Sam Brusco, Associate Editor08.07.23
Masimo released findings of a study published in Frontiers in Neuroscience, in which Dr. Lichy Han and colleagues at Stanford University analyzed Masimo SedLine brain function monitoring to assess sedation levels of patients undergoing drug-induced sleep endoscopy (DISE) with the sedative dexmedetomidine.
The researchers discovered Masimo’s Patient State Index (Psi), a SedLine parameter derived from electroencephalographic (EEG) data, was “statistically significantly associated” with dexmedetomidine dosage. They also found along with another EEG metric, “better captured changes in brain state from dexmedetomidine and ha[s] potential to improve the monitoring of dexmedetomidine sedation.”
The researchers noted while anesthesia induced with dexmedetomidine might more closely mimic sleep compared to other sedatives, its effects on the brain are inconsistent, which has historically limited its use. They posited that better understanding of sedation’s impact and corresponding EEG changes could support more widespread adoption of the drug.
The researchers sought to compare and evaluate various methods of assessing sedation in such a scenario. With regard to the choice of EEG markers, they noted “Previous EEG markers, such as the bispectral index, have been unable to determine differences elicited with dexmedetomidine (Kaskinoro et al., 2011), thus motivating the discovery of novel EEG markers associated with changes in brain state seen with dexmedetomidine sedation.”
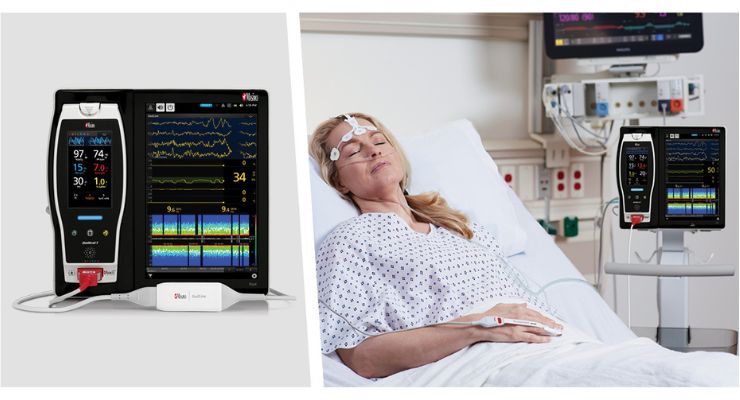
51 patients undergoing DISE were enrolled for diagnosis and potential treatment of obstructive sleep apnea. They were sedated with dexmedetomidine and continuously monitored using SedLine.
The researchers observed that RASS scores decreased with increasing dexmedetomidine concentration but noted that, “Overall, the RASS score was least able to capture the brain state changes seen with dexmedetomidine, suggesting other metrics for titrating dexmedetomidine sedation may be of greater value.” They found that PSi, SEF95, and CD all decreased statistically significantly with increasing dexmedetomidine concentration (p < 0.001, p = 0.006, and p < 0.001, respectively), “a clear dose-dependent decrease with an inflection point.”
Study lead authors Lichy Han, MD, Ph.D. and David Drover, MD, Perioperative and Pain Medicine at Stanford University, told the press, “This study provides one more step in the journey to understanding SedLine processed EEG parameters that can guide sedation levels. In this case, dexmedetomidine, a widely used sedative, which has not been fully characterized by processed EEG, was titrated using standard indices PSi, SEF95, as well as fractal dimension (CD) commonly applied to time series data like EEG. In contrast to BIS, SedLine parameters (particularly PSi) were able to characterize processed EEG changes that correlated with dexmedetomidine sedation level and concentration, and these parameters correlated better than the subjective measure RASS (the most widely used clinical measure of sedation depth). This work helps clinicians use SedLine as an objective measure reflecting how the brain is responding to this important sedative, dexmedetomidine.”
The researchers discovered Masimo’s Patient State Index (Psi), a SedLine parameter derived from electroencephalographic (EEG) data, was “statistically significantly associated” with dexmedetomidine dosage. They also found along with another EEG metric, “better captured changes in brain state from dexmedetomidine and ha[s] potential to improve the monitoring of dexmedetomidine sedation.”
The researchers noted while anesthesia induced with dexmedetomidine might more closely mimic sleep compared to other sedatives, its effects on the brain are inconsistent, which has historically limited its use. They posited that better understanding of sedation’s impact and corresponding EEG changes could support more widespread adoption of the drug.
The researchers sought to compare and evaluate various methods of assessing sedation in such a scenario. With regard to the choice of EEG markers, they noted “Previous EEG markers, such as the bispectral index, have been unable to determine differences elicited with dexmedetomidine (Kaskinoro et al., 2011), thus motivating the discovery of novel EEG markers associated with changes in brain state seen with dexmedetomidine sedation.”
51 patients undergoing DISE were enrolled for diagnosis and potential treatment of obstructive sleep apnea. They were sedated with dexmedetomidine and continuously monitored using SedLine.
The researchers observed that RASS scores decreased with increasing dexmedetomidine concentration but noted that, “Overall, the RASS score was least able to capture the brain state changes seen with dexmedetomidine, suggesting other metrics for titrating dexmedetomidine sedation may be of greater value.” They found that PSi, SEF95, and CD all decreased statistically significantly with increasing dexmedetomidine concentration (p < 0.001, p = 0.006, and p < 0.001, respectively), “a clear dose-dependent decrease with an inflection point.”
Study lead authors Lichy Han, MD, Ph.D. and David Drover, MD, Perioperative and Pain Medicine at Stanford University, told the press, “This study provides one more step in the journey to understanding SedLine processed EEG parameters that can guide sedation levels. In this case, dexmedetomidine, a widely used sedative, which has not been fully characterized by processed EEG, was titrated using standard indices PSi, SEF95, as well as fractal dimension (CD) commonly applied to time series data like EEG. In contrast to BIS, SedLine parameters (particularly PSi) were able to characterize processed EEG changes that correlated with dexmedetomidine sedation level and concentration, and these parameters correlated better than the subjective measure RASS (the most widely used clinical measure of sedation depth). This work helps clinicians use SedLine as an objective measure reflecting how the brain is responding to this important sedative, dexmedetomidine.”