-eluting stents did when they were introduced in 2003—it should be noted that convergent technology has been around a long time. For example, prefilled syringes may not be the prime example of revolutionary combination products, and they certainly don’t present many controversial issues in the form of regulatory affairs, but nonetheless, they reinforce that combination products are nothing new to the medical device or pharmaceutical industries.
This burgeoning market has gained increasing amounts of attention, though, as the device and biopharmaceutical industries come up with products unlike anything seen in the past. For example, the orthopedic industry already is benefiting from implants combined with biologics that facilitate bone regeneration and, thus, implant stability. And, of course, one of the first noticeable splashes in the industry was the introduction of drug-eluting stents, which employ a coating that can help prevent stenosis that has been known to occur after a stent is placed in the body. Cordis’ introduction of its Cypher sirolimus-eluting stent in 2003 was followed by various other varieties of this type of technology and, eventually, the combination version of stent products had captured 90% of the stent market, according to research by Millennium Research Group.
In coming years, everything from pain management to oncology, migraines and neurologic disorders is expected to benefit from convergent technology. Following are a few other examples of what has been recently approved by the FDA or is on the horizon.
Inhalable medicine. As this year’s launch of Exubera and the 2003 approval of FluMist (a flu vaccine administered as a nasal spray) showed, the use of a medical device to deliver medicine via the pulmonary route is expected to open up a significant new market. While biopharmaceutical companies dream up the next concept for a product that doesn’t involve pills or painful injections, they will increasingly partner with device manufacturers to design and produce the component that delivers the drug.
Nanotechnology. Mark Kramer, director of the FDA’s Office of Combination Products, believes this is one area where drug delivery will see a great impact in future applications, as this type of technology will enable greater capabilities for medicine in general. Ford, who agreed with Kramer’s assessment, cited implantable microchips as an example of products being developed for improved drug delivery.
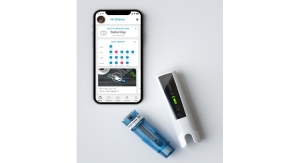
Tiny microchips with drug-filled wells on them are currently in development for use with a remote-controlled device that remains outside the body. “For example, if you have a medicine that needs to be delivered at 10 am, the patient can just hit a button on the remote and it will send a signal to have the microchip deliver the drug,” Ford explained.
Transdermal patches and iontophoretic drug delivery systems. While they aren’t necessarily new, the traditional patches—already well known for delivering nicotine to smokers trying to quit, etc.—are now helping improve compliance among children being treated for attention deficit hyperactivity disorder (Daytrana) or easing dosing regimens in adults with depression (Emsam).
Even more impressive is that developers are expanding the limits of transdermal drug delivery by employing energy sources such as ultrasound, heat and electrical current to affect active transport through the skin, according to Amherst, NH-based Greystone Associates, which recently completed a survey to analyze this market. According to Kramer, expect to see more iontophoretic drug delivery systems, which incorporate patches with electrodes that help deliver more consistent doses of analgesia (or other drug) medications.
“It’s a pretty cool product,” Kramer said. “For some time, we’ve had transdermal patches and iontophoretic therapy. We’ve even had patient-controlled analgesia. This newest product is a self-contained unit that isn’t IV controlled, eliminating the need for painful injections or even possibly less-effective topical analgesic treatments.”
Regulating Innovation
As new frontiers in device/drug pairings are explored, one challenge manufacturers are encountering after they come up with the next brilliant idea in the “combo” realm is figuring out which branch of the FDA would be most likely to review the product. Since each component may be regulated by a different branch within the agency, it’s not always a clear path in determining who will evaluate the product.
That’s not to say some strides haven’t been made. In accordance with the Medical Device User Fee and Modernization Act of 2002, the FDA established its Office of Combination Products (OCP) that year. While the office doesn’t evaluate the products submitted for approval, it does serve as a facilitator and coordinator of the review process by answering questions and helping to determine which branch of the FDA would best evaluate a product.
That type of determination isn’t simple, either. Generally, the OCP evaluates what the product’s primary mode of action is and assigns the review to the center with primary jurisdiction over that component.
Since any manufacturer hoping to bring a new product to market faces both time and money issues, it’s important to try to figure out as quickly as possible which FDA center will have jurisdiction over review of the product. If the manufacturer has a solid understanding up front about how the technology will be regulated, a sound regulatory approach can be formulated during the early development phases.
The more common questions Kramer fields on a daily basis relate to issues that have not, to date, had a firm precedent from which to form sound conclusions regarding best practices, etc. Many device manufacturers (and their pharmaceutical co-contributors) aren’t sure what issues are likely to impact the approval or production of a new combination product.
For example, in cases in which Center for Drug Evaluation and Research (CDER) will be the center overseeing the approval process, many device manufacturers want to know if, and how much, the Center for Devices and Radiological Health will be involved as well.
“Anything from A to Z where they differ, we get questions about. Our charge has been to handle these issues,” Kramer noted.
In previous years, Kramer said most submissions for combination products came from the device industry, thanks to technology such as drug-eluting stents or products with coatings. In the FDA’s last fiscal year, however, he has found that submissions are slightly higher from the pharmaceutical sector.
While the OCP tends to agree with 75% of the manufacturers’ perceived proper designation for which center should review a product, Kramer said some companies have approached the OCP with a preference based on perceived differences among the different centers when it comes to their individual regulatory process. “Some feel the device process is easier, while others prefer the drug center because they are more familiar with CDER’s processes,” he explained.
With any new technology, challenges are bound to arise. In the FDA’s case, these have come in the form of criticisms regarding its approach to combination products, which tend to have their own myriad issues related to the need for various marketing applications, GMP regulations and adverse-event reporting requirements due to the differing components. Concerns include the assignment process, management of the review process when two or more branches of the agency are involved, post-market regulatory controls and lack of clarity regarding certain policies for these products.
“Our objective has been to make the process more transparent. We’ve continued to refine our processes, and we’re making the process about as efficient as we can get it,” Kramer said, additionally noting that the timing to receive approval has been cut down from an average of 60 days to about 30 to 40 days.
To further clarify issues that have arisen since the OCP was formed, in September 2006 the FDA released a guidance document, Early Development Considerations for Innovative Combination Products. Notably, the FDA encouraged developers of convergent technology to “carefully consider the effect of the manufacturing methods on the interaction of the constituent parts.” One example provided was that stability of a combination product as a whole may differ from that of each component; in addition, sterilization issues can be more tricky, since what can be effective for a device component may unintentionally alter the drug or biologic component.
Kramer’s advice for navigating the FDA’s regulatory system for combination products is simple: “Do your homework. Read everything we have made available, since that’s why we’re doing this—to provide information. Once you understand the process, get involved early and consult with us often. Make sure your thinking is sound and readjust, if necessary. If you thought something should be regulated as a drug and we think it’s more of a device, or vice versa, you will need to know that early on.”
Collaboration Issues
Just as outsourcing often comes down to a matter of a company choosing to focus on core competency, most device manufacturers aren’t looking to make a drug in-house and most pharmaceutical companies don’t have medical device engineering knowledge. Therefore, strategic partnerships or licensing agreements are the typical approach to bringing new products to market.
In addition, Minneapolis, MN-based Medtronic and Cambridge, MA-based Genzyme took the idea of collaboration one step farther in June 2004 when they formed a joint venture, MG Biotherapeutics, LLC. The companies have stated that they formed this entity to develop cell-therapy treatments for heart disease that leverage each company’s complementary strengths through the combination of biologics and delivery devices.
To address the needs of the growing number of companies interested in the combination market, Reed Life Sciences, a division of Reed Exhibitions, Inc., will launch PharmaMedDevice on April 24-26, 2007 in New York City (visit www.pharmameddevice.com for more information). After realizing there was no single event that was fully serving the needs of the burgeoning convergent technology industry, Reed decided to design an event that will cover everything from regulatory to manufacturing issues, along with protecting intellectual property, overcoming international issues and forming successful collaborations—and, of course, the spotlight will shine on the plethora of new products.
“It’s important to point out that this is an evolving industry,” Ford said. “Companies can be challenged to find partners. One of the reason we created this conference is to fulfill this type of need, educating the industry and helping companies find partnerships and understand the unique regulatory environment.”
As Treadaway from The Tech Group can attest, this market is very complex—but it’s also very rewarding, since the bottom line is that it’s all about the people (ie, patients) benefiting from these products.