Business Wire05.06.16
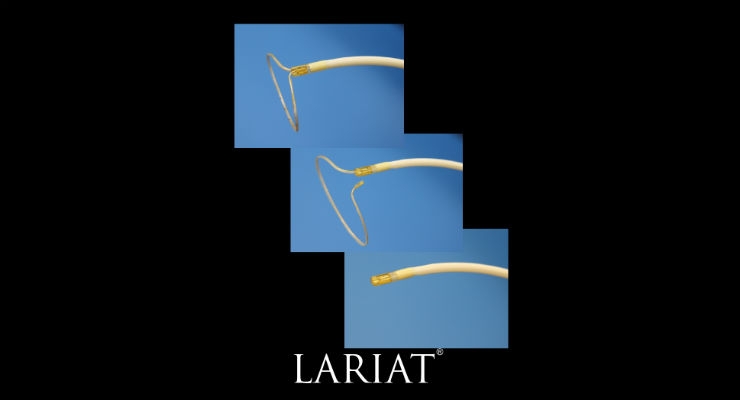
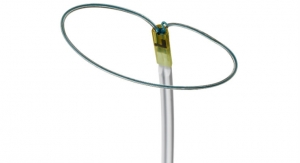
SentreHeart Inc. has received 510(k) approval for the LARIAT XT, the latest in a family of soft tissue closure devices, designed to offer remote suture delivery for immediate, complete closure, with no metal, clip, or implant left behind. The LARIAT XT incorporates a variety of enhancements, including a fully retractable snare designed to facilitate ease-of-operator use and potentially expand its applicable anatomic range.
The LARIAT XT offers precise, user controlled remote delivery of a pre-tied suture loop that is compatible with a wide range of anatomical shapes and sizes up to 45mm in width.
The Lariat XT will compliment the Lariat+, currently being used in the recently FDA IDE approved aMAZE study, which is intended to demonstrate that a LARIAT procedure for LAA closure, plus a subsequent PVI ablation will lead to a reduced incidence of recurrent AFib compared to PVI alone; with a high safety profile. The study plans to enroll a maximum of 600 persistent or longstanding persistent patients who are candidates for PVI catheter ablation at up to 50 centers.
The aMAZE Study
The aMAZE Trial is a FDA approved, multicenter, randomized control trial that is assessing the safety and efficacy of the LARIAT left atrial appendage closure procedure combined with pulmonary vein isolation (PVI) compared to PVI ablation only in patients with persistent or longstanding persistent atrial fibrillation. The primary outcome being assessed is freedom from AFib at one year.
PVI Catheter ablation is the standard of care in the management of drug-refractory symptomatic AFib. However, the success rates of PVI ablation are less than ideal, especially in patients with persistent AFib.1 Current data suggests that a single ablation procedure of the pulmonary veins (PV) for treating AFib results in success rates of only 20-40 percent.
The left atrial appendage (LAA) has been shown to play a role in the initiation and maintenance of atrial arrhythmias and is the source of most stroke-causing blood clots (thrombus) in AFib patients.2 A recent study by Dibiase, et al showed that nearly 30% of AFib patients returning for repeat ablation procedures had abnormal electrical activity that included the LAA as its source. Studies have demonstrated that the LARIAT device not only closes the LAA mechanically3 but may also isolate electrical activity within the LAA4.
1 Lakkareddy D, et al. Left Atrial Appendage Ligation and Ablation for Persistent Atrial Fibrillation, JACC: Clinical Electrophysiology 2015; VOL. 1, NO. 3.
2 Manning WJ. Atrial fibrillation, transesophageal echo, electrical cardioversion, and anticoagulation. Clin Cardiol. 1995; 18: 58,114.
3 Bartus K, et al. Percutaneous Left Atrial Appendage Suture Ligation Using the LARIAT Device in Patients with Atrial Fibrillation. J Am Coll Cardiol 2013 Jul 9;62(2):108-18.
4 Han FT, et al. The Effects of LAA Ligation on Electrical Activity. Heart Rhythm. 2014 May; 11(5):864-70.
The LARIAT XT offers precise, user controlled remote delivery of a pre-tied suture loop that is compatible with a wide range of anatomical shapes and sizes up to 45mm in width.
The Lariat XT will compliment the Lariat+, currently being used in the recently FDA IDE approved aMAZE study, which is intended to demonstrate that a LARIAT procedure for LAA closure, plus a subsequent PVI ablation will lead to a reduced incidence of recurrent AFib compared to PVI alone; with a high safety profile. The study plans to enroll a maximum of 600 persistent or longstanding persistent patients who are candidates for PVI catheter ablation at up to 50 centers.
The aMAZE Study
The aMAZE Trial is a FDA approved, multicenter, randomized control trial that is assessing the safety and efficacy of the LARIAT left atrial appendage closure procedure combined with pulmonary vein isolation (PVI) compared to PVI ablation only in patients with persistent or longstanding persistent atrial fibrillation. The primary outcome being assessed is freedom from AFib at one year.
PVI Catheter ablation is the standard of care in the management of drug-refractory symptomatic AFib. However, the success rates of PVI ablation are less than ideal, especially in patients with persistent AFib.1 Current data suggests that a single ablation procedure of the pulmonary veins (PV) for treating AFib results in success rates of only 20-40 percent.
The left atrial appendage (LAA) has been shown to play a role in the initiation and maintenance of atrial arrhythmias and is the source of most stroke-causing blood clots (thrombus) in AFib patients.2 A recent study by Dibiase, et al showed that nearly 30% of AFib patients returning for repeat ablation procedures had abnormal electrical activity that included the LAA as its source. Studies have demonstrated that the LARIAT device not only closes the LAA mechanically3 but may also isolate electrical activity within the LAA4.
1 Lakkareddy D, et al. Left Atrial Appendage Ligation and Ablation for Persistent Atrial Fibrillation, JACC: Clinical Electrophysiology 2015; VOL. 1, NO. 3.
2 Manning WJ. Atrial fibrillation, transesophageal echo, electrical cardioversion, and anticoagulation. Clin Cardiol. 1995; 18: 58,114.
3 Bartus K, et al. Percutaneous Left Atrial Appendage Suture Ligation Using the LARIAT Device in Patients with Atrial Fibrillation. J Am Coll Cardiol 2013 Jul 9;62(2):108-18.
4 Han FT, et al. The Effects of LAA Ligation on Electrical Activity. Heart Rhythm. 2014 May; 11(5):864-70.